A member of the Poxviridae family of orthopoxviruses, the monkeypox virus, is the causative agent of monkeypox, The Democratic Republic of the Congo (DRC), where the disease is thought to be endemic, is one of the most common locations where it occurs in Central and West African nations. 1958,1959,1962,2003 were the years when monkeypox virus outbreaks seen. In 2022, four MPXV cases were found in India as well. Congo Basin clade of MPXV is more infectious and attenuated than West African clade. In the case of the typical human MPV disease, symptoms such as fever, malaise, headaches, and lymphadenopathy start to manifest 4–17 days after the exposure. The primary method of confirming MPV infection is a positive test for Polymerase Chain Reaction (PCR) of swabs from lesions of skin or mucosa or scabs. A confirmatory test is also performed if a PCR of a blood sample or Cerebrospinal Fluid (CSF) yields positive results. supportive care is the core of treatment for mild cases, with an emphasis on pain management, hydration, nourishment, and avoiding bacterial superinfection of skin lesions. Lesions on the skin need to be kept dry and clean. Both topical petroleum jelly and oral antihistamines are effective treatments for pruritis. To prevent MPV infection, people must avoid close contact with those who are thought to be infected because they may be contagious To reduce transmission and to expand understanding of disease burden, surveillance has to be improved. Since eradication is impossible due to the cycle’s sylvatic component, prevention becomes crucial as it can be controlled by preventing MSM and isolating oneself who got infected with MPXV. This review gives information about Monkeypox virus, it’s epidemiology, virology, pathophysiology, how it can be transmitted, symptoms, prevention and management.
Monkeypox, Democratic Republic of Congo, West Africa, Polymerase Chain Reaction, Orthopoxvirus, MSM
A member of the Poxviridae family of orthopoxviruses, monkeypox virus,- is the causative agent of monkeypox, an uncommon, sporadic, smallpox-like zoonotic infectious illness.1,2 The Democratic Republic of the Congo (DRC), where the disease is thought to be endemic, is one of the most common locations where it occurs in Central and West African nations.3 Monkeypox virus is most commonly contracted by children between the ages of 5 and 9,4 especially in small communities where youngsters hunt and eat squirrels and many other small mammals. Individuals with a history of travelling to Africa have been documented to have imported cases in the Singapore, United States, and Israel.5
First MPXV Outbreak in Denmark (1958)
In 1958, a nonfatal outbreak of MPXV was reported at a Copenhagen, Denmark, animal facility. Outbreak occured in Rhesus macaques (Macaca mulatta) and Asian monkeys (mainly M. fascicularis) that were regularly supplied from Singapore, to the institution for research in polio vaccine. 2 months after the delivery of the monkeys, the first episode began, and four months later, the second As soon as arrival of monkeys, they were treated with antibiotics and appeared to be in satisfactory health. The outbreak manifested itself with vesiculopustular skin eruptions.6
MPXV Outbreak in the USA (1959)
In the same year i.e 1959 the Von Magnus et al.7 report, a second MPXV outbreak in a colony of captive monkeys in Philadelphia, USA, was also documented. This outbreak affected small numbers of animals of both ages and both sexes. Species affected were Macacus Rhesus and Macacus Cynomolgus. Clinical symptoms noted were rashes developing into a maculopapular eruption, associated with itching. Lesions could be seen over the body most abundantly in limbs. Papules were thick with pus formation. Some monkeys were left for observation for around two months and the lesions were first covered with crust and later fell off as healing proceeded. However, it was difficult to estimate the specific number of ill animals because of the vast numbers of animals in a given cage and the difficulty to inspect every animal.8
MPXV Outbreak in the USA (1962)
In two M. fascicularis monkeys the USA reported a second MPXV outbreak roughly 45 days following whole-body radiation treatment.9 Clinically, the lesions resembled those described by Prier et al. and Von Magnus et al.7,10 including pox-like eruptions, severe facial and cervical edema, hemorrhagic ulcerations, dyspnea, and bloody diarrhoea. After 12 days, both afflicted monkeys passed away. One nonirradiated monkey developed cervical edema and had ulcerated skin on its limbs and forehead, but it lived.6
MPXV Outbreak in Central and Western Africa (1970)
In the 1970s, the first human cases of MPV illness was discovered in Central and Western Africa, mostly in children who had a diffuse vesiculopustular rash, lymphadenopathy, and fever. The Congo Basin saw the majority of the succeeding decades’ hundreds to thousands of new human MPV disease cases.11
MPXV Outbreak in the USA (2003)
The importation of rodents from Ghana and Washington led to the occurrence of a third MPXV outbreak in the USA. Native prairie dogs, kept next to the African rodents, were later infected by infected animals. The first reported instance of human monkeypox (MPX) outside of Africa was caused by prairie dogs, which tested to be highly susceptible to the virus and spread MPXV to about 40 people. Clinical symptoms included rashes over the body, coughing, sneezing, ocular discharge and swollen eyelids.12,13
Epidemiology
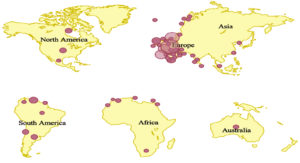
In more than 90 countries in Europe, the Americas, the Eastern Mediterranean, the Western Pacific, and Southeast Asia, there were over 45,000 confirmed and suspected cases of monkeypox as of August 29, 2022, according to the World Health Organization. The abundance of disease can be seen in Figure 1. Future predictions include more instances as well. In 1970, a 9-month-old child from Zaire (now the DRC) became infected with MPXV, the first human infection reported in history. Since then number of human monkeypox cases has been increasing. There is no doubt that the deadly monkeypox disease may spread between people in Central Africa.14,5
Adult travellers from Nigeria were diagnosed with monkeypox in Israel, the UK, Singapore, and the US between 2018 and 2021; however, each of them had previously visited endemic areas of Central and West Africa. The median age at presentation has increased from 4 (1970s) to 21 years (2010–2019). The majority of recent cases, in sharp contrast to earlier ones, involve community transmission, involve less females and children, and have no known travel connections to endemic areas [the majority of the initial reported cases in males who have sex with other men (MSM)]. Currently, certain countries are reporting instances of community transmission, especially in women and children. This shows that children are also prone to develop monkeypox. The reason for spreading of disease across border could be mutation in virus, stoppage of smallpox vaccination or reduction in human immunity to MPXV.14,5
MPV was ultimately recognised in 1958 when a collection of unique morphological skin eruptions was found in a lab colony of crab-eating macaques in Denmark. In more than 70 nations on six continents, there had been more than 20,000 recorded cases of the human MPV disease by the end of July, with more than 5,000 cases in the US. However, not all of these occurrences were among MSM. Epidemiologic analyses also found that close physical contact, such as skin-on-skin contact or sexual activity, was the most likely method of human-to-human transmission (or associated with foreign travel or the importation of animals from these regions). However, the United Kingdom announced that it has found the disease in May 2022.11 As of July 24, 2022, four MPX instances have been reported in India; the first case had been made public on July 14. All of them were male. In contrast to the previous three patients, who were all from Kerala, the final patient, from Delhi, had never travelled outside of the country before. Re-emergence of monkeypox has been linked to high-risk sexual contact, a changing biological makeup of the virus, climate variability, a decline in immunity following the discontinuation of smallpox vaccination, and increased international travel following the removal of COVID-19 travel restrictions.15
Virology
The family Poxviridae, genus Orthopoxvirus, which contains the variola virus (VARV), monkeypox virus (MPXV), cowpox virus (CPXV), and vaccinia virus, is home to numerous illnesses that can infect humans (VACV). The 200 kb or smaller genomes of these viruses have highly conserved core sections that encode replication and assembly machinery in addition to genes important in pathogenicity and host range determination. Smallpox virus, known as VARV, was only known to infect humans and is projected to encode 20% fewer functional proteins than CPXV.11 Out of all naturally occurring orthopoxviruses, it has the smallest genome (186 kb).
Similar to VARV, MPXV is a very virulent orthopoxvirus that has a 10% case-fatality rate and causes severe illness and death. It is extremely dangerous (30% case fatality rate). Monkeypox is currently a problem on a global level. The MPV’s natural reservoirs are most likely small African mammals like dormice, African rope squirrels, Gambian pouched rats, and primates. The two recognised subclades of MPV, which is indigenous to Central and Western Africa, are a more virulent Congo Basin (Central African) clade and a lesser virulent West African clade.11
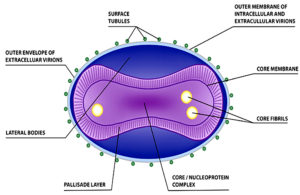
Poxviruses replicate in the cytoplasm of cells from vertebrates. Their genomes are between 130 and 360 kbp in size. Poxviruses do not reproduce and reveal their genes in the nucleus like DNA viruses generally do, which largely depend on cellular proteins. Because they heavily rely on virus-encoded proteins to enable cytoplasmic replication, poxviruses are unusual in this regard.16 49 genes are recognized by all sequenced members of this family and 90 genes are shared by the chordopoxvirus subfamily out of the more than 150 genes encoded by poxviruses. Most of these genes are shared by all viruses and are essential for the viral genome’s functionality. Poxviruses are larger than other viruses, making it more challenging for viruses like monkeypox to penetrate gap junctions and overcome host defences. The structure of Monkeypox virus has been shown in Figure 2. The virus’s larger size also makes it more difficult for it to spread. The larger orthopoxviruses alarm the immune system of the body more early and make it easier to produce an immunological response.17,18 The MPXV virion is an enveloped virus having a brick-like structure and a dumbbell-shaped core that is 200–250 nm in size. The WA (West Africa) and CB (Congo Basin) groups of MPXV have been found through genome sequencing. The genetic make-up and varying levels of pathogenicity of WA and CB MPXVs. Despite the fact that it has been postulated that CB is more infectious and attenuated than WA MPXV. The host’s susceptibility to the virus, the mode of transfer, and the quantity of virus injection can all have an impact on how severe an illness is.17
Pathophysiology
Orthopoxviruses are loaded with a number of proteins that are created by genes and operate as modulators by focusing on immune system components in order to escape the host immune system. Depending on whether they work intracellularly or extracellularly, these proteins that control the host’s immune response can be divided into two groups. Two categories of proteins regulate the modulatory actions against the host’s immune response. Virotransducer and virostealth proteins are two examples of intracellular proteins.18 The oxidative burst and apoptotic pathways, as well as the cell’s ability to respond to the infection, are all blocked by the virotransducer proteins.16,19,20 Virostealth is a protein that decreases the detection of the major histocompatibility complex class 1 (MHC 1) and CD+4 molecules, by downregulating them. As these molecules are responsible for immune recognition so virostealth reduces the ability of immune system to recognise virus.18 Although there are two distinct categories of internal modulatory proteins that help frustrate the host’s immune response, viromimic proteins are the sole type of surface protein discovered in monkeypox. Chemokines move in opposition to and competition with one another. Viral proteins, also referred to as viromimic proteins, act extracellularly and control the immune response. They fall within the categories of viroreceptors and virokines.19,20
Viroreceptors are cell surface glycoproteins that are released or bound collectively by host cytokines and chemokines to block their activities. It is possible for virokines to mimic host cytokines, chemokines, and growth factors in order to defeat host defences that are harmful to the survival of the virus and to foster responses that are beneficial for viral reproduction and dissemination.13
Thus, virokines create viral copies of the host’s cytokines, chemokines, and growth factors that can counteract host defences that are harmful to the survival of the virus and enhance defences that are helpful for viral reproduction and dissemination. These modulatory proteins promote viral replication while also undermining the host’s immune response. If these proteins weren’t present, the immune system could not be evaded by the monkeypox and other orthopoxviruses.21
Transmission
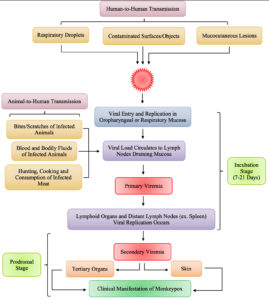
According to recent reports, the MPXV is spreading more frequently from person to person. The pathway for human to human transmission is shown in Figure 3. Seven generations of unbroken human reproduction were documented in the DRC in 2003. It is anticipated that the introduction and spread of MPXV among people will significantly rise when susceptibility increases at the same time that herd immunity declines. A monkeypox pandemic in the Midwest of the United States in 2003 showed how likely it is for MPXV to be transmitted to unaware individuals. As opposed to the Central African strains that are present in the DRC, the MPXV strain in issue belonged to the Western African clade, with less virulent strains.22,23
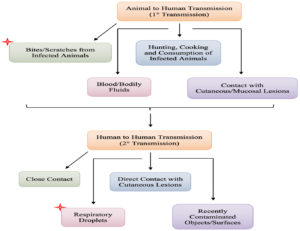
Zoonotic transmission as shown in Figure 4 can occur as a result of direct contact with diseased animals, such as bites, scratches, or the preparation of bushmeat. Direct skin-to-skin (or mucosal) contact with infected wounds, contaminated bedding and clothing, and contaminated respiratory secretions are further ways that human-to-human transmission can occur.24,11
Therapeutic Presentation
In the case of the traditional human MPV disease, symptoms such as fever, malaise, headaches, and lymphadenopathy start to manifest 4–17 days after the exposure. The usual maculopapular rash that follows, which may be unpleasant or itchy, develops into vesiculopustular lesions. These lesions may be umbilicated and are normally well-circumscribed, evolving at a consistent size. They may spread to the mouth, face, trunk, palms, and soles. The disease normally lasts two to four weeks. The normal beginning symptoms have frequently been absent or have appeared after the rash in the most recent MPV disease outbreak, also known as the West African clade.15,25
The anal, vaginal, and oral mucosae (or other surrounding skin areas) are where the rash is supposed to start in this pandemic, and it might not extend to other places. Instances of severe urethritis, pharyngitis, balanitis, and proctitis have also been reported. Lesions have also experienced bacterial superinfections. Patients are regarded as contagious after prodromal or rash signs develop until the sores heal, fall off, and a fresh layer of skin or mucosa grows in their place. Symptoms of syphilis, varicella zoster, herpes simplex, molluscum contagiosum, and acute human immunodeficiency virus may resemble these cutaneous and mucosal sores (HIV).26,27
Monkeypox often has symptoms that may last around two to four weeks and is a self-limiting condition. According to the amount of exposure to virus, the patient’s health, and the difficulties present, children are more likely to have severe instances. It is uncertain how widespread asymptomatic infection is. Among the general population, the standardised death rate of monkeypox has traditionally fluctuated from 0 to 11%; it has been higher in young children. The mortality rate is determined to be between 3 and 6 percent. The most typical symptoms and indicators include fever, lymphadenopathy, chills and/or sweats, sore throat and cough, and rashes. These problems frequently appear within one to three days of the initiation of a fever and last for two to four weeks.
Stages of Rash May Include
Enanthem: first mouth and tongue lesions, Within 24 hours, Macules begin on the face and spread centrifugally to the arms, legs, palms, and soles. There are four stages to the rash: macular, papular, vesicular, and pustular. Lesions turn into papules by the third day, and vesicles by the fourth to fifth day (raised and fluid filled).
Lesions turn pustular, sharply elevated, filled with opaque fluid, firm, and deeply seated by the sixth to seventh day. They dry out and crust towards the end of the second week.28 The incubation period is 5 to 21 days, but it usually lasts between 6 and 13 days. Around all ages are impacted, the middle age has risen over time. More men than women are impacted. Smallpox and other pox virus infections share clinical characteristics.28 The onset phase is nondescript and often lasts 0 to 5 days. Fever, headache, sluggishness, myalgia, and lymphadenopathy are its hallmarks. The commencement of a fever triggers the development of a unilateral or bilateral cervical, axillary, or inguinal lymphadenopathy. The rashes appears, which lasts for 2-4 weeks, happens next. Up until they start to crust, the lesions are polymorphic and are quite painful. Lesions can range in number from one to hundreds.17,21
Diagnosis
The primary method of confirming MPV infection is a positive test for PCR of swabs from lesions of skin or mucosa or scabs.1,2,7 A confirmatory test is also performed if a PCR of a blood sample or CSF yields positive results. Viral culture, while less accurate, can occasionally aid in confirmation. An anti-orthopox virus IgM assay that is positive in the blood or CSF may be a sign of recent MPV infection even if it might not be able to distinguish between recent immunisation and other orthopox viral infections. An anti-orthodox IgM test may also be negative in MPV-infected people who are unable to produce an antibody response. Various tests for diagnosis of the monkeypox virus has been shown in Table.
Table :
Test for confirmation of MPXV.30
Test |
Description |
|---|---|
Viral culture or isolation |
Live viruses are produced and identified using patient specimens. |
Electron microscopy |
For the visual classification of a poxvirus, a better result of a brick-shaped particle was acquired. |
Immunohistochemistry |
determine whether the OPXV-specific antigens are present. |
PCR, including real-time PCR |
To check whether MPXV-specific DNA markers exist |
Anti OPXV IgG |
To determine presence of OPXV antibodies |
Anti-OPXV IgM |
To see the presence of OPXV antibodies |
Tetracore OrthopoxBioThreat Alert |
It tests for the presence of OPXV antigens.30 |
Other diseases like syphilis, varicella zoster, herpes simplex, molluscum contagiosum, or acute HIV should also be taken into consideration because they can mimic MPV or even co-infect with it.11
Management and Treatment
Most MPV infections progress slowly and naturally without the need for specialised antiviral medication. Therefore, supportive care is the core of treatment for mild cases, with an emphasis on pain management, hydration, nourishment, and avoiding bacterial superinfection of skin lesions. Lesions on the skin need to be kept dry and clean. Both topical petroleum jelly and oral antihistamines are effective treatments for pruritis. Anesthetic gels or “magic” mouthwash, which frequently contains antihistamines, steroids, lidocaine, and antimicrobials, can be used to treat oral sores. Topical anaesthetics, NSAIDs, neuropathic pain relievers, or even opiate medicines in severe situations may be used to treat painful genital sores. Proctitis can be treated with sitz baths and stool softeners. Hydration, acetaminophen, NSAIDs, or other well-known acute headache treatments may be used as necessary to treat headaches symptomatically. In addition to being used in an expanded access investigational new drug (EA-IND) regimen for MPV infections, tecovirimat (TPOXX), an antagonist of the orthopox viral VP37 envelope wrapping protein, is a treatment that has been given FDA approval for treating human smallpox virus infection. Orthopox antiviral medicines can be taken into consideration for severe cases, including any potential neuroinvasive signs, even though there are presently no FDA-approved therapies for treating MPV infections.29,11
Cidofovir and brincidofovir are additional antiviral drugs that may have anti-orthopox virus action (inhibitors of various viral DNA polymerases). Although there aren’t any clinical studies to support this yet, intravenous vaccine virus immune globulin (VIGIV) may also be helpful in treating severe MPV infection.15 Imvamune, a third-generation modified vaccinia Ankara (MVA) vaccine, and ACAM2000TM, a second-generation live attenuated immunisation developed from Dryvax®, are not recommended by the CDC. Currently, MPX cases are advised to utilise ACAM2000TM for up to 14 days after exposure to minimise symptoms but not guaranteed to prevent sickness. Since 2007, the USA has been hoarding ACAM2000TM. ACAM2000TM is equivalent to Dryvax® in terms of immunogenicity, but unhappily it also frequently causes cardiac adverse events.29,30
Patients can be managed by isolating them in a space with its own ventilation, covering their compromised skin and mucous membranes, using a triple-layer mask, etc. This also includes monitoring and treating issues, rehydration therapy, and nutritional support.29,30
Prevention
To prevent MPV infection, people must avoid close contact with those who are thought to be infected because they may be contagious. MSM should be more cautious at this time. People who have an MPV infection should avoid crowds and stay at home or in other isolated areas, cover all lesions, wear a mask, and wash or disinfect their hands if they come into touch with sores. Currently, when treating patients with suspected or proven MPV infection, contact precautions are required ( which include eye protection as well). For those who have recently been exposed to MPV (preferably within 4 days) or who are more likely to contract MPV in the future, the CDC also advises vaccination. To isolate cases, stop future transmission, provide the best clinical care, safeguard primary healthcare workers, and implement effective control and preventative measures based on the known channels of transmission, monitoring techniques should be put into place as soon as feasible.31
Outline for Surveillance
(a) Use Standard Case Definitions at Points of Entry and by all District Surveillance Units (DSUs) under the Integrated Disease Surveillance Program (IDSP) (PoEs).
(b) A monkeypox outbreak should be regarded as having even one case. Rapid Response Teams must begin an extensive inquiry through IDSP.
(c) Immediately notify the DSU/State Surveillance Units (SSUs) and CSU (Central Surveillance Unit), who will thereafter notify MoHFW of any suspicious cases.
(d) Send the samples to the specified laboratories in accordance with the instructions.32
Investigations are currently being conducted into rare reports of suspected neuroinvasive MPV illness in this outbreak. For instance, the Spanish Ministry of Health recently reported two cases of neuroinvasive MPV illness that were fatal in two adult males (ages 31 and 44) who had been diagnosed with encephalitis. Animal experiments have also revealed that MPV has neurotropic potential. Multiple instances of infectious virus being found in various animals’ brains. Neurologists should be ready to recognise, detect, and treat any neuroinvasive diseases notwithstanding the frequency of neurological symptoms linked to human MPV infection. This is because there are a growing number of instances of MPV infection around the world. Inquiries regarding travel and possible contacts (including sexual exposures) in the 21 days preceding the beginning of symptoms should be made of suspected MPV disease cases. World Health Organization (WHO) website include the most recent information for patients and medical professionals. Low MPX incidence has been made possible by smallpox immunisation. Re-emergence has been caused by people that depend on hunting for food and a younger, non-immune generation. Immunocompromised people should not receive the smallpox vaccine. MVA vaccines are still being developed, but complete licensure of antiviral therapy options to support preventative efforts should be taken into consideration. The USA outbreak demonstrated MPXV’s ability to infect and significantly increase morbidity in a variety of hosts globally. A large mortality rate has indicated that the CB clade has been more aggressive. Due to globalisation, nations cannot disregard infectious pathogens that were previously thought to be restricted to specific geographic areas. The emergence of cases outside Africa indicates the high risk for geographical spread and the global relevance of the disease. Further investigation to discover the reservoir hosts and focused educational programmes are required in view of environmental impacts to safeguard those who are most vulnerable. International funding is necessary for mass surveillance and case detection to better understand the epidemiology of this emerging sickness, which is constantly changing.
ACKNOWLEDGMENTS
None.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
All authors listed have made a substantial, direct and intellectual contribution to the work, and approved it for publication.
FUNDING
None.
AVAILABILITY OF DATA
All datasets generated or analyzed during this study are included in the manuscript.
ETHICS STATEMENT
Not applicable.
- Sklenovska N, Van Ranst M. Emergence of monkeypox as the most important orthopoxvirus infection in humans. Front Public Health. 2018;6:241.
Crossref - Mccollum AM, Damon IK. Human monkeypox. Clin Infect Dis. 2014;58(2):260-7.
Crossref - Durski KN, McCollum AM, Nakazawa Y, et al. Emergence of monkeypox—west and central Africa, 1970–2017. Morbidity and mortality weekly report. 2018 Mar 16;67(10):306.
Crossref - Emergence of monkeypox–West and Central Africa, 1970–2017. MMWR Morb Mortal Wkly Rep. 2018;67:306–10.
Crossref - Dou YM, Yuan H, Tian HW. Monkeypox virus: past and present. World J Pediatr. 2022:1-7.
Crossref - Parker S, Buller RM. A review of experimental and natural infections of animals with monkeypox virus between 1958 and 2012. Future Virol. 2013;8(2):129-157.
Crossref - Von Magnus P, Andersen EK, Petersen KB, Birch-Andersen A. A pox-like disease in cynomolgus monkeys. Acta Path Micro Scand. 1959;46(2):156-176.
Crossref - Sauer RM, Prier JE, Buchanan RS, Creamer AA, Fegley HC. Studies on a pox disease of monkeys. I. Pathology. Am J Vet Res. 1960;21:377-380.
- Prier JE, Sauer RM. A pox disease of monkeys. Ann NY Acad Sci. 1960;85:951-959.
Crossref - Hutson CL, Lee KN, Abel J, et al. Monkeypox zoonotic associations: insights from laboratory evaluation of animals associated with the multi-state US outbreak. Am J Trop Med Hyg. 2007;76(4):757-768.
Crossref - CDC. Update: multistate outbreak of monkeypox – Illinois, Indiana, and Wisconsin, 2003. Mort Morb Wkly Rep. 2003;52(27):642-646.
- World Health Organization. Multi-country monkeypox outbreak: situation update. 2022. https:// www. who. int/ emerg encies/ disease-outbr eak- news/ item/ 2022- DON392. Accessed June 10, 2022.
- World Health Organization. Monkeypox outbreak: global trends. 2022. https:// world healt horg. shiny apps. io/ mpx_ global/. Accessed Aug 29, 2022.
- Kozlov M. How does monkeypox spread? What scientists know. Nature. 2022;608(7924):655-656.
Crossref - CDC. Monkeypox. 2022. https://www.cdc.gov/poxvirus/ monkeypox/index.html. Accessed July 30, 2022.
- Pastula DM, Tyler KL. An overview of monkeypox virus and its neuroinvasive potential. Ann Neurol. 2022;92(4):527-531.
Crossref - NDTV. Monkeypox symptoms, prevention as india records 4 cases. 2022. https://www.ndtv.com/india-news/ monkeypox-outbreak-check-symptoms-prevention-as-india-re-cords-4-cases-3190470. Accessed July 27, 2022.
- Okyay RA, Bayrak E, Kaya E, et al. Another epidemic in the shadow of Covid 19 pandemic: a review of monkeypox. EJMO. 2022;6(2):95-99.
Crossref - Di Giulio DB, Eckburg PB. Human monkeypox: an emerging zoonosis. Lancet Infect Dis. 2004;4(1):15-15.
Crossref - Ministry of Health and Family Welfare, Govt. of India. Guide¬lines for management of monkeypox disease. https:// main.mohfw.gov.in/sites/default/files/Guidelines%20for%20 Management%20of%20Monkeypox%20Disease.pdf. Accessed July 24, 2022.
- Kaler J, Hussain A, Flores G, Kheiri S, Desrosiers D. Monkeypox: a comprehensive review of transmission, pathogenesis, and manifestation. Cureus. 2022;14(7):e26531.
Crossref - Petersen E, Kantele A, Koopmans M, et al. Human monkeypox: epidemiologic and clinical characteristics, diagnosis, and prevention. Infect Dis Clin North Am. 2019;33(4):1027-1043.
Crossref - Stanford MM, McFadden G, Karupiah G, Chaudhri G: Immunopathogenesis of poxvirus infections: forecasting the impending storm. Immunol Cell Biol. 2007;85(2):93-102.
Crossref - Learned LA, Reynolds MG, Wassa DW, et al. Extended interhuman transmission of monkeypox in a hospital community in the Republic of the Congo, 2003. Am J Trop MedHyg. 2005;73(2):428-34.
Crossref - Chen N, Li G, Liszewski MK, et al. Virulence differences between monkeypox virus isolates from West Africa and the Congo basin. Virology. 2005;340(1):46-63.
Crossref - Kugelman JR, Johnston SC, Mulembakani PM, et al. Genomic variability of monkeypox virus among humans, Democratic Republic of the Congo. Emerg Infect Dis. 2014;20(2):232-239.
Crossref - Minhaj FS, Ogale YP, Whitehill F, et al. Monkeypox Outbreak -Nine States, May 2022. MMWR Morb Mortal Wkly Rep. 2022;71(23):764-769.
Crossref - Ministry of Health and Family Welfare, Govt. of India. Guide¬lines for management of monkeypox disease. Available at: https:// main.mohfw.gov.in/sites/default/files/Guidelines%20for%20Management
%20of%20Monkeypox%20Disease.pdf. Accessed on 24 July 2022 - Isidro J, Borges V, Pinto M, et al. Phylogenomic characterization and signs of microevolution in the 2022 multi-country outbreak of monkeypox virus. Nat Med. 2022.
Crossref - Brown K, Leggat PA. Human monkeypox: current state of knowledge and implications for the future. Trop Med Infect Dis. 2016;1(1):8.
Crossref - Nalca A, Zumbrun EE. ACAM2000: The new smallpox vaccine for United States Strategic National Stockpile. Drug Des Dev Ther. 2010;4:71-79.
- Guarner J, Johnson BJ, Paddock CD, et al. Veterinary Monkeypox Virus Working Group. Monkeypox transmission and pathogenesis in prairie dogs. Emerg Infect Dis. 2004;10(3):426.
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.