ISSN: 0973-7510
E-ISSN: 2581-690X
This study examined 150 ear swab samples from patients with otitis media who consulted at Al-Sadr Teaching Hospital from January to April 2021 in Misan, Iraq. The participants were aged 14–50 years, among which the infection rate was highest in participants aged 14–22 years and lowest in those aged 40–50 years. Subsequently, bacterial isolates were identified based on their morphology in various culture media and using biochemical tests. Six bacterial species were identified, namely Pseudomonas aeruginosa, Staphylococcus aureus, Escherichia coli, Streptococcus pneumoniae, Klebsiella pneumoniae, and Staphylococcus epidermidis. Staphylococcus aureus had the highest infection rate (30%), whereas Staphylococcus epidermidis had the lowest infection rate (8.55%). When the sensitivity of each isolate to antibiotics was determined, Escherichia coli was the most sensitive to trimethoprim (TMP), whereas Pseudomonas aeruginosa was the most resistant to 75% of the tested antibiotics.
Otitis Media, Pathogenic bacteria, Antibiotic resistance
Ear infection (otitis media) is a major public health issue in developing countries, with considerable infection rates and financial costs to patients, communities, and healthcare facilities. Even though it can affect adults, it is a commonly encountered ailment in children, resulting in numerous postoperative appointments in both modern and developing economies.1 The middle ear effusion (MEE), without symptoms or signs of severe disease, is recognized in approximately 10% of children as a result of acute otitis media. Chronic OME or the absence of purulent fluid in the middle ear, in the absence of constitutional symptoms, can result to significant hearing loss and difficulties in speech, language, and social skills.2-4,17,30 Otitis media encompasses a spectrum of conditions, including minor acute otitis media, otitis media with effusion, acute otitis media, and chronic otitis media (COM).5 Improper treatment of OM, including imprecise diagnostic tests or misuse of antibiotics, results in inflamed otitis, frequent incisions; subsequent complications, such as RAOM and persistent middle ear effusion requiring the incorporation of a drainage tube, which frequently results in hearing loss, brain abscess, COM, and/or sepsis.5-7 In addition, otitis externa is an inflammation of the external auditory canal, which is more prevalent in patients with eczema or diabetes mellitus.
The identification of OM is hampered by a lack of a link between clinical symptoms and the causative microorganism, as well as the pattern of medication susceptibility. Furthermore, the habitual absence of an otoscope in many health institutions, particularly in poorer countries, restricts the ability of the health personnel to make more accurate diagnoses of OM.14 The cause and pathology of OM are complex.8,9 Pathogenic infection of the upper respiratory tract is the most significant factor. Virus or virus antigen was identified in the middle ear of 5% to 25% of individuals with AOM.10,11,15,16. Bacteria can be found in approximately 40% to 70% of patients.12,13,18,19 Moreover, a strong association was observed between the bacteria obtained from patients with middle ear OM and the major organisms found in the nasopharynx.20,21 Bacterial ear infections frequently develop after a throat infection, flu, or other respiratory system infections in children. If the upper respiratory infection is caused by a bacterium, this may travel to the middle ear. If the upper respiratory infection is viral, such as a cold, viruses may be attracted to the habitat of the microorganism and invade the middle ear as a serious infection. Fluid accumulates behind the eardrum because of the illness.22-24
Prompt, fast, and successful ear infection treatments can greatly reduce the short- and long-term consequences of ear infection. Furthermore, they can enhance the lives of patients. Thus, it is critical to have the most up-to-date data on the etiology of ear infection and associated antibiotic susceptibility pattern.25-27 Therefore, this study aimed to isolate and identify the most common bacteria causing OM in patients from the Misan governorate, Iraq, and exploring bacterial sensitivity to most commonly used antibiotics.
Sample Collection
A total of 150 patients diagnosed with OM by specialists at (name of a clinic) in Misan governorate, Iraq from January to April 2021 was included in this study. The patients were classified according to age, ranging from 14 to 50 years. Swab sample from an irritated area was collected using a sterile cotton swab. Samples were collected on patients who had not taken antibiotics for at least one week prior to swab collection.
Collection and Culturing of Ear Discharge
Firstly, the outer ear was cleaned using regular saline. Then, a sample of the discharge was collected. Swabs were subsequently inoculated onto MacConkey and blood agar plates, which were incubated aerobically at 37°C for 24–48 hours, and mannitol salt agar plates, which were incubated anaerobically at 37°C for 24–48 hours.28
Identification of Bacteria
Bacterial colonies were initially identified based on their phenotype and cultural characteristics. Identification of the isolated bacteria was performed according to standard microbiological methods, including cultural characteristics, Gram staining; biochemical reactions, such as catalase, indole urea media, oxidase; diagnostic tests, such as motility, hemolysis, and the triple sugar iron (TSI); and the VITEK 2 Compact.28,29
Measurement of Bacterial Sensitivity to Antibiotics
To evaluate the antibiotic susceptibility of bacteria isolated from patients with OM, we performed the procedures developed by.31 Briefly, Muller-Hinton agar was used for the experiment, except for S. pneumoniae isolates, which were grown on 5% blood agar medium. Samples were incubated at 37°C for 24 hours, and then the diameters of growth inhibition zones were measured.33 Antibiotic discs were chosen based on the frequency of prescription in the study region and the guidelines of the Clinical Laboratory Standards Institute (CLSI) and the European Association on Antibiotic Susceptibility (EUCAST).32,41 The following antibiotics ( Oxoid, UK) were used: amoxicillin (AMC, 30µg) plus clavulanic acid, penicillin G (P-10 U), amoxicillin (AX, 25µg), and trimethoprim (TMP, 10µg).
Study population
A total of 150 patients (age ranging from 14 to 50 years) with OM participated in this study. Of the patients, 50 (33.3%) were aged 14–22 years, 50 (16.6%) were aged 26–30 years, and 20 (13.3%) were aged 30–35 years. The least represented group was the age range 40-50 years, with only seven participants (4.6%) (Table 1).
Table (1):
Age distribution of study population.
Age range(years) |
Frequency (n) |
Percentage % |
|---|---|---|
14-22 |
50 |
33.3 |
22-26 |
30 |
20 |
26-30 |
25 |
16.6 |
30-35 |
20 |
13.3 |
35-40 |
18 |
12 |
40-50 |
7 |
4.6 |
Identification of Bacteria
Our results showed that the most dominant isolate was Staphylococcus aureus (45/150, 30%), followed by Pseudomonas aeruginosa (38/150, 25.5%). Streptococcus pneumoniae was identified in 20 cases (13.3%), whereas Klebsiella pneumoniae was isolated from 18 participants (12%). Escherichia coli and Staphylococcus epidermidis were the least frequent bacteria isolated from patients, with 16 (10.6%) and 13 (8.6%), respectively Table 2 and Table 3.
Table (2):
Diagnostic criteria of isolated bacteria.
Bacterial Isolates |
Gram Stain |
Catalase |
S.C. |
Indol |
Motility |
Ozidase |
TSI |
Haemolysis |
|---|---|---|---|---|---|---|---|---|
Staphylococcus aureus |
+ve |
+ve |
+ve |
-ve |
+ve |
-ve |
/ |
b |
Streptococcus pneumoniae |
+ve |
+ve |
+ve |
-ve |
+ve |
-ve |
/ |
b |
Pseudomonas aeruginosa |
-ve |
+ve |
+ve |
-ve |
V |
+ve |
R/R |
b |
Staphylococcus epidermidis |
+ve |
+ve |
+ve |
-ve |
V |
-ve |
/ |
y |
Escherichia coli |
-ve |
+ve |
-ve |
+ve |
V |
-ve |
Y/Y |
y |
Klebsiella pneumoniae |
-ve |
+ve |
+ve |
-ve |
-ve |
-ve |
Y/Y/ |
+ve – gram positive; -ve – gram negative; V – Variable; R – Red; Y Yellow; B – Beta; Y Gama
Table (3):
Bacterial types isolated from patients with OM.
Bacterial isolates |
Number |
Percentage % |
|---|---|---|
Staphylococcus aureus |
45 |
30 |
Streptococcus pneumoniae |
20 |
13.3 |
Pseudomomas aeruginosa |
38 |
25.3 |
Staphylococcus epidermidis |
13 |
8.6 |
Escherichia coli |
16 |
10.6 |
Klebsiella pneumoniae |
18 |
12 |
Antibiotic Sensitivity Test
The following antibiotics were used in this study: amoxicillin plus clavulinic acid (AmC 30 g), penicillin G (P-10 U), amoxicillin (AX-25 g), and trimethoprim (TMP 10 g). In general, all bacteria isolated in this study showed high sensitivity to amoxicillin (100%) and a relatively high sensitivity to trimethoprim (83%). Furthermore, 67% of the isolated bacteria were resistant to penicillin, whereas 50% of the isolates were resistant to amoxicillin Table 4.
Table (4):
Antibiotic resistance.
| Antibiotic Resistance (mm) | ||||
|---|---|---|---|---|
| AMC | AX | PG | TMP | |
| Staphylococcus aureus* | 10 | 9 | 8.5 | 10.5 |
| Streptococcus pneumoniae* | 10.5 | 7.5 | R | 8.5 |
| Pseudomonas aeruginosa** | 12.5 | R | R | R |
| Staphylococcus epidermidis* | 10 | 12.5 | 8.5 | 12.5 |
| Escherichia coli** | 13.5 | R | R | 15 |
| Klebsiella pneumoniae** | 12 | 10.5 | R | 12.5 |
| Sensitivity percent % | 100 | 50 | 33 | 83 |
| Resistance percent % | 0 | 50 | 67 | 17 |
*Gram positive bacteria; **Gram negative bacteria
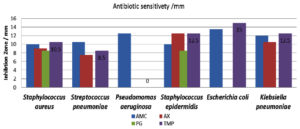
Overall, Gram-positive isolates were highly sensitive to the antimicrobials used, ranging from as low as 7.5 mm for Streptococcus pneumoniae sensitive to amoxicillin and as high as 12.5 mm for Staphylococcus epidermidis for amoxicillin and trimethoprim. Streptococcus pneumoniae was observed to be resistant to penicillin. For Gram-negative isolates, majority showed high resistance to almost all tested antibiotics. Pseudomonas aeruginosa were resistant to all tested antibiotics, except amoxicillin (12.5 mm), followed by Escherichia coli that reacted as 50% resistant to amoxicillin and penicillin, while showed 50 % sensitivity for amoxicillin (13.5mm) and for trimethoprim with 15 mm inhibition zone measure (Fig. 1).
Middle ear inflammation associated with OM is a common childhood and adult disease.34 This study enrolled 150 patients from the Misan governorate, Iraq, who were screened to determine the causative bacteria of OM and their susceptibility to several commonly used antibiotics. Additionally, we investigated the prevalence of OM across the examined age groups. The findings indicated that women (66%) had a higher prevalence of OM than men (44 %). This observation is consistent with35,36 who reported that females (66.1%) were more affected by OM than males (33.9 %). Several studies have demonstrated an equal prevalence of AOM in men and women, while numerous previous studies have indicated an increased incidence in boys. This could be a reflection of the environmental conditions (in-depth, recommended study) associated with the onset of OM symptoms.
Age is a significant factor in determining the percentage of OM infections. In the present study, the highest infected age group was 14–22 (33.3 %), followed by 22–26 (33.3 %) (20%). A low distribution of OM (4.6 %) was discovered in adults aged 40–50. Children are evidently more susceptible to OM due to their susceptibility to upper respiratory tract infections.37 reported that majority of their subjects were aged of 0–15 years, with 0–5 years accounting for 67.5%. This finding is consistent with the reasons children are more likely to contract OM than adults: children have a more vulnerable immune system and must fight off multiple infectious pathogens. Furthermore, the eustachian tube is a relatively small passageway. A child’s ear is shorter and more angular than that of an adult, making it more susceptible to blockage. Additionally, infection with adenoids may contribute to pathogen transmission into the eustachian tube.38 Other studies discovered that OM was the most prevalent disease in the first two years of children.39,40
Majority of the bacteria isolated in this study were Gram-positive (50 %), and the most common isolate was Staphylococcus aureus (30 %). Pseudomonas aeruginosa represented the majority with 25.3 percent. Similar findings were observed by Roland and Storman,42 who observed that Pseudomonas aeruginosa and Staphylococcus aureus were the most dominant bacterial pathogens in OM, and43-46,55 who reported that Pseudomonas aeruginosa and Staphylococcus aureus were the most common bacteria among patients with chronic OM.
S. pneumoniae represented 16% of infections isolated from Brazilian participants with severe otitis media, whereas S. aureus was responsible for only 1%.48 S. pneumoniae was the most frequently isolated pathogen from the middle ear of children with otitis media drug resistance with (39.69%), whereas S. aureus was recovered from 16.03 % of the participants.47 Geographical heterogeneity may be responsible for the differences in the distribution of bacteria.49
This study discovered that amoxicillin plus clavulanic acid (AmC 30 g) was 100% effective against most bacterial isolates from patients with OM, whereas trimethoprim TMP (10 g) was 83% effective. Amoxicillin is primarily bactericidal as a β-lactam antibiotic. It inhibits the third and final stages of bacterial cell wall synthesis by preferentially binding to a specific PBP found in the bacterial cell wall. As is the case with all β-lactam antibiotics, inhibition PBP-mediated cell wall synthesis results in cell lysis.50,51 Clavulanic acid is a β-lactamase inhibitor with negligible antimicrobial activity, and it acts as an effective “suicide” suppressor of a range of infectious β-lactamases mediated by plasmids and chromosomes.52 Pseudomonas aeruginosa exhibited the highest resistance to 75% of antibiotics tested but showed good sensitivity to amoxicillin. Escherichia coli was identified as the most susceptible isolate to trimethoprim (15 mm) and amoxicillin (13.5 mm). Antibiotic resistance is increasing worldwide as a result of antimicrobial misappropriation and overuse.53
A number of pediatricians and infectious disease organizations have recently launched a program to limit antibiotic use for competitive reasons.54,56 The Centers for Disease Prevention and U.S. Centers for Disease Control collaborated to review the prudent use of antimicrobial agents in infectious agents and recommend measures for potential pathogens, including those causing AOM.57,59 These guidelines emphasize the importance of limiting the use of antimicrobial agents. If these guidelines are adopted, the selective pressure caused by widespread antiviral use may be alleviated. Antimicrobial resistance is a significant challenge to international public health, and such guidelines may help reduce the therapeutic failures caused by drug-resistant bacteria.58
The findings of this study shed light on pathogenic bacteria that caused OM in patients from Misan, Iraq, and highlighted the phenomenon of antibiotic resistance, which has captured the interest of biological scientists, particularly microbiologists, in recent years. The most frequently isolated organism was Staphylococcus aureus, followed by Pseudomonas aeruginosa. Antibiotics, such as amoxicillin and trimethoprim, were the most efficient against most of the isolates. We firmly advocate for a nationwide antimicrobial surveillance to ensure appropriate antibiotic recommendations and rigorous adherence to antibiotic use policies and prevent the spread of drug-resistant bacteria and related consequences throughout the country, particularly in Misan.
ACKNOWLEDGMENTS
The authors would like to thank Al-Sadr teaching hospital staff for helping us collecting of specimens.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
All authors listed have made a substantial, direct and intellectual contribution to the work, and approved it for publication.
FUNDING
None.
ETHICS STATEMENT
Permission to conduct this study was issued by the Health institutional; Al-Sadr teaching hospital and the Swabbing from patients was carried out by a public health technician.
AVAILABILITY OF DATA
All datasets generated or analyzed during this study are included in the manuscript
- Hailegiyorgis T, Sarhie W, Workie H. Isolation and antimicrobial drug susceptibility pattern of bacterial pathogens from pediatric patients with otitis media in selected health institutions, Addis Ababa, Ethiopia: a prospective cross-sectional study. BMC Ear, Nose and Throat Disorders. 2018;18(1).
Crossref - Vanneste P, Page C. Otitis media with effusion in children: Pathophysiology, diagnosis, and treatment. A review. Journal of otology. 2019;14(2):33-9.
- Schilder AG, Chonmaitree T, Cripps AW, et al. Otitis media. Nature reviews Disease primers. 2016;8;2(1):1-8.
Crossref - Kong K, Coates HL. Natural history, definitions, risk factors and burden of otitis media. Medical Journal of Australia. 2009;191(S9):S39-43.
Crossref - Levy C, Varon E, Ouldali N, Wollner A, Thollot F, Corrard F, Werner A, Béchet S, Bonacorsi S, Cohen R. Bacterial causes of otitis media with spontaneous perforation of the tympanic membrane in the era of 13 valent pneumococcal conjugate vaccine. PLoS One. 2019;14(2):e0211712.
Crossref - Klein JO. Otitis externa, otitis media, and mastoiditis. Mandell, Douglas, and Bennett’s principles and practice of infectious diseases. 2015:767.
Crossref - Cripps AW, Kyd J. Bacterial otitis media: current vaccine development strategies. Immunology and cell biology. 2003 Feb;81(1):46-51. https://doi.org/10.1046/j.0818-9641.2002.01141.x
- Heikkinen T, Chonmaitree T. Importance of respiratory viruses in acute otitis media. Clinical microbiology reviews. 2003;16(2):230-41.
Crossref - Massa HM, Cripps AW, Lehmann D. Otitis media: viruses, bacteria, biofilms and vaccines. Medical journal of Australia. 2009;191(S9):S44-9.
Crossref - Marom T, Nokso-Koivisto J, Chonmaitree T. Viral–bacterial interactions in acute otitis media. Current allergy and asthma reports. 2012;12(6):551-8.
Crossref - Wiegand S, Berner R, Schneider A, Lundershausen E, Dietz A. Otitis externa: investigation and evidence-based treatment. Deutsches Ärzteblatt International. 2019;116(13):224.
Crossref - Ngo CC, Massa HM, Thornton RB, Cripps AW. Predominant bacteria detected from the middle ear fluid of children experiencing otitis media: a systematic review. PloS one. 2016;11(3):e0150949.
Crossref - Nogueira JC, Diniz MD, Lima EO, Lima ZN. Identification and antimicrobial susceptibility of acute external otitis microorganisms. Revista Brasileira de Otorrinolaringologia. 2008;74(4):526-30.
Crossref - Cilveti R, Olmo M, Pérez-Jove J, et al. Epidemiology of otitis media with spontaneous perforation of the tympanic membrane in young children and association with bacterial nasopharyngeal carriage, recurrences and pneumococcal vaccination in Catalonia, Spain-The Prospective HERMES Study. PLoS One. 2017;12(2):e0170316.
Crossref - Wasihun AG, Zemene Y. Bacterial profile and antimicrobial susceptibility patterns of otitis media in Ayder Teaching and Referral Hospital, Mekelle University, Northern Ethiopia. Springer Plus. 2015;4(1):1-9.
Crossref - Rybak A, Levy C, Bonacorsi S, et al. Antibiotic resistance of potential otopathogens isolated from nasopharyngeal flora of children with acute otitis media before, during and after pneumococcal conjugate vaccines implementation. The Pediatric Infectious Disease Journal. 2018;37(3):e72-8.
Crossref - Chirwa M, Mulwafu W, Aswani JM, Masinde PW, Mkakosya R, Soko D. Microbiology of chronic suppurative otitis media at queen Elizabeth central hospital, Blantyre, Malawi: a cross-sectional descriptive study. Malawi Medical Journal. 2015;27(4):120-4.
Crossref - Naziat H, Saha S, Islam M, et al. Epidemiology of otitis media with otorrhea among Bangladeshi children: baseline study for future assessment of pneumococcal conjugate vaccine impact. The Pediatric Infectious Disease Journal. 2018;37(7):715-21.
Crossref - Spoială EL, Stanciu GD, Bild V, Ababei DC, Gavrilovici C. From evidence to clinical guidelines in antibiotic treatment in acute otitis media in children. Antibiotics. 2021;10(1):52.
Crossref - Afolabi OA, Ologe FE, Nwabuisi C, Salaudeen AG, Ajiboye OT, Nwawolo CC. Correlation of Bacterial Isolates from Middle Ear and Nasopharynx in Patients with Chronic Suppurative Otitis Media in Ilorin, Nigeria. The Malaysian Journal of Medical Sciences: MJMS. 2015;22(5):23.
- Arola M, Ziegler T, Ruuskanen O. Respiratory virus infection as a cause of prolonged symptoms in acute otitis media. The Journal of pediatrics. 1990;116(5):697-701.
Crossref - Dasaraju PV, Liu C. Chapter 93: infections of the respiratory system. Galveston: University of Texas Medical Branch at Galveston. 1996.
- Chonmaitree T, Owen MJ, Howie VM. Respiratory viruses interfere with bacteriologic response to antibiotic in children with acute otitis media. Journal of Infectious Diseases. 1990;162(2):546-9.
Crossref - Pettigrew MM, Gent JF, Pyles RB, Miller AL, Nokso-Koivisto J, Chonmaitree T. Viral-bacterial interactions and risk of acute otitis media complicating upper respiratory tract infection. Journal of clinical microbiology. 2011;49(11):3750-5.
Crossref - Minovi A, Dazert S. Diseases of the middle ear in childhood. GMS current topics in otorhinolaryngology, head and neck surgery. 2014;13.
- Cohen BE, Durstenfeld A, Roehm PC. Viral causes of hearing loss: a review for hearing health professionals. Trends in hearing. 2014;18:2331216514541361.
Crossref - Giebink GS. The microbiology of otitis media. The Pediatric infectious disease journal. 1989;8(1):S21.
Crossref - Tadesse A, Alem M. Medical Bacteriology. EPHTI. Gondar University. 2006.
- Agha ZH, Al-Delaimi MS. Prevalence of common bacterial etiology and antimicrobial susceptibility pattern in patients with otitis media in Duhok Province–Iraq. Zanco Journal of Pure and Applied Sciences. 2021;33(4):11-25.
Crossref - Chauhan S, Surender. Clinico-Mycological Profile of Otomycosis in Chronic Suppurative Otitis Media Patients Attending a Tertiary Care Teaching Hospital. Journal of Pure and Applied Microbiology. 2021;15(2):813-9.
Crossref - Muleta D, Gebre-Selassie S. Isolation and antimicrobial susceptibility patterns of bacterial pathogens causing otitis media in children in Jimma Hospital, Southwestern Ethiopia. Ethiopian Journal of Health Sciences. 2004;14(2).
- Derese H, Mekonnen D, Awoke D, Wondemagegn M. na Bayeh, A. Profaili ya bakteria ya pathogen na mifumo ya uwezekano wa antimicrobial ya maambukizo ya sikio katika Kituo cha Maabara ya Utafiti wa Afya ya Mkoa wa Bahir Dar, Ethiopia. Springer Plus.; 2016;5:466.
- Banoon S, Ali Z, Salih T. Antibiotic resistance profile of local thermophilic Bacillus licheniformis isolated from Maysan province soil. Comunicata Scientiae. 2020;11:e3291.
Crossref - Korona-Glowniak I, Wisniewska A, Juda M, Kielbik K, Niedzielska G, Malm A. Bacterial aetiology of chronic otitis media with effusion in children-risk factors. Journal of Otolaryngology-Head & Neck Surgery. 2020;49(1):1-7.
Crossref - Al-Ani R. Prevalence of otitis media among Patients attending otorhinolaryngology clinic in Ramadi City/Iraq. Egyptian Journal of Ear, Nose, Throat and Allied Sciences. 2020;21(1):17-21.
Crossref - Al-Alousi M, Mayas N. Bacteria causing otitis media in some private and public centers in Thamar governorate-Yemen. Yemeni Journal for Medical Sciences. 2012;6.
- Mazlan R, Saim L, Thomas A, Said R, Liyab B. Ear infection and hearing loss amongst headphone users. The Malaysian journal of medical sciences: MJMS. 2002;9(2):17.
- Buzatto GP, Tamashiro E, Proenca-Modena JL, et al. The pathogens profile in children with otitis media with effusion and adenoid hypertrophy. PLoS One. 2017;12(2):e0171049.
Crossref - Roy E, Hasan KZ, Haque F, Siddique AK, Sack RB. Acute otitis media during the first two years of life in a rural community in Bangladesh: a prospective cohort study. Journal of health, population, and nutrition. 2007;25(4):414.
- Reed D, Dunn W. Epidemiologic studies of otitis media among Eskimo children. Public health reports. 1970;85(8):699.
Crossref - Weinstein MP, editor. Performance standards for antimicrobial susceptibility testing. Clinical and Laboratory Standards Institute; 2021.
- Roland PS, Stroman DW. Microbiology of acute otitis externa. The Laryngoscope. 2002;112(7):1166-77.
Crossref - Brook I, Frazier EH. Microbial dynamics of persistent purulent otitis media in children. The Journal of pediatrics. 1996;128(2):237-40.
Crossref - Ologe FE, Nwawolo CC. Prevalence of chronic suppurative otitis media (CSOM) among school children in a rural community in Nigeria. The Nigerian postgraduate medical journal. 2002;9(2):63-6.
- Bluestone CD. Pathogenesis and Epidemiology of chronic otitis media. InWHO/CIBA foundation workshop, report on prevention of hearing impairment for chronic otitis media held at CIBA foundation, London 1996 (pp. 14-17).
- Afolabi OA, Salaudeen AG, Ologe FE, Nwabuisi C, Nwawolo CC. Pattern of bacterial isolates in the middle ear discharge of patients with chronic suppurative otitis media in a tertiary hospital in North central Nigeria. African health sciences. 2012;12(3):362-7.
Crossref - Zielnik-Jurkiewicz B, Bielicka A. Antibiotic resistance of Streptococcus pneumoniae in children with acute otitis media treatment failure. International Journal of Pediatric Otorhinolaryngology. 2015;79(12):2129-33.
Crossref - Sih TM. Acute otitis media in Brazilian children: analysis of microbiology and antimicrobial susceptibility. Annals of Otology, Rhinology & Laryngology. 2001 Jul;110(7):662-6. Crossref
- Rosenblüt A, Santolaya ME, González P, et al. Bacterial and viral etiology of acute otitis media in Chilean children. The Pediatric infectious disease journal. 2001;20(5):501-7.
Crossref - Min HK, Kim SH, Park MJ, Kim SS, Kim SH, Yeo SG. Bacteriology and resistance patterns of otitis media with effusion. International Journal of Pediatric Otorhinolaryngology. 2019;127:109652.
Crossref - Chung HS, Yao Z, Goehring NW, Kishony R, Beckwith J, Kahne D. Rapid β-lactam-induced lysis requires successful assembly of the cell division machinery. Proceedings of the National Academy of Sciences. 2009;22;106(51):21872-7.
Crossref - Privalsky TM, Soohoo AM, Wang J, et al. Prospects for Antibacterial Discovery and Development. Journal of the American Chemical Society. 2021;3;143(50):21127-42.
Crossref - Tesfa T, Mitiku H, Sisay M, et al. Bacterial otitis media in sub-Saharan Africa: a systematic review and meta-analysis. BMC infectious diseases. 2020;20(1):1-2.
Crossref - Fanelli U, Chiné V, Pappalardo M, Gismondi P, Esposito S. Improving the quality of hospital antibiotic use: Impact on multidrug-resistant bacterial infections in children. Frontiers in Pharmacology. 2020;11:745.
Crossref - Al-Alousi M, Mayas N. Bacteria causing otitis media in some private and public centers in Thamar governorate-Yemen. Yemeni Journal for Medical Sciences. 2012;6.
- Caron WP, Mousa SA. Prevention strategies for antimicrobial resistance: a systematic review of the literature. Infection and drug resistance. 2010;3:25.
Crossref - Damoiseaux RA. Antibiotic treatment for acute otitis media: time to think again. Cmaj. 2005;172(5):657-8.
Crossref - Prestinaci F, Pezzotti P, Pantosti A. Antimicrobial resistance: a global multifaceted phenomenon. Pathogens and global health. 2015;109(7):309-18.
Crossref - Frost HM, Lou Y, Keith A, Byars A, Jenkins TC. Increasing guideline-concordant durations of antibiotic therapy for acute otitis media. The Journal of Pediatrics. 2022;240:221-7.
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.