ISSN: 0973-7510
E-ISSN: 2581-690X
Corona disease outbreak occurred in 2019 from Wuhan, China and the virus was identified to be a member of the Coronaviridae family. The disease was named as COVID-19 by WHO. It started as an epidemic and later turned into pandemic affecting world wide. The present study was aimed to conduct a systematic review on most prevalent symptoms associated with COVID-19 and to perform a Meta analysis on Comorbidities associated with COVID-19 and assess its severity in underlying conditions. A literature search was conducted using search engines like Pubmed, Web of Science, Elsevier COVID-19 and LitCovid databases between January 2020 and August 2020. Forest plot analysis was done using Random effects model to estimate odds ratio and 95% confidence interval estimate. 83 papers with a sample size of 19,454 were analysed statistically after adopting inclusion and exclusion criteria. Our results showed the most prevalent symptoms to be Cough, fever, dyspnoea and myalgia in interval plot analysis. When assessed for comorbidities, Hypertension (27.02%), Diabetes (16.61%), Cardiovascular disease (12.75%) and Chronic pulmonary obstructive diseases(19.9%) are found to be the most risk factors in comparison with others. However, a finer experimental research needs to be confirmed with the findings.
COVID-19, Systematic Review, Meta Analysis, Comorbidities, Symptoms
Novel Coronavirus began spreading in Wuhan China by December, 2019 and turned into Pandemic affecting the whole world. World Health Organization (WHO) declared this virus as COVID-19 on 11th February, 2020. International Committee on Taxonomy of Viruses (ICTV) named this virus as Severe Acute Respiratory Syndrome (SARS-CoV2). It is a single stranded positive sense RNA virus belonging to the family Coronaviridae which unlike its close relatives such as SARS-CoV and MERS, has increased affinity towards the ACE 1 receptor, probably a reason in accounting for its increased pathogenicity.1
The virus has a non segmented, large genome size of about 30kb with club shaped spike proteins on the spherical surface. Although the ACE2 receptor has been associated with SARS-CoV2 and HCoV-NL633 a notable change is observed in the expression of ACE2 receptors in the oral tissue, epithelial cells, and the isolation of SARS-CoV-2 from faecal samples and stools of the virus infected samples. This indicates that the oral and faecal route might be a potential route of transmission of the SARS-CoV-2 virus.
The genomic homology studies of SARS-CoV-2 suggested two different possible intermediate hosts, the horseshoe bat2, and the Malayan Pangolins.4 Another study also suggested snakes as a possible intermediate host. The optimization of the SARS-CoV-2 virus to bind to the human receptors efficiently has been attributed to natural selection, but whether this selection occurred before or after the zoonotic transfer, is yet to be studied. However, sequencing studies of the common ancestor of the different strains of the novel Coronavirus estimated to have been present between October and November of 2019 might reveal the significant mutations that the virus underwent which might have contributed to its pathogenicity.5,6
WHO declared the spread of the virus to be through respiratory droplets which resulted in a pandemic outbreak. Previous reports stated that symptoms were noted more in adults with characteristic symptoms of fever, sore throat, cough and malaise. The symptoms ranged from mild to severe like shortness of breath and hospitalization in ICU. As the disease is progressing many other symptoms have been observed which included , loss of smell and taste, diarrhea, vomiting, chest pain etc and is observed in neonates and children as well. Rapid spread of the disease, Morbidity and mortality associated with COVID-19 are very important to determine the possible factors associated with it. Comorbidities like Hypertension, Diabetes, cardiovascular disease, COPD associated with COVID-19 are known to aggravate the condition and increase the risk of infection in patients. Understanding the dynamic changes observed in terms of symptoms and comorbidities in people affected with COVID-19 the present study was undertaken to perform a systematic review and meta analysis on symptoms and comorbidities in COVID-19 infected people.
Eligibility Criteria
The search for research papers was done using search engines like Pubmed, Web of Science, Elsevier COVID-19 and LitCovid databases between January 2020 and August 2020. Key terms used for search included “COVID-19, Coronavirus Disease 2019, clinical characteristics of COVID-19, comorbidities associated with COVID-19 ” etc. The papers were shortlisted based on the title of the paper and abstract. Selection of relevant articles and extraction of data was done selectively by two authors independently who are a part of this study. Disagreements between the authors was resolved in consultation with the third author and by mutual consensus.
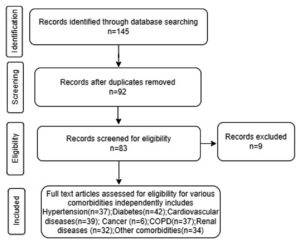
Inclusion and Exclusion criteria were adopted to all the shortlisted papers. Inclusion criteria included the data retrieved from only the papers published in a peer-reviewed journal, Variables extracted from the studies includes the patients of all age groups, gender, clinical manifestations like cough, fever, Myalgia, dyspnoea, sore throat, rhinorrhoea, anorexia, fatigue, headache, diarrhoea, Nausea, chest pain and comorbidities like Hypertension, diabetes, cardiovascular disease, renal disease, Obesity, COPD, Immunodeficiency and cancer, severity of symptoms like patients in ICU, discharged/recovered and mortality were included in study. Exclusion criteria included duplicate studies, general articles, editorial boards, reports published by various health agencies, studies with small sample size and studies with incomplete data were excluded from the study. The steps involved in literature search were showed in Figure 1.
Data Analysis
Interval plot analysis was done for symptoms to show the confidence interval for the mean of the data. Correlation analysis was performed with individual symptoms against mortality to understand the most associated symptom with COVID-19 fatal rate. Relationship between severities of the symptoms was recorded with admission of patients in ICU, discharged/recovered to Mortality rate was done by using surface plot analysis. 3D scatter plots were used to understand the relationship between gender against mortality. All calculations were performed using R programming.
Risk of bias was assessed by a cross-sectional study which provided a snapshot of a COVID and other variables in a defined population at a specific point in time. This is done to infer the relationships between a COVID and other variables.
Statistical analysis was done using R studio software for generating Forest plot analysis. This was done using Random effects model due to heterogeneity between the studies to estimate the random effects and precision which gives 95% confidence interval estimate (CI). The risk of comorbidities in different patients was described using odds ratio and the statistical heterogeneity was assessed using I2 Statistics.
Systematic Review on Symptoms Associated with COVID-19 and Severity of Disease
Database search was conducted using different search engines and 145 research records were found. After cleaning the data for duplication 92 research papers were shortlisted. 83 papers with a sample size of 19,454 were analysed after excluding 9 papers which has insufficient data for analysis adopting exclusion criteria. The data was analysed for symptoms associated with COVID-19 and severity of disease using interval plot analysis. Mortality with respect to gender was done using scatter plot analysis.
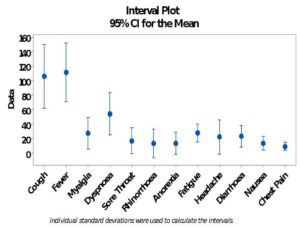
From figure 2 an overlap of confidence intervals was noted commonly for different sets of data. Cough, fever showed higher overlapping which indicates that the two symptoms are most commonly found among the COVID-19 patients as indicated by similarity of data. However, there is slight overlapping noted with dyspnea or shortness of breath characterizing the most prevalent symptom noted along with fever and cough. An interesting observation was made with the other symptoms like Myalgia, sore throat, rhinorrhea, anorexia, fatigue, headache, diarrhea, nausea/vomiting which displayed the commonality and overlapping in interval plot analysis (Figure 2) A clear demarcation can be done and the results can be categorized in two groups: the most prevalent group with cough and fever and less prevalent group with all other symptoms noted. However, one common symptom i.e. dyspnoea or shortness of breath is found to be commonly associated with both the groups. The amount of variation is also significantly high in both cough and fever followed by shortness of breath compared to other symptoms. The symptom chest pain seemed to be very consistent as variation is remarkably less
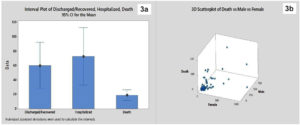
When analysed for severity of symptoms in terms of Discharged /recovered, hospitalized and death, overlapping of data is noted for two categories ie people who are hospitalized and recovered from the disease. Variation is noted maximum for hospitalized patients compared with the other two categories. Death/Mortality did not show any overlapping with the other two groups indicating the least contribution rate in COVID-19 patients as is evidenced by the practical display but the important point to be noted is the small interval in case of death which shows consistency in COVID-19 pandemic mortality (Figure 3a) To understand and investigate the relationship between male, female and mortality rate a 3D scatterplot was drawn. The results from figure 3b demonstrate that COVID-19 mortality is more noted in males than in females which are in accordance with studies done by Del et al.7 This may be due to the variations in hormones like progesterone and 17 β estradiol which acts as immune modulators in viral infections.
Figure 3. 3a represents Interval plot of severity of symptoms; 3b represents 3D scatter plot of gender vs mortality
Meta Analysis on Comorbidities Associated with COVID-19
When analyzed for percentage of prevalence among all comorbidities associated with COVID-19, highest prevalence was noted for Hypertension(27.02%), followed by COPD (19.9%), Diabetes mellitus(16.61%), Other comorbidities like immune deficiency disorders and obesity disorder accounting to 13.66%, cardiovascular diseases (12.75%), Renal disease (6.06%), and cancer (1.5%). Meta analysis was carried out using forest plot analysis after applying inclusion and exclusion criteria independently for shortlisted comorbidities. The total number of studies are not uniform in each case and they vary with complete availability of data pertaining to that comorbidity studied. A total of 37 studies for Hypertension, 42 for diabetes, 39 for cardiovascular, 6 for cancer, 37 for COPD, 32 for Renal diseases and 34 for other abnormalities which included Immunodeficiency and Obesity were analyzed for Meta analysis.
Hypertension
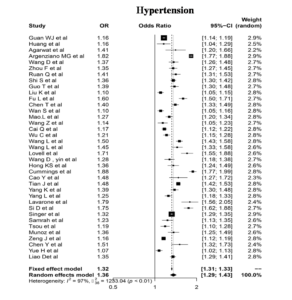
For assessing the impact of the most reported comorbidity Hypertension on COVID-19 mortality a total of 37 studies were tested for Meta analysis after applying exclusion & Inclusion criteria in reported studies. A heterogeneity test was performed for these 37 studies applying random effects model. Forest plot analysis was done with 95% CI which revealed a substantial probability of attaining COVID-19. Heterogeneity, I2 for the studies performed was noted to be 97 % with Odds Ratio of 1.32 (Figure 4). The results indicate that a strong positive correlation was noted with hypertension. Studies by Zhang et al.8 reported cytokine release syndrome and shooting up of IL6 levels in COVID-19 patients which is correlated with earlier studies indicating the role of Interleukins, inflammasomes, cytokines and TLRs in hypertension.9,10 These studies are showing a probability of aggravated responses of COVID-19 in patients with Hypertension as comorbidity. However further research needs to be done at molecular level to confirm the findings.
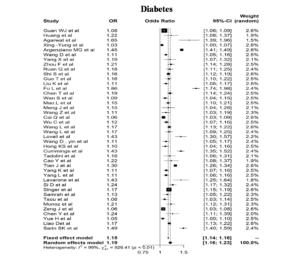
Diabetes
When analysed for impact of Diabetes in patients affected with COVID-19, an odds ratio of 1.19 was noted in 42 studies using random effects model which showed a positive correlation between Diabetes and COVID-19. Heterogeneity was noted as 96% (Figure 5). The findings in previous metaanalysis studies reported by Kou et al11, Fadini, et al12 were quite different from our present findings. One reason for this could be inclusion of many studies in present research. Also, the total estimated Odds ratio value indicates that people with Comorbidity Diabetes exhibits more risk and proceeds to severe COVID-19 disease than normal people. Though some studies could explain the probable correlation between Diabetes and COVID-19 is due to down regulation of ACE2 receptor Gupta R et al.13 the exact mechanism is still unknown. Reports by Kumar and Arora, also suggest that imbalance in different immune cells during diabetes and the shared role of DPP4 receptors and ACE2 receptors in glucose metabolism might be taking the lead role in contributing to the severity of disease in diabetes patients.
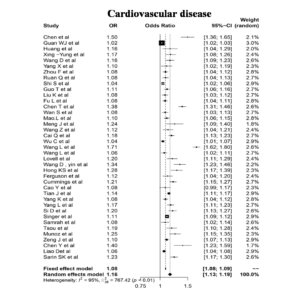
Cardiovascular Disease
Significant heterogeneity was noted in 39 studies pertaining to comorbidity cardiovascular disease with an I2 value of 95%. With forest plot analysis using Random effects model the value was found to be 1.16 which indicates a positive correlation between CVD and COVID-19 which is significant with OR value (Figure 6). The values reported are in accordance with other metaanalysis studies reported so far. However significant correlation can be drawn from our study as the number of studies included are quite high.
The probable mechanism explains the role of ACE2 report in progression of COVID-19 among people with comorbidity CVD. The ACE 2 receptors are expressed in various cells of the body including the cells of the cardiac system.14 An important function of ACE 2 receptors is the conversion of vasoconstrictive angiotensin II to vasodilatory forms, which leads to a negative response on the Renin-angiotensin-aldosterone system (RAAS). Thus the ACE 2 receptors apart from acting as a critical entry site to the SARS CoV 2 virus, also play a role in controlling the RAAS mechanism, which is in turn again responsible for several cardiovascular diseases including hypertension, atherosclerosis and even heart failure.15 ACE 2 commonly has an antihypertensive effect and also affects the cardiac output. Therefore, the dysregulation of this receptor during SARS-CoV-2 infection might be a plausible explanation for the incidence of cardiac abnormalities during COVID-19.16 The overdrive of the immune system has also been cited as a cause of heart damage in COVID-19 patients.17
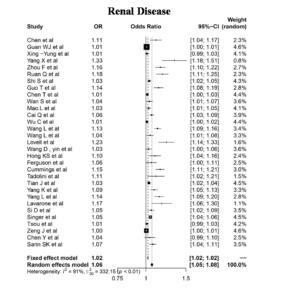
Renal Diseases
The pooled odds ratio estimate the number of patients affected by both renal diseases and COVID-19 among 31 studies was found to be 1.06. The randomized effects model also demonstrated a pronounced heterogeneity of I2 = 91% and P<0.01 (Figure 7). Overall a positive correlation between renal diseases and SARS-CoV-2 infection can be inferred from this extensive meta-analysis study, making it an important comorbidity associated with COVID-19 disease severity. The most commonly recorded renal diseases were Chronic Kidney disease(CKD) and acute kidney injury (AKI).
In our meta analysis a very small proportion of cases reported end stage renal disease, kidney injury, chronic renal failure and chronic renal insufficiency. However, the reporting of these was very rare in other studies. Therefore these values differed from the combined value obtained in our analysis when compared with studies.18,19,20
The underlying mechanism of renal diseases has been explored by many studies, which have stated several routes through which this might occur. The viral particles were observed at different sites in the kidney, including the viral antigens in kidney tubules,21 virus-like particles in the proximal tubular epithelium and podocytes,22 and viral RNA in urine samples of a COVID-19 infected patient with CKD.23 The expression of ACE2 receptor24,25,26 and its coexpression with protease coding TMPRSS genes27 in kidneys similar to lungs and the digestive system points to the fact that the kidney is a potential target for the virus. The dysregulation of immune factors such as induction of CD68+ cells and its complement C5b9 in tubular epithelial cells,28 reduction of T Cells, and increase of certain interleukins directly cause cytokine storms and significant inflammatory responses and in turn contribute to kidney damage. The cytokine storms can have various serious consequences. One study pointed out that the activation of coagulation factors mediated by cytokine storm can lead to hypercoagulation thereby leading to necrosis.29 Cytokines can also cause pressure on the kidney leading to rhabdomyolysis.30 A lung and kidney cross interaction could also impair the functions of the kidney leading to internal damage, and disruption of circulation in kidneys.
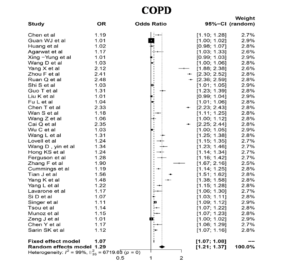
COPD
COPD carrying an odds ratio of 1.07 & heterogeneity of 99% has confirmed a greater positive correlation with COVID-19 ( CI -95% & p=0) on forest plot analysis (Figure 8) COPD which was ranked as the third leading cause of death by the WHO in low income countries, might be a potential cause of maximum infection in those areas. COPD was considered to have the highest mortality rate & risk factors especially with smokers in comparison to other comorbidities in COVID-19 infection.31
Similar to SARS-CoV, COVID-19 virus also possesses spike protein which is primed to the cellular serine protease TMPRSS2, this facilitates fusion & cell entry though ACE2. COPD causes increased ACE2 expression.32 However ACE2 expression is decreased in individuals having asthma and are taking Inhaled & systemic corticosteroids(ICS) in comparison to those not taking ICS33 giving a possibility to decrease the viral entry. Anti ACE2 acts as a functional receptor in blocking the viral replication.34
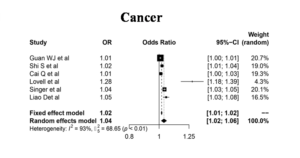
Cancer
Not many papers resulted on correlating cancer and COVID-19. However the six studies shortlisted showed an OR of 1.04 and heterogeneity of 93%, which demonstrates the comorbidity Cancer has shown a positive correlation (p<0.01) with COVID-19 on Forest plot analysis considering CI of 95% (Figure 9).
Individuals with cancer as comorbidity were considered to be vulnerable towards COVID-19. Though the studies report the possibility with the mediation of increased ACE2 levels35 in the plasma samples, which is the key connector between cancer & COVID-19 host interactions, the disproportionate results in various other studies leave keyholes to be filled in. Effect of ACE2 expression & its impact on COVID-19 depends upon multiple factors like the type of cancer, age, sex etc.36 However the cytokine storm effects37,38 will keep individuals with cancer comorbidity at higher risk.
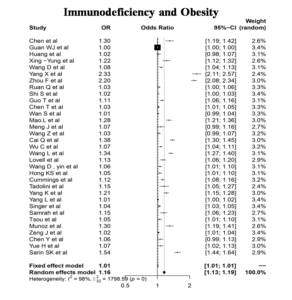
Other Comorbidities (Immune Deficiency and Obesity)
The total estimated fraction of SARS-CoV-2-infected patients suffering from immune deficiency and Obesity in a randomized effects model was found to be 1.16 [95%=1.13-1.19]. A remarkable heterogeneity of I2 = 98% and P=0 was noted (Figure 8). This strong correlation between these two factors with the COVID-19 infection has significant room to be explored (Figure 10).
Results reported by Gao et al.39, Huang et al. 40 are in accordance with the results obtained by the present study. The mechanism underlying the positive correlation between obesity and COVID-19 is yet to be studied, but notably studies by reported that obese patients are likely to develop hypoventilation leading to lung complications in severe SARS-CoV-2 infected patients. It was also noted that since ACE2 expression was higher in adipose tissue, obese individuals are at a higher risk to contract SARS-CoV-2 virus particles entry.41 Since obesity is also a risk factor for other comorbidities like diabetes and also affects the immune responses, it is safe to say from our meta-analysis that obese individuals are at a higher risk to develop severe COVID-19 infections.
Limitations
Patients can be suffering with multiple comorbodities which might have added to the severity in effect. This is a very important limitation of the study. The studies with reported mortality rates to a specific comorbidity alone were used for analysis, an inherent bias could exist in terms of selection of patients and their treatment regimes also may differ.
SARS-Cov-2 affected large group of population especially the patients with comorbidities. The present study analysed for most prevalent and less prevalent symptoms and comorbidities associated with COVID-19. The study highlights the most common symptoms to be fever, cough and shortness of breath and the most correlated comorbidities are Hypertension, Diabetes, CVD and COPD. However, in depth research studies are to be done as the studies are still in infancy with novel Coronavirus COVID-19 and the underlying mechanisms for its varied expression with respect to Symptoms and comorbidities in diverse groups of population is yet to be studied.
ACKNOWLEDGMENTS
The authors Swathi J, Selva Kumar V and Aparna Y thank Principal and Management of Bhavan’s Vivekananda college of Science, Humanities and Commerce for their constant support and encouragement. The authors also thank the support provided by STAR College scheme, Department of Biotechnology, Government of India (BT/HRD/11/034/2019). The author Prathyusha Y thank Principal and Management of St Marys College, Yousufguda for extending their support.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
YA designed and guided the research project. SJ and PY contributed equally in retrieving and consolidation of data. VSK performed the statistical analysis of the data. All authors contributed equally in the preparation of manuscript and approved the same for final publication.
FUNDING
The research project undertaken was supported by the Star College Scheme, Department of Biotechnology, Government of India (BT/HRD/11/034/2019) at Bhavan’s Vivekananda College.
DATA AVAILABILITY
All datasets analyzed during this study are included in the manuscript. The data sheet used for analysis is available with the corresponding author.
ETHICS STATEMENT
Not applicable.
- Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. The Lancet, 2020; 395(10223), 507-513.
Crossref - Zhou P, Yang XL, Wang XG, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. nature, 2020;579(7798):270-273.
Crossref - Fehr AR, Perlman S. Corona viruses: an overview of their replication and pathogenesis. In Coronaviruses, 2015 (pp. 1-23). Humana Press, New York, NY.
Crossref - Lam TTY, Jia N, Zhang YW, et al. Identifying SARS-CoV-2-related coronaviruses in Malayan pangolins. Nature, 2020;1-4.
- Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD. How will country-based mitigation measures influence the course of the COVID-19 epidemic?. The Lancet, 2020;395(10228):931-934.
Crossref - Yang X, Yu Y, Xu J, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. The Lancet Respiratory Medicine. 2020.
Crossref - Del RC, Malani PN. 2019 novel coronavirus-important information for clinicians. Jama, 2020;323(11), 1039-1040.
Crossref - Zhang C, Wu Z, Li JW, Zhao H, Wang GQ. The cytokine release syndrome (CRS) of severe COVID-19 and Interleukin-6 receptor (IL-6R) antagonist Tocilizumab may be the key to reduce the mortality. International journal of antimicrobial agents, 2020;105954.
Crossref - Tanase DM, Gosav EM, Radu S, et al. Arterial hypertension and interleukins: potential therapeutic target or future diagnostic marker? International journal of hypertension, 2019.
Crossref - Youn JC, Yu HT, Lim BJ, Immunosenescent CD8+ T cells and CXC chemokine receptor type 3 chemokines are increased in human hypertension. Hypertension, 2013; 62(1):126-133.
Crossref - Kou M, Hu X , Chen M. Appel, The relationship of COVID-19 severity with cardiovascular disease and its traditional risk factors: A systematic review and meta-analysis. BMJ medRxiv Prepr. 2020.
- Fadini GP, Morieri ML, Longato E, Avogaro A. Prevalence and impact of diabetes among people infected with SARS-CoV-2. Journal of Endocrinological Investigation, 2020;1
Crossref - Gupta R, Hussain A, Misra A. Diabetes and COVID-19: evidence, current status and unanswered research questions. European journal of clinical nutrition, 2020; 1-7.
Crossref - Grob S, Jahn C, Cushman S, Bär C, Thum T. SARS-CoV-2 receptor ACE2-dependent implications on the cardiovascular system: From basic science to clinical implications. Journal of Molecular and Cellular Cardiology, 2020.
- Iravanian S, Dudley JrSC. The renin-angiotensin-aldosterone system (RAAS) and cardiac arrhythmias. Heart rhythm, 2008; 5(6):S12-S17.
Crossref - Ghafouri-Fard S, Noroozi R, Omrani MD. Angiotensin converting enzyme: A review on expression profile and its association with human disorders with special focus on SARS-CoV-2 infection. Vascular Pharmacology, 2020;106680.
Crossref - Rio DC, Malani PN. COVID-19—new insights on a rapidly changing epidemic. Jama, 2020;323(14): 1339-1340.
Crossref - Oliveira CB, Lima CAD, Vajgel G, Coelho AVC, Sandrin-Garcia P. High burden of acute kidney injury in COVID-19 pandemic: systematic review and meta-analysis. Journal of Clinical Pathology,2020.
Crossref - Xu Z, Tang Y, Huang Q. Whether Remdesivir Increases the Risk of Acute Kidney Injury (AKI) in Patients with COVID-19: A Systematic Review and Meta-Analysis, 2020.
Crossref - Kunutsor SK, Laukkanen JA. Renal complications in COVID-19: a systematic review and meta-analysis. Annals of Medicine, 2020; 1-9.
Crossref - Diao B, Feng Z, Wang C. Human kidney is a target for novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. MedRxiv, 2020.
Crossref - Su H, Yang M, Wan C. Renal histopathological analysis of 26 postmortem findings of patients with COVID-19 in China. Kidney international, 2020.
Crossref - Wang L, Li X, Chen H, et al. Coronavirus disease 19 infection does not result in acute kidney injury: an analysis of 116 hospitalized patients from Wuhan, China. American journal of nephrology, 2020;51(5): 343-348.
Crossref - Qi F, Qian S, Zhang S, Zhang Z. Single cell RNA sequencing of 13 human tissues identify cell types and receptors of human coronaviruses. Biochemical and biophysical research communications, 2020.
Crossref - Serfozo P, Wysocki J, Gulua G, et al. Ang II (angiotensin II) conversion to angiotensin-(1-7) in the circulation is POP (prolyloligopeptidase)-dependent and ACE2 (angiotensin-converting enzyme 2)-independent. Hypertension, 2020;75(1): 173-182.
Crossref - Ye M, Wysocki J, William J, Soler MJ, Cokic I, Batlle D. Glomerular localization and expression of angiotensin-converting enzyme 2 and angiotensin-converting enzyme: implications for albuminuria in diabetes. Journal of the American Society of Nephrology, 2006;17(11):3067-3075.
Crossref - Pan XW, Da-Xu HZ, Zhou W, Wang LH, Cui XG. Identification of a potential mechanism of acute kidney injury during the COVID-19 outbreak: a study based on single-cell transcriptome analysis. Intensive care medicine, 2020;1.
Crossref - Muscogiuri G, Pugliese G, Barrea L, Savastano S, Colao A. Comentary: Obesity: The “Achilles heel” for COVID-19?. Metabolism-Clinical and Experimental, 2020:108.
Crossref - Gagliardi I, Patella G, Michael A, Serra R, Provenzano M, Andreucci M. COVID-19 and the kidney: from epidemiology to clinical practice. Journal of Clinical Medicine, 2020;9(8):2506.
Crossref - Khouchlaa A, Bouyahya A. COVID-19 nephropathy; probable mechanisms of kidney failure. Journal of Nephropathology, 2020;9(4).
Crossref - Alqahtani JS, Oyelade T, Aldhahir AM, et al. Prevalence, severity and mortality associated with COPD and smoking in patients with COVID-19: a rapid systematic review and meta-analysis. PloS one, 2020;15(5):e0233147.
Crossref - Leung JM, Niikura M, Yang CWT, Sin DD. COVID-19 and COPD. European Respiratory Journal, 2020;56(2).
Crossref - Peters MC, Sajuthi S, Deford P, et al, COVID-19 related genes in sputum cells in asthma: relationship to demographic features and corticosteroids. Am J Respir Crit Care Med., 2020; 202(1):83-90.
Crossref - Tanonaka K, Marunouchi T. Angiotensin-converting enzyme, 2016;147(2): 120-121.
Crossref - Wallentin G, Kaziyeva D, Reibersdorfer-Adelsberger, E. COVID-19 intervention scenarios for a long-term disease management. International journal of health policy and management, 2020;9(12):508-516.
Crossref - ElGohary GM, Hashmi S, Styczynski J, et al. The risk and prognosis of COVID-19 infection in cancer patients: a systematic review and meta-analysis. Hematology /oncology and stem cell therapy, 2020.
Crossref - Jyotsana N, King MR. The impact of COVID-19 on cancer risk and treatment. Cellular and Molecular Bioengineering, 2020;1-7.
Crossref - Bakouny Z, Hawley JE, Choueiri TK, et al. COVID-19 and cancer: current challenges and perspectives. Cancer cell, 2020.
Crossref - Gao Y, Chen Y, Liu M, Shi S, Tian J. Impacts of immunosuppression and immunodeficiency on COVID-19: A systematic review and meta-analysis. The Journal of Infection, 2020.
Crossref - Huang Y, Yao LU, Huang YM, Min WANG, Wei LING, Yi SUI, Hai-Lu ZHAO. Obesity in patients with COVID-19: a systematic review and meta-analysis. Metabolism, 2020:154378.
Crossref - Kassir R. Risk of COVID-19 for patients with obesity. Obesity Reviews, 2020;21(6).
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.