ISSN: 0973-7510
E-ISSN: 2581-690X
In developing countries due to lack of sanitary practices, poor socioeconomic conditions and huge population burden, intestinal parasitic infections continue to be a major public health problem. The present study was done to determine the prevalence of Intestinal parasitic infections (IPI) among patients attending our tertiary care rural hospital. The study was conducted for a duration of 3 years at R L Jalappa Hospital and Research Centre, Kolar. Retrospective data of samples sent for stool microscopy were collected from laboratory records and were analyzed. During the study period, 62 out of 892 patients were screened positive for intestinal parasitic infections. The most common parasite observed was Entamoeba histolytica (5.3%) followed by Hookworm (1.2%), Ascaris lumbricoides (0.4%), Strongyloides stercoralis (0.1%), and Taenia species (0.1%). Findings of our study show that intestinal parasitic infections continue to be a burden, hence regular screening is essential to know the common parasites causing infections. Improved sanitation, safe drinking water practices, and health education are essential for prevention.
Helminths, Intestinal parasitic infections, Protozoans, Haemoglobin, South India, Prevalence
Intestinal parasitic infections (IPI) are the major public health problems in developing countries.1 Most common parasites causing IPI include Ascaris lumbricoides, Entamoeba histolytica, Toxoplasma gondii, Cyclospora species, Giardia lamblia, and Cryptosporidium species.2 They are transmitted by feco-oral route by contaminated soil in areas with poor sanitary practices. Worldwide approximately 1.5 billion people are affected by soil-transmitted helminths. The high prevalence of infection by IPI is associated with poor environmental hygiene and poverty. These issues are distributed widely in tropical and subtropical areas, with large numbers occurring in sub-Saharan Africa, America, China, and East Asia.3 A diverse parasitic combination is observed in different regions of India. Hookworm infestations are common in South India compared to Trichuris trichiura and Ascaris lumbricoides.4 Infections due to IPI may lead to significant illnesses such as iron deficiency anemia, vitamin deficiencies, poor performance, and cognitive outcomes, especially in children.5 Prevalence data from community studies are much more informative for public health, however, hospital-based studies may also impart the data to a certain extent. Hence the present study was carried out to determine the prevalence of IPI among patients attending a tertiary care rural hospital in Karnataka.
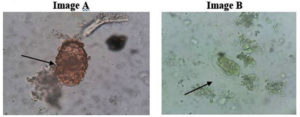
The study was conducted at the department of Microbiology, R L Jalappa Hospital, Kolar, India for a duration of 3 years (July 2018 to June 2021). All the stool samples sent to the Microbiology department from clinically indicated patients from both the outpatient departments and inpatient wards were included in the study. Duplication of samples sent from the same patients with the same reports were excluded. Demographic data of patients and details of stool microscopy were collected from laboratory records. As a routine microbiological procedure stool samples collected were subjected to the macroscopic examination which included naked eye examination for its consistency, presence of mucus, blood, segments of parasites, or helminths, and then were subjected to microscopic examination. The microscopic method was done using normal saline and Lugol’s iodine wet mount preparations (Figure 1). Modified Ziehl Neelsen stain (Modified ZN stain) was done for screening opportunistic coccidian parasites following the clinician’s request as per the standard microbiological techniques.6,7 Ethical clearance was obtained before the start of the study from the Institutional Ethics Committee, SDUAHER, Kolar, Karnataka.
Statistical Analysis
Data was entered and analyzed using Microsoft excel. Descriptive statistics were used to summarize the results and quantitative data was expressed using percentages in figures and tables.
Over 3 years out of 892 patients screened, 62 patients were positive for IPI with a prevalence rate of 6.9%(62/892). The most common parasite observed was Entamoeba histolytica (5.3%) followed by Hookworm (1.2%), Ascaris lumbricoides (0.4%), Strongyloides stercoralis (0.1%), and Taenia (0.1%) as shown in Table 2. From 892 patients screened for IPI, 60 patients (99.77%) were found to have single parasitic infections, and 2 patients (0.22%) had multiple parasitic infections. Around 28 patients were screened for opportunistic coccidian parasites using modified ZN stains, and none of them were positive.
Table (1):
Age wise distribution of Intestinal parasitic infections.
Age group |
Total patients screened for IPI |
No. of patients screened positive for IPI |
|---|---|---|
0-10 years |
159 |
3 (1.9%) |
11-20 years |
64 |
5 (7.8%) |
21-30 years |
141 |
10 (7.09%) |
31-40 years |
136 |
8 (5.9%) |
41-50 years |
165 |
8 (4.8%) |
51-60 years |
108 |
12 (11.1%) |
Above 60 years |
119 |
15 (12.7%) |
Total |
892 |
62 (7%) |
* IPI- Intestinal parasitic infections
Table (2):
Prevalence of Intestinal parasitic infections.
Parasites identified |
No. of parasites identified (%) |
|---|---|
Entamoeba histolytica |
47 (5.3%) |
Hookworm |
10 (1.2%) |
Ascaris lumbricoides |
04 (0.4%) |
Strongyloides stercoralis |
01 (0.1%) |
Giardia lamblia |
01 (0.1%) |
Taenia |
01 (0.1%) |
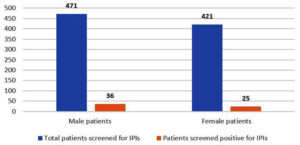
Of 892 patients screened for intestinal parasites, the age of the patients varied from 1 year to a maximum of 88 years. Concerning the age, 10 years intervals of stratification maximum number of samples were from the age group of 41-50 years (18.5%) followed by 0-10 years (17.8%), age-wise distribution of samples received is shown in Table 1. Concerning the gender-wise distribution of samples out of 892 patients, 471 patients (52.80%) were males and 421 patients (47.19%) were females (Figure 2).
Hemoglobin levels of patients affected with IPI were collected from the laboratory records and only 56 out of 62 patients’ details were available. Out of 56 patients, 6 patients (18.18%) had severe anemia, 11 patients (33.33%) had moderate anemia, 16 patients (18.18%) had mild anemia and 23 patients were not anemic. Age-wise distribution of patients showed that 12 patients (36.36%) aged above 60 years were anemic and the percentage of patients with IPI having anemia was less among children.
In developing countries like India, intestinal parasitic infections (IPI) are more prevalent and studies on the distribution of IPI will help in planning treatment. During the 3 years of study period, the prevalence of IPI in our hospital was 6.9%. The overall prevalence of pathogenic IPIs in India ranges between 12.5% to 91%. When compared to other studies done in India and other developing countries it was low.8,9 In a hospital-based retrospective study done at Vellore the prevalence of IPI was 8.9% which is almost near to our findings.10 The difference in the prevalence of IPI in various regions may depend on the number of samples examined per patient, use of stool concentration techniques, various sampling methods, time of the study, and geographical difference in the area.11 Microscopy using fresh stool samples is considered to be the gold standard test for the identification of IPI. However, a study from Hyderabad suggested that formal ether sedimentation techniques had increased the prevalence rates when compared to direct microscopic methods.12 In our study, direct microscopic methods were used which may be one of the reasons for the low prevalence of IPI.
In our study modified ZN stain was used to identify coccidian intestinal parasites like Cryptosporidium species, Isospora species, and Cyclospora species. A concentration of at least 50,000 to 5,00,000 oocysts per gram of stool is required for 100% detection of coccidian intestinal parasites.13 However, no coccidian intestinal parasites were identified during our study period.
In our study, a slightly higher proportion of male patients were positive for intestinal parasitic infections compared to female patients (7.7% versus 5.9%). Males were found to be more predisposed to intestinal parasitic infections which may be due to their occupation, increased susceptibility to some parasites due to immunomodulatory effects of the hormone testosterone.14,15
The highest prevalence of IPI in our study was in the age group of 51-60 years (11.1%) and >60 years (12.7%). The prevalence of IPI among the age group of 0 to 10 years was 1.9% and 11 to 20 years was 7.8%. Higher prevalence rates of IPI among adults were also observed in other studies of India.16,17 It is observed that the prevalence among children aged between 0 to 10 years was low which could be due to an effective deworming program by the Ministry of Health and Family Welfare initiated in 2015. Also, it is the world’s largest school-based deworming program, targeting a population of around 240 million children aged between 1 year to 19 years.18
Protozoan parasitic infections are predominant in our study when compared to helminthic infections. Out of 62 patients screened, 48 patients (77.41%) had protozoan parasites and 16 patients (25.80%) had helminthic parasites. In a study done by Saurabh K et al in Rajasthan, 95.38% were protozoan parasites and 4.62% were helminthic parasites which are almost similar to our findings.17 Other studies in India also observed protozoan parasites as a predominant parasite causing IPI.19-22 In our study most common protozoan parasite identified was Entamoeba histolytica (47 patients), and the most common helminthic parasite was Hookworm (10 patients). The high prevalence of Entamoeba histolytica could be due to exposure to unclean food and water. Improved sanitary practices such as hand washing techniques, fly control, safe drinking water facilities may help in preventing the parasitic infestations. According to the World Health Organization (WHO), Entamoeba histolytica affects around 500 million individuals worldwide; 50 million of them have invasive diseases. It is the fourth leading cause of mortality due to parasitic infections.23,24 In endemic areas intestinal carriers of Entamoeba histolytica range between 5 to 50%. Among these intestinal carriers, 10% of them may develop invasive dysenteric bowel disease, 0.5% may develop extraintestinal disease, liver abscess being the most common; 2% to 4% of those with a liver abscess may die. In patients with fulminant colitis, a death rate of up to 70% can be seen.25 In our study, intestinal protozoan parasitic infection is more when compared to helminthic parasites. Commensal protozoan parasites should also be considered and need to be correlated clinically as they reflect the sanitary conditions and socioeconomic status.
We could find only a few helminthic infections in our study which included Hookworm Roundworm, Strongyloides stercoralis, and Taenia species. In our study, the prevalence of Hookworm infection is 1.2% and the infection was more common among the adult population than in the children. In a study done by Kaliappan et al in a tribal area of south India, an increasing prevalence of Hookworm infection with increasing age was observed.26 Moderate to heavy intensity hookworm infections are linked with low hemoglobin levels and anemia, especially in pregnant women and young children.18 Identification of eggs of hookworm in patients’ samples is very important, further quantitative counts should be made, because the potentially severe disease may be associated with this nematode in heavy infection. Even light infection has been linked to serious sequelae secondary to chronic anemia.25,18
In our study, Strongyloides stercoralis was found in a 65 years female patient and was found to be HIV positive. Strongyloidiasis in humans may be from asymptomatic to chronic symptomatic strongyloidiasis. Uncontrolled multiplication of this parasite can cause life threatening disease like Loeffler’s pneumonia in immunocompromised patients high mortality rates of up to 85% is observed. Although stool examination of the larva is required for definitive diagnosis, newer diagnostic tests like immunoassays and molecular tests can also be used.27
Multiple parasitic infections in our study were less common, only 2 patients out of 62 patients screened were positive accounting to 3.22%. A 11 years female patient was found to be positive for both Giardia and Entamoeba histolytica and another male patient aged 21 years was positive for Hookworm and Taenia species. Few other studies were done in India also observed multiple parasitic infections of 8.9% to 13.3%.17,20 In a study done by Mehraj et al, 10% of children screened had two or more than two intestinal parasites.28
In another study done by Sayasone S et al 86.6% of the study participants had two or more intestinal parasitic infections concurrently.29 In a study done by Jayaram S et al, out of 187 participants, 25(13.4%) had parasitic infections and among them 12(6.4%) had soil transmitted helminthic infections and 13(6.9%) had intestinal protozoan parasites.30 In another done by Husen EA et al. out 404 school children screened, overall prevalence of intestinal parasitic infections is 33.91% (137/404). Double infection rate was found to be 2.72%(11/404). Most common parasite was Ascaris lumbricoides (8.9%), followed by Hymenolepis nana (7.7%), Taneia species (5.4%), Hookworm(4.7%), Trichuris trichura (2.5%), Schistosoma mansoni (2.2%), Enterobius vermicularis (1.7%) and Strongyloides stercoralis(0.7%).31
Few limitations of the study includes, other details of the patients like socioeconomic status, eating habits, sanitary practices, and other risk factors could not be collected as it is a retrospective study. The findings of our study could only be the tip of the iceberg, as only symptomatic patients who presented to the hospital were screened. A community-based study is always a better indicator compared to a hospital-based study to know the true burden.
The findings of our study will add knowledge to the existing data and indicate that regular screening of intestinal parasitic infections is essential to plan treatment strategies. Such regular screening should also be extended towards the population in the community as it reflects the actual burden.
There was a high occurrence of protozoan parasitic infections compared to helminths, which could be due to the effective National deworming program and Swachh Bharat Abhiyan initiated by the Government of India. The National deworming program concentrates the population aged between 1 year to 19 years and the other age groups are not treated. Thus, the population more than 19 years who are infected with intestinal parasites and also asymptomatic carriers may serve as a source of infection.
ACKNOWLEDGMENTS
Authors are thankful to technicians of the Department of Microbiology, who assisted in data collection.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
All authors have made a direct, substantial, and intellectual contribution to the work, and approved it for publication.
FUNDING
None.
ETHICS STATEMENT
The study was approved by the Institutional Ethics Committee, Sri Devaraj Urs Medical College, Tamaka, Kolar, India with reference number DMC/KLR/IEC/209/2021-22.
DATA AVAILABILITY
The datasets generated and/or analysed during the current study are available from the corresponding author on reasonable request.
- Brooker S, Hotez PJ, Bundy DAP. Hookworm-related anaemia among pregnant women: A systematic review. PLoS Negl Trop Dis. 2008;2(9):e291.
Crossref - Alum A, Rubino JR, Ijaz MK. The global war against intestinal parasites-should we use a holistic approach? Int J Infect Dis. 2010;14(9):e732-738.
Crossref - WHO. Soil transmitted infection. 2022. https://www.who.int/news-room/fact-sheets/detail/soil-transmitted-helminth-infections
- Parija SC, Chidambaram M, Mandal J. Epidemiology and clinical features of soil-transmitted helminths. Trop Parasitol. 2017;7:81-85.
- World Health Organization. Preventive Chemotherapy to Control Soil-Transmitted Helminth Infections in at-Risk Population Groups: Guideline. Geneva: WHO; 2017. http://www.who.int/nutrition/publications/guidelines/deworming/en/
- Collee JG, Duguid JP, Fraser AG, Marmion BP, Simmons A. Mackie & McCartney Practical Medical Microbiology. 14th edition; Protozoa & Helminthes. New Delhi, Churchill Livingstone Elsevier, 2007;42 & 43:721-791.
- Patrica M Tille. Bailey & Scott”s Diagnostic Microbiology; 14th edition, Overview of methods and strategies in Parasitology. Canada, Elsvier. 2014;46:601-626.
- Kang G, Mathew MS, Rajan DP, et al. Prevalence of intestinal parasites in rural Southern Indians. Trop Med Int Health 1998;3(1):70-75.
Crossref - Waikagul J, Krudsood S, Radomyos P, et al. A cross-sectional study of intestinal parasitic infections among schoolchildren in Nan Province, Northern Thailand. Southeast Asian J Trop Med Public Health. 2002;33(2):218-223. PMID: 12236415
- Praharaj I, Sarkar R, Rao Ajjampur SS, Roy S, Kang G. Temporal trends of intestinal parasites in patients attending a tertiary care hospital in south India: A seven-year retrospective analysis. Indian J Med Res. 2017;146(1):111-120.
Crossref - Teja SS, Swarna SR, Jeyakumari D, Kanna V. A study on intestinal parasitic infections among school children in Karaikal. Trop Parasitol. 2020;10(2):79-85.
Crossref - Venkatesh BMS, Rao SR, Vivekanand N. A comparative study of concentration techniques for detection of Intestinal parasitic infections – To evaluate the prevalence and to identify a better method of concentration technique at a tribal tertiary care hospital. IOSR J Dent Med Sci. 2016;15(07):42-46.
Crossref - Ricciardi A, Momar N. Diagnosis of parasitic infections: Whats going on? J Biomol Screen. 2015;20:6-21.
Crossref - Lifson AR, Thai D, O’Fallon A, Mills WA, Hang K. Prevalence of tuberculosis, hepatitis B virus, and intestinal parasitic infections among refugees to Minnesota. Public Health Rep 2002;117(1):69-77.
Crossref - Klein SL. Hormonal and immunological mechanisms mediating sex differences in parasite infection. Parasite Immunol. 2004;26(6-7):247-264.
Crossref - Singh R, Singla P, Sharma M, Chaudhary U. Original research article prevalence of intestinal parasitic infections in a tertiary care hospital in Northern India: Five-year retrospective study. Int J Curr Microbiol Appl Sci. 2013;2(10):112-117.
- Saurabh K, Nag VL, Dash S, et al. Spectrum of Parasitic Infections in Patients with Diarrhoea Attending a Tertiary Care Hospital in Western Rajasthan, India. J Clin Diagn Res. 2017;11(8):DC01-DC04.
Crossref - Ajjampur SSR, Kaliappan SP, Halliday KE, et al. Epidemiology of soil transmitted helminths and risk analysis of hookworm infections in the community: Results from the DeWorm3 Trial in southern India. PLoS Negl Trop Dis. 2021;15(4):e0009338.
Crossref - Paul RC, Das NC, Rao CK, Joshi M, Mathur A. Prevalence of intestinal parasites in three villages of Dungarpur district, Rajasthan. J Commun Dis. 1982;14(2):149-151. PMID: 7153483
- Choubisa SL, Jaroli VJ, Choubisa P, Mogra N. Intestinal parasitic infection in Bhil tribe of Rajasthan, India. J Parasit Dis. 2012;36(2):143-148.
Crossref - Kavathia G, Pattani M, Dharsandiya M, Chaudhary A, Joshi T. A prevalence study of intestinal parasitic infections in a Tertiary Care hospital in Rajkot city of Gujarat (India): A hospital-based study. IOSR J Dent Med Sci. 2015;14(10):45-47.
- Marothi Y, Singh B. Prevalence of intestinal parasites at Ujjain, Madhya Pradesh, India: Five-year study. Afr J Microbiol Res. 2011;5(18):2711-2714.
Crossref - Cui Z, Li J, Chen Y, Zhang L. Molecular epidemiology, evolution, and phylogeny of Entamoeba spp. Infect Genet Evol. 2019;104018.
Crossref - Tharmaratnam T, Kumanan T, Iskandar MA, et al. Entamoeba histolytica and amoebic liver abscess in northern Sri Lanka: a public health problem. Trop Med Health. 2020;48:2.
Crossref - Winn W, Allen S, Janda W, et al. Koneman’s color Atlas and Textbook of Diagnostic Microbiology.6 th edition, Baltimore(MD); Lippincott Williams and Wilkins. Parasitology. 2006;22:1256-1262.
- Kaliappan SP, George S, Francis MR, et al. Prevalence and clustering of soil-transmitted helminth infections in a tribal area in Southern India. Trop Med Int Health. 2013;18(12):1452-1462.
Crossref - Nutman TB. Human infection with Strongyloides stercoralis and other related Strongyloides stercoralis and other related Strongyloides species. Parasitology. 2017;144(3):263-273.
Crossref - Mehraj V, Hatcher J, Akhtar S, Rafique G, Beg MA. Prevalence and factors associated with intestinal parasitic infection among children in an urban slum of Karachi. PLoS One. 2008;3(11):e3680.
Crossref - Sayasone S, Mak TK, Vanmany M, et al. Helminth and intestinal protozoa infections, multiparasitism and risk factors in Champasack province, Lao People’s Democratic Republic. PLoS Negl Trop Dis. 2011;5(4):e1037.
Crossref - Jayaram S, Saya GK, Rajkumari N, Ulaganeethi R, Roy PK, Mathavaswami V. Prevalence of intestinal parasitic infection and its associated factors among children in Puducherry, South India: a community-based study. J Parasit Dis. 2021;45(4):897-902.
Crossref - Husen EA, Tafesse G, Hajare ST, Chauhan NM, Sharma RJ, Upadhye VJ. Cross-Sectional Study on Assessment of Frequency of Intestinal Helminth Infections and Its Related Risk Factors among School Children from Adola Town, Ethiopia. BioMed Research International. 2022;2022:5908938.
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.