ISSN: 0973-7510
E-ISSN: 2581-690X
2019 – Coronavirus diseases caused by severe acute respiratory syndrome coronavirus 2. In Gujarat, COVID-19’s first two cases were confirmed in Rajkot and Surat on 19th March 2020. In India to prevent COVID-19 cases from being: “test, track and treat”: For testing, RT-PCR is the gold standard test or frontline testing for the Coronavirus. The most prominent cause of infection in health care workers due to they were directly exposed to unrecognized COVID-19 patients. To determine the Infection rate and also assess the clinical profile of COVID-19 infections in health care workers. Sample collected from 2081 health care workers by universal sampling method during the period from April 2020 to November 2020. Nasopharyngeal and Oro-pharyngeal swabs were collected at the collection center and tested at the Viral Research Diagnostic Laboratory (VRDL), by RT-PCR (Real-Time Polymerase Chain Reaction) Method. During the study period, there were 2081 suspected healthcare workers samples received from 70 Health care workers were positive. We observed 3.36 % Positivity rate, positivity was high in the age group of 20–30 years 64.2%, most common clinical presentation was a fever 82.8%, cough 47.1% and Sore throat 50% and 01 severely infected health care worker died during hospitalization. Health care workers were at a higher risk of COVID-19 infection. So, to protect health care workers routine screening of asymptomatic staff and early identification of staff with potential infection could help to lower the risk. COVID-19 mortality was lower in health care workers.
HCWs, COVID-19, SARS-CoV-2 virus, RT-PCR, RNA, Mortality
2019 – Coronavirus disease was first identified in China as a newly emerging infectious disease in December 2019. In January 2020, the World Health Organization (WHO) declared COVID-19 a pandemic. COVID-19 was caused by the SARS-CoV-2 virus.1 In Gujarat, the first two cases were confirmed in Rajkot and Surat on 19th March 2020.2 National Institute of virology scientists isolated the strain SARS-CoV-2 virus on 14 march 2020, which will help towards the development of drugs, diagnostic kits, and vaccines.3 In India to prevent COVID-19 cases from being: “test, track and treat”: For testing RT-PCR is the gold standard or frontline test for the Coronavirus but other types of tests available like antibody/antigen detection, Truenat (Chip-based, rapid molecular test) and CBNAAT (Cartridge-based nucleic acid amplification test) were introduced; ICMR advised antigen/antibody detection test are as “supplementary test” to molecular testing.4 The disease burden is expected to rise due to community transmission from asymptomatic individuals. The SARS-CoV-2 virus spreads when person to person in close contact. The virus can spread from an infected person’s respiratory tract (mouth or nose) by larger ‘respiratory droplets’ or smaller ‘aerosols’ during the person sneezes, coughs, heavily breathes, or talks.5 In the first wave of COVID-19 the sporadic cases evolved; so, the chains of transmission were broken by effective contact tracing, defined quarantine zone, Sanitary curfew, and isolation of COVID-19 positive patients at treatment centers.6 In Asia, currently, India has the largest number of confirmed cases, with 26.7 million cases reported for COVID-19 infection and 3rd largest number of COVID-19 deaths.7-9 Health care workers were serving as a vector for transmission of illnesses because of higher exposure to infectious diseases as compared to the general population, and also repeated exposure to the same pathogen may alter the course of infectious diseases.10 Thousands of doctors, Nurses, and health workers have been infected with COVID-19; because in patient-facing roles, they will be front-line healthcare workers.11-12 As Frontline health – care workers they were exposed to large numbers of infected patients for a long period, and inadequate knowledge and training for infection prevention and control, the most prominent causes are directly exposed to unrecognized COVID-19 patients and also some medical procedures that generate aerosols that lead to aerosol transmission during procedures.13 Here we outline the testing of both symptomatic and asymptomatic cases of Healthcare workers. This study shows the prevalence of COVID-19 in Health care workers and their characteristics who tested positive for COVID-19 by RT-PCR method (Using kit Meril diagnostic) at Jamnagar, Gujarat.
Aim and Objective
To determine the Infection rate of COVID-19 among healthcare workers.
To assess the clinical profile of COVID-19 infected health care workers.
Target Population
All frontline health care workers involved in care, screening, diagnosis and Management, sample collection, transportation of sample, testing, and Bio-medical waste handlers of Ahmedabad, Botad, Dang, Dwarka, Gir-Somnath, Jamnagar, Junagadh, Kutch, Morbi, Porbandar, Rajkot, Surendra Nagar districts. Sample size: A total of 2081 samples were collected from health care workers by universal sampling method during the period from April 2020 to November -2020. Type of Study: Cross-sectional study.
Inclusion Criteria
All health care workers exposed directly or indirectly to COVID-19 patient care and willing to participate in the study and gave written consent.
Exclusion Criteria
History of close contact with a family member or close friends outside the working area. The study got approval from the Ethical Institution Committee, M.P. Shah Medical College and Guru Gobind Singh Hospital, Jamnagar, IEC/Certi/93/03/2020.
Sample Collection
Oropharyngeal and Nasopharyngeal swabs were collected at the collection center and tested at the Department of Microbiology at Viral Research Diagnostic Laboratory (VRDL) section, M. P. Shah Medical College at Jamnagar by Real-Time Polymerase Chain Reaction (RT-PCR) Method.
The following steps to get the quantitative detection for SARS CoV-2: 1) Viral RNA Extraction: QIAamp Viral RNA mini kit (Qiagen, Valencia, CA, USA) was used for RNA extraction by following the manufacturer’s protocol. In the microcentrifuge tube add 560 μl prepared Buffer and 140 μl sample. Mix by pulse-vertexing for 15 seconds then Incubate for 10 min at room temperature (15–25°C). To remove drops from the inside of the lid centrifuge the tube. RNA precipitation was done using 560 μl of ethanol (96%–100%) mixed into the sample by pulse-vertexing for 15 seconds. The Final viral RNA was eluted in 60 μl of the elution buffer. 2) Master Mix Preparation: We have used the Meril COVID-19 One-step RT-PCR Kit from Meril Diagnostics Pvt. Ltd for RT-PCR. For that, we have used the manufacturer protocol according to a Total Volume of 15 μl including Resuspended Master Mix – 9 μl, ORF1ab/N/IC Primer and Probe (FAM/HEX/ROX) – 1 μl, and RNase-free water – 5 μl. Aliquot 15 μl of the master mix preparation into the PCR plate including one positive control and one negative control; add 5 μl sample into the appropriate wells. Add 5 μl RNase-free water to the negative control well and 5 μl positive control to the positive control well respectively. After adding, cover with a lid, and by using a mini centrifuge spin down briefly then place the PCR plate into the instrument; save your plate setup. 3.) Program the run method as follows: Amplification Program (Temp./time/cycle) for RT-PCR: Reverse Transcription at 50 °C/15 min/ 1 cycle; cDNA Initial Denaturation at 95 °C/ 3 min/1 cycle; Denaturation 95 °C/15 sec/40 cycle; Annealing, Extension and Fluorescence measurement at 55 °C/ 40 sec/40 cycle and final step was Cooling at 25 °C/10 sec/1 cycle. 4.) Interpretation: specimen is of acceptable quality when in clinical samples RNase P reaction curves cross the threshold line at or before 35 cycles, which indicates the presence of sufficient RNA in the sample. First to analyze the Internal control (positive and negative) of the assay. Detection is valid if Ct ≤ 35, and then analysis of the subsequent assay. Clinical samples show a typical Sigmoidal (S – type) amplification curve in FAM and HEX channels, which indicates the COVID-19 virus is present in the sample (Positive). If no amplification curve in FAM and HEX channels (No Ct) and no typical S – type (Sigmoidal) that indicates COVID-19 virus is Negative. Ct cut-off value for different fluorescent channels is as below for consider positive:
ORF1ab gene (FAM) – Ct ≤ 35
N gene (HEX) – Ct ≤ 35
Internal Control (ROX) – Ct ≤ 35
Data Collection
Data were collected, cleaned, and analyzed using Microsoft Excel for Windows 10. Distribution statistics are used.
During the study period, there were 2081 suspected HCWs samples received from various districts (by universal sampling method) [Figure 1 /Table] in our laboratory at M.P. Shah Govt. Medical College, Jamnagar, out of which 70 Health care workers were positive. We observed 3.36 % Positivity rate in HCWs. Out of 70 HCWs 83% (n= 58) were Symptomatic while 17% (n=12) were Asymptomatic.
Table:
District-wise distribution of samples of Health care workers (n=2081).
District |
Total |
Positive |
|---|---|---|
Ahmedabad |
53(2.55%) |
1 (1.89%) |
Botad |
1(0.04%) |
0 (0%) |
Dang |
1(0.04%) |
0 (0%) |
Dwarka |
273(13.11%) |
0 (0%) |
Gir Somnath |
6(0.28%) |
0 (0%) |
Jamnagar |
854(41.03%) |
64 (7.49%) |
Junagadh |
2(0.09%) |
0(0%) |
Kutch |
7(0.33%) |
1(14.29) |
Morbi |
531(25.51%) |
0(0%) |
Porbandar |
330(15.85%) |
4(1.21%) |
Rajkot |
20(0.96%) |
0(0%) |
Surendra Nagar |
3(0.14%) |
0(0%) |
Total |
2081 |
70(3.36%) |
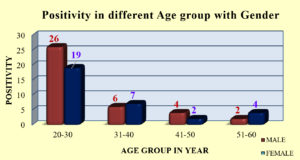
The positivity was high in age group of 20–30 year 64.2% (n=45), followed by 31-40 year 18.5% (n=13), and 41-60 year 8.5% (n=6). Positivity was higher in male 54.3% (n=38) as compare to female 45.7% (n=32) HCWs. (Figure 1).
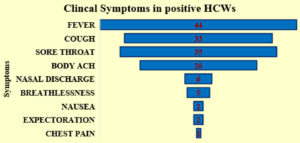
The frequent clinical presentation in HCWs was a fever (82.8%, n=44), cough (47.1%, n=33), Sore throat (50%, n=35), Bodyache (37.1%, n=26), Nasal discharge and Breathlessness were seen only (8.5%, n=6) and (7.1%, n=5). Other symptoms such as Nausea, expectoration, and chest pain were 2-3% which represented small percentages. (Figure 2).
In the current study, the infection among HCWs with comorbidity or chronic disease like Hypertension (n=1. 1.43%) and diabetes (n=4, 5.71%) were not found to be significant. Positivity rate in health workers like doctors shows (n=24, 34.28%) and other paramedical and supportive or administration staff shows (n=46, 65.72%).
One severely infected HCW (1.43%) died during hospitalization. All the HCWs had a mild infection so, do require hospitalization but some HCWs (n=12, 17.14%) were moderate to severe infections were admitted to the hospital.
The present study summarized the clinical information, characteristics, comorbidity, and risk factors of COVID-19 in health care workers.
The Study determines positivity was 3.4% in HCWs, similar to sabetian et al.14 5.6%, Al Maskari Z et al.15 4.3%, Nguyen L H et al.16 3.9%, which explains the lower infection rates in HCWs may be due to the proper use of personal protective equipment’s, like N95 masks, gloves and face shield in flu OPD and COVID-19 wards,17 but in opposite higher in Gholami, Mandana et al.18 51. 7% indicate inappropriate workplace setting, long-term exposure, and insufficient use of Personal protective equipment; while one study by Lai, Xiaoquan et al.19 1.1% which shows much lower positivity signify the diligent prevention action taken in hospitals to prevent transmission in a health care setting.
In a study out of 70, Positive HCWs 83% (n=58) were Symptomatic and 17% (n=12) were asymptomatic compared with Tolpadi A et al.20 shows respectively 88% and 12% and Xiaoquan et al.19 shows a total of 0.9% of positive HCWs were asymptomatic. Overall, the percentage might become very less but high risks for close contact with persons and the community. So, to avoid cross-infection early recognition of asymptomatic carriers would be important and should be set apart from co-workers and family.
Positivity was higher in males 38 (54.3%) as compared to females 32 (45.7%), which may be due to the majority of the male working outside than females; which was similar to Chu J et al.21 63.2% and 36.8%, Huang, Chaolin et al.22 73% and 27% respectively, in contrast to that Tolpadi A et al.20 shows higher in female 55.1%, than male 44.8%, also higher in the USA (73%). This may be due to a large number of female nursing staff working in the hospital area.17
In this study more affected age group was 21-30 years 64.2%, followed by 31-40 years 18.5%, similarly was seen in Al Maskari Z et al.15 41.5% and Nguyen L H et al.16 28.1%, which was conflicting to reported by Huang et al.22 and Wang et al.23 Based on empirical assumptions some contraindications like the lower ratio of elder people in medical staff; and medial age staff (aged 20-40years) are the mainstays of the hospital due to longer work time and higher work intensity but this was not supported by quantitative analysis.
The most common clinical presentation was in the present study fever 82.8%, cough 47.1%, and Sore throat 50%; similar to Al Maskari Z et al.15 Nguyen LH et al.,16 and Gholami, Mandana et al.18 Study shows HCWs had mild or moderate symptoms; for these various possible reasons young adults HCWs were more affected; and early symptoms were easily noticed by HCWs, which could explain the reason for higher reporting of fever as a clinical presentation in our study. So, for a better outcome, early diagnosis and treatment were preferred.
However, death among HCWs is rare, and mostly older HCWs were more affected, and also universal availability and utilization of PPE reduce the infection in HCWs. Various recent study discovers that HCWs those without PPE were more infected than who had used PPE.17
Limitation
Our study was retrospective and we included only molecular (SARS-CoV2 PCR) tested patients because RT-PCR was high specificity; we were not included patients tested with other types of testing methods like rapid antigen/ antibody detection, CBNAAT, etc. In addition, we study for 8 months; so difficult to access host risk factors, disease severity, and mortality for SARS -Cov-2 infection. And also, does not discriminate against numerous types of HCWs according to their Occupation, Experience level, and amount of exposure to the infected patient or aerosolizing systems.
This finding shows HCWs were at a higher risk of COVID-19 infection during providing care to suspected or confirmed cases. HCWs patients had lower hospitalization due to younger age group and early detection of mild symptoms; that concludes regular screening of asymptomatic staff and quick identification of staff with probable infection help to defend HCWs. COVID-19 mortality was lower in health care workers due to early detection of symptoms, early treatment, and use of effective preventive measures; it highlights the regular training of HCWs regarding infection control practices related to COVID-19 and their strict implementation should be an essential component of a preventive strategy.
ACKNOWLEDGMENTS
The authors would like to thank all the Staff Members of Viral Research Diagnostic Laboratory (VRDL), Microbiology Department, Shree M.P. Shah Government Medical College for their help and support.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
All authors have made substantial, direct and intellectual contribution to the work, and approved it for publication.
FUNDING
None.
DATA AVAILABILITY
All datasets generated or analyzed during this study are included in the manuscript.
ETHICS STATEMENT
This study was approved by the Institutional Ethics Committee, Shree M.P. Shah Government Medical College, Guru Gobindsingh Hospital, Jamnagar with reference number IEC/Certi/93/03/2020.
- World Health Organization. Coronavirus disease (COVID-19) outbreak: rights, roles and responsibilities of health workers, including key considerations for occupational safety and health: interim guidance. World Health Organization. 2020. https://apps.who.int/iris/handle/10665/331510
- “Coronavirus | Gujarat reports first cases of COVID-19 infection”. The Hindu. 2020. https://www.thehindu.com/news/national/other-states/coronavirus-gujarat reports-first-cases-of-covid-19-infection/article31111847.ece
- Jha, Durgesh Nandan. Coronavirus cases in India: Fewer cases, but India becomes 5th country to isolate coronavirus. The Times of India. 2020. https://www.thehindu.com/news/national/coronavirus-live-updates-march-14-2020/article62125461.ece
- Abhishek De, Covid-19 testing: What are the testes and testing procedures being carried out in India? 2020. https://indianexpress.com/article/explained/coronavirus-covid-19-testing-procedures-in-india-6479312
- Ha noi, Q&A: How is COVID-19 transmitted? 2020. https://www.who.int/vietnam/news/detail/14-07-2020-q-a-how-is-covid-19-transmitted.
- Comparative analysis of public health measures implemented related to COVID-19 across the first wave (2020) and second wave (2021). World Health Organization. 2021. https://www.afro.who.int/publications/comparative-analysis-public-health-measures-implemented-related-covid-19-across-first.
- Tiwari A. From Janta Curfew To Unlock 2.0: How India Fought COVID-19 And Crossed 1 Million Cases. 2020. https://www.indiatimes.com/trending/social-relevance/indias-covid-fight-518207.html
- Bhattacharya A. India’s Covid toll tops 3 lakh, 50,000 deaths in 12 days. The Times of India. 2021. https://timesofindia.indiatimes.com/india/indias-covid-toll-tops-3-lakh-50000-deaths-in-12-days/articleshow/82892432.cm
- “India’s COVID crisis ‘beyond heart breaking’: WHO. 2021. https://www.aljazeera.com/news/2021/4/26/india-sets-new-covid-world-record-for-5th-straight-day-live-news
- Mohanty A, Kabi A, Mohanty AP. Health problems in healthcare workers: A review. J Family Med Prim Care. 2019;8(8):2568-2572.
Crossref - Mascarenh A. “747 doctors died of Covid-19 in India: IMA”. The Indian Express. 2021. https://indianexpress.com/article/cities/pune/747-doctors-died-of-covid-19-in-india-ima-7277087
- Dey S. 87k health staff infected with Covid, 573 dead; 74% cases from six states. The Times of India. 2020. https://timesofindia.indiatimes.com/india/over-87k-health-workers-infected-with-covid-19-573-dead/articleshow/77814189.cms
- Wang J, Zhou M, Liu F. Reasons for healthcare workers becoming infected with novel coronavirus disease 2019 (COVID-19) in China. J Hosp Infect. 2020;105(1):100-101.
Crossref - Sabetian G, Moghadami M, Haghighi LHF, et al. COVID-19 infection among healthcare workers: a cross-sectional study in southwest Iran. Virol J. 2021;18(1):58.
Crossref - Al Maskari Z, Al Blushi A, Khamis F, et al. Characteristics of healthcare workers infected with COVID-19: A cross-sectional observational study. Int J Infect Dis. 2020;102:32-36.
Crossref - Nguyen LH, Drew DA, Joshi AD, et al. Risk of COVID-19 among frontline healthcare workers and the general community: a prospective cohort study. Preprint. medRxiv. 2020;2020.04.29.20084111.
Crossref - Kim R, Nachman S, Fernandes R, et al. Comparison of COVID-19 infections among healthcare workers and non-healthcare workers. PLoS One. 2020;15(12):e0241956.
Crossref - Gholami M, Fawad I, Shadan S, et al. COVID-19 and healthcare workers: A systematic review and meta-analysis. Int J Infect Dis. 2021;104:335-346.
Crossref - Lai X, Wang M, Qin C, et al. Coronavirus Disease 2019 (COVID-2019) Infection Among Health Care Workers and Implications for Prevention Measures in a Tertiary Hospital in Wuhan, China. JAMA Netw Open. 2020;3(5):e209666.
Crossref - Tolpadi A, Mane A, Oswal J, et al. Clinico-epidemiological profile of COVID-19 among health care workers from a tertiary care hospital. Int J Adv Med. 2021;8(8):1047-1051.
Crossref - Chu J, Yang N, Wei Y, et al. Clinical characteristics of 54 medical staff with COVID-19: A retrospective study in a single center in Wuhan, China. J Med Virol. 2020;92(7):807-813.
Crossref - Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China Lancet. 2020;395(10223):497-506.
Crossref - Wang X, Liu W, Zhao J, et al. Clinical characteristics of 80 hospitalized frontline medical workers infected with COVID-19 in Wuhan, China. J Hosp Infect. 2020;105(3):399-403.
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.