ISSN: 0973-7510
E-ISSN: 2581-690X
Multi – drug resistant (MDR) P. aeruginosa had emerged in Iraq and seen mainly in the hospitals is due to the selective pressure by over usage of antibiotics. P. aeruginosa considered as a serious therapeutic challenge for treatment of both nosocomial and community-acquired infections. For this reason the selection of the appropriate antibiotic to initiate therapy is essential to optimizing the clinical outcome 1,2. The recent research was design to detect and characterized the antibiotic resistant patterns of P. aeruginosa and also to detect the presence of bacterial plasmid of multiple antibiotic resistant strains that’s obtained from clinical burns samples in Baghdad, against some of the commonly prescribed antibiotics. Out of 52 Pseudomonas aeruginosa isolates were collected from 152 burns swabs at two teaching hospitals in Baghdad city. Purified isolates of diagnosed P.aeruginosa were underwent to various morphology, biochemical tests, antibiotic sensitivity testing by using discs diffusion method as recommended and developed by CLSI. Only the seventieth MDR bacterial isolates were underwent for profiling of plasmid. Fourteen different antibiotics discs will be use to detect the drug susceptibility and bacterial isolates resistance pattern , and the plasmid will be extracted by using commercial plasmid isolation kit ( Promega company / USA) and electrophoresis of the plasmid will be done by using o.8% agarose gel. The examined isolates were expressed resistance pattern as following: Piperacillin 2 (3.84%); Ciprofloxacin 6 (11.53%); Aztreonam 8(15.38%), Ceftazidime 9(17.30%); Amikacin 10 (19.23%); Levofloxacin 10 (19.23%); Gentamycin 12(23.07%); Meropenem 15(28.84%); Mezlocillin 20(38.46%); Tetracycline 37(71.15%); Imipenem 22 (42.30%); Trimethoprim – sulfamethoxazol 32(61.53%); Nalidixic acid 46(88.46%); and Amoxicillin 49(94.23. The result of the plasmid profiling has been revealed that there were five detectable plasmids 5 (29.41) out of 17 MDR P. aeruginosa isolates while, the remaining twelve (70.58%) bacterial isolates were lacked plasmid. Four isolates ( 23.52%) isolates expressed single sized plasmid (550 – 800bp) and only one (5.88%) isolate was expressed double plasmids between (550-940 bp) The present study was determined the dangerous of MDR P. aeruginosa and it constitute a major and strict problem in our hospitals. Eradication and control methods should be used to avoid and prevent the spreading of this threat. In addition, avoid over usage of any antibiotic to overcome the evolution of resistance. The combination of antibacterial sensitivity test with detection of the plasmid might be the easiest, cheapest, and effective method for clarifying the origin of infection
Plasmid profiling, Multi – drug Resistant, Pseudomomnas aeruginosa.
Pseudomonas aeruginosa, is widely distributed in the nature, it is a non-fermentative gram negative bacterium including water, soil and hospitals environment. It is responsible for about 10% -20% of nosocomial infections which are seen as septicaemia in intensive-care units (ICUs), cystic fibrosis, burn and wound infections, etc.3 Pseudomonas aeruginosa bacterium exhibited a wide spreading that can acquire resistance rapidly to many and various broad -spectrum antibacterial agents (antibiotics). Multidrug resistant (MDR) of P. aeruginosa is an emerging and a major cause of morbidity and mortality in burns patients, which leading to (4 – 60%) nosocomial infections in various parts of the world 4. Multidrug resistant P. aeruginosa (MDR) phenotype can be defined as a bacterium which exhibited a major resistant to antimicrobial drugs which are consist of three or more antiPseudomonal antimicrobial classes (penicillins; carbapenems; aminoglycosides; fluoroquinolones, and cephalosporins 5 .
Pseudomonas aeruginosa nosocomial infections is generally difficult to killed because of the possibility intrinsic resistance and its ability to obtain faster resistance mechanism against many groups of antimicrobials6. In other study, P. aeruginosa strains isolated was showed resistance to gentamicin and carbenicillin. P. aeruginosa is intrinsically less susceptible to the fluoroquinolones and usually it is moderately susceptible or resistant7. MDR P. aeruginosa produced inactivating enzymes that in turn make the beta-lactams and carbapenems ineffective and in active, such as metallolactamases (MBLs) and extended spectrum beta lactamases (ESBLs)8. Extended spectrum beta lactamases (ESBLs) P. aeruginosa was first investigated in western Europe in the mid-1980s, and MBL-producing P. aeruginosa was first detected in Japan in 1991. They have rapidly spread over area of various world since then9.
The spreading of resistant gene at a higher rate suspected as the source of elevating antibiotic resistance cases in it. Plasmid carry genes that could be spread by conjugation and transduction while the genome based resistant genes are also spread by replication. Plasmid profile was detected the total plasmid content, or subjects plasmids to restriction endonucleases and separates the cleaved plasmid DNA by electrophoresis for analysis. This method is a strength strategy for following the spread of antibiotic resistance, since resistance is usually transported between bacteria on plasmids 10 .
A total of 152 clinical burns specimens were collected by using a sterilized swabs from Alkindy and Al- Yarmuk Tertiary Hospitals in Baghdad city. The burns swabs were collected between September 2016 to July 2017. 2.2
Cultural methods
By using permanent marker the bottom of each plates of cultural media were labeled ; the total samples were cultured on the MacConkey and Blood agar agar plates and immediately incubated at 37°C for 24 to 48 hour depending on the nature of the sample. The identification and detection of the fifty two bacterial isolates as P. aeruginosa was depended on a combination of colonial morphology, Gram stain features and biochemical tests such as oxidase and catalase tests, and were confirmed by culuring them on the selective and differential agar media for P. aeruginosa called citromid agar media then incubated at 37°C for 24 hr.
Antimicrobial sensitivity testing
Susceptibility and resistance pattern were performed on each of 52 isolates by using agar disc diffusion method on Mueller – Hinton agar described by Kirby Bauer method11 according to the recommendations of the NCCLS 12and by using the following antibiotics: Amoxicillin (AML), Erythromycin (ERY), Nalidixic acid (NA), Ceftazidime (CAZ), Ciprofloxacin (CIP), Aztreonam (ATM), Mezlocillin (MEZ) Imipenem (IPM), Trimethoprim- sulfamethoxazol (STX),Tetracycline (TET), Amikacin (AK), Gentamycin (GEN), Piperacillin ( PIP), and Levofloxacin (LVX).
To investigate the antibiotics sensitivity and resistance for the selected isolate, 100 µl of each purified bacterial isolate was inoculated to the prepared 10 ml of nutrient broth and incubated at 37°C to mid log phase. One hundred µl of each inoculated bacterial isolate was streaked on Mueller- Hinton agar plates, the selected antibiotics discs were placed over the surface of inoculated plates then were incubated at 37°C for 18-24 hr.
After incubation the inhibition zone diameter of each disc was measured and registered, then compared with inhibition zone diameter interpretative chart to determine the sensitivity of isolates to antibiotics13. The multi – resistant isolate that expressed resistant to more than one antibiotic were taking for plasmid DNA profiling.
Plasmid extraction and profiling
Prepare Lysate
Plasmid extraction was done using a commercial plasmid kit (Plasmid Miniprep Kit, Promega Co.USA) and depending on the manufacture instructions: 600µl of lauria broth was prepared and used for growing each one of bacterial isolate, then added to a 1.5 ml microcentrifuge tube. Cell lysis buffer (Blue) at a size of 100µl was added, and mixed by inverting the microcentrifuge only tube 6 times. Then 350µl of cold (4-8°C) neutralization solution was added, and strongly mixed by inverting. micro centrifuges were Centrifuged at a higher speed in for 3 minutes. The supernatant of each tube was transfer (~900µl) to a Minicolumn (PureYield™ ) carefully without disturbing the pellet of the cell debris. The minicolumns were putted inside the collection tubes, and at maximum speed were centrifuged in a microcentrifuge for only 15 seconds. The minicolumns were placed into the same collection tubes, while the follow-throughs were discarded and wash.
Wash
Endotoxin removal wash (ERB) were added at 200 µl to the minicolumn. The minicolumn were centrifuged in a microcentrifuge at maximum speed for 15 seconds then column wash solution (CWC) at 400µl were added to the minicolumns. In a microcentrifuge were centrifuged at maximum speed for 30 seconds.
Elute
Elute The minicolumns were transmitted to a clean 1.5 ml microcentrifuge tubes, then 30µl of elution buffer was added directly to the minicolumn – matrix. Each tube lets it to stand for one minute at room temperature. The plasmid DNA was eluted by centrifuge for 15 seconds to. The eluted plasmid DNA was stored at -20°C and microcentrifuge tubes were capped.
Agarose gel electrophoresis
Following DNA plasmid extraction from the bacterial cells, agarose gel at 0.8% was prepared with wells, in which loading dye at 2ul was mixed with 10 ul of the 1000 base pair DNA markers and transmitted into the first well. The sample was mixed with 2 ul of the loading dye it was transmitted into the other wells. The ethidium bromide was used for staining the gel, and agarose gel electrophoresis was done on the plasmid DNA at 90 v for 1 hr. Then examined under UV Trans-illuminetion for the band harboring plasmid.
All the 52 P. aeruginosa bacterial isolates were subjected for sensitivity test by using 14 different antimicrobial agents. The antibiotic resistant and sensitivity patterns of the P. aeruginosa isolates that obtained from clinical burns swabs was expressed by table (1).The resistance and sensitivity pattern of the tested isolates were as following: Piperacillin 2 (3.84%); Ciprofloxacin 6 (11.53%); Aztreonam 8(15.38%), Ceftazidime 9(17.30%); Amikacin 10 (19.23%); Levofloxacin 10 (19.23%); Gentamycin 12(23.07%); Meropenem 15(28.84%); Mezlocillin 20(38.46%); Tetracycline 37(71.15%); Imipenem 22 (42.30%); Trimethoprim – sulfamethoxazol 32 (61.53%); Nalidixic acid 46(88.46%); and Amoxicillin 49(94.23).
Table (1):
Antibiotics sensitivity tests of 52 P. aeruginosa clinical burns isolates by disc diffusion method
| Type of antibiotic | Conc. µg | R | S | No. | % | |
|---|---|---|---|---|---|---|
| No. | % | |||||
| Piperacillin | 100 | 2 | 3.85 | 50 | 96.15 | |
| Ciprofloxacin | 5 | 6 | 11.54 | 46 | 88.46 | |
| Aztreonam | 30 | 8 | 15.39 | 44 | 84.61 | |
| Ceftazidime | 30 | 9 | 17.31 | 43 | 82.69 | |
| Levofloxacin | 5 | 10 | 19.24 | 42 | 80.76 | |
| Amikacin | 30 | 10 | 19.24 | 42 | 80.76 | |
| Gentamycin | 10 | 12 | 23.08 | 40 | 76.92 | |
| Mezlocillin | 75 | 20 | 38.47 | 32 | 61.53 | |
| Imipenem | 10 | 22 | 42.31 | 30 | 57.69 | |
| Trimethoprim-sulfamethoxazol | 125/23.7 | 32 | 61.54 | 20 | 38.46 | |
| Erythromycin | 10 | 35 | 67.31 | 17 | 32.69 | |
| Tetracycline | 25 | 37 | 71.16 | 15 | 28.84 | |
| Nalidixic acid | 30 | 46 | 88.47 | 6 | 11.53 | |
| Amoxicillin | 25 | 49 | 94.24 | 3 | 5.76 | |
Antibacterial resistant profile of the tested 52 P. aruginosa isolates was suggested that 17 (32.69%) isolates were resistant to at least five or more antibacterial agents. P38,P40,P42 were resistant to (12) antibiotics, antibiotics; P32,36 were resistant for (11), antibiotics; P14 was resistant to (9) , antibiotics; P34, P52 were resistant for (8), P4, P44,P49 were resistant to (7), P19,20,46 were resistant for (6), antibiotics P16, 26 were resistant for (5) antibiotics. Most of these tested isolates were give resistance at higher percentage for amoxicillin, nalidixic acid tetracycline, and erythromycin (Table 2).
Table (2):
Antibiotic profiling of multidrug – resistant P. aeruginosa isolates detected by using 14 different antibiotic disc
Isolates |
Resistant pattern |
No. of antibiotic that resistant for it |
|---|---|---|
P38 |
AMX, NA, ERY,MEZ, IPM, TIM, LVX,CIP,GN, CAZ, AK, TET |
12 |
P40 |
AMX,ERY, NA,CAZ, IPM,TET,LVX,TIM,GN, AK, MEZ,CIP |
12 |
P42 |
AMX,ERY, NA,CAZ, TET,IPM,TIM,LVX,GN,AK,MEZ,ATM |
12 |
P32 |
AMX, NA, CAZ,ERY, IPM, TIM, CIP,AK,GN,TET, ATM |
11 |
P36 |
AMX,NA,ERY, CAZ, IPM,TIM, LVX,CIP,TET,GN,AK |
11 |
P14 |
AMX, NA, ERY,CAZ, TMP, TET, CIP, AK, LVX, |
9 |
P34 |
AMX, ATM, MEZ, IPM, TIM, CIP,AK,GN. |
8 |
P52 |
AMX, NA, AK, MEZ, TET, CAZ, LVX, GN |
8 |
P4 |
AMX, ERY, NA, TMP, IPM, TET, MEZ |
7 |
P44 |
AMX, CAZ, MEZ,TIM,LVX,GN,IPM |
7 |
P49 |
AMX, MEZ, NA,IPM, TIM,AK,TET |
7 |
P19 |
AMX, MEM, TIM, GN, TET, IPM |
6 |
P20 |
AMX,CAZ,MEM, ATM,TIM, LVX |
6 |
P46 |
AMX,MEM,ATM,LVX,TET,IPM |
6 |
P12 |
AMX, TET, CAZ, , GN,AK |
5 |
P16 |
AMX, NA, MEM, TIM, GN |
5 |
P26 |
AMX, NA, MEM,TIM, GN,IPM |
5 |
Revealed that there were 5 (29.41%) detectable plasmid out of 17 selected multi – drug resistant P. aeruginosa isolates. Four ( 23.52%) isolates give single sized plasmid (550 – 800bp) and only one (5.88%) isolate giving double plasmids between (550-940 bp). No. P32,36 had plasmid size of (550 – 750bp) respectively while No. P38, P40 isolates were possessed plasmid size at (600 – 800bp) respectively. Only one isolate P42 have two plasmids with size from ( 550-940). The remaining 12 (70.58%) isolates were give no plasmid,
(Fig. 1).
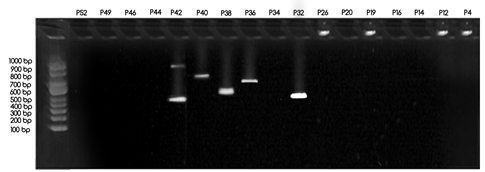
Fig. 1. Agarose gel electrophoresis showing profiles of plasmid DNA of clinical burns isolates of multi – drug resistant P. aeruginosa Lane M, (100-1000bp) ladder. No. P32, 36 had plasmid size of (550 – 750bp) respectively, while No. P38, P40 isolates were possessed plasmid size at (600 – 800bp) respectively. Only one isolate P42 have two plasmids with size from ( 550-940).
The present study was carried out for examined the susceptibility of 52 P. aeruginosa clinical burns isolates and only seventeen MDR P. aeruginosa were employed to investigate and detect the plasmid profiling.
Antibiotic susceptibility profile demonstrated that the multidrug resistance level to antibacterial has been increased in our hospitals, but was still relatively low when compared to other studies from other countries 14,15. The highest resistance to different anti- pseudomonal drugs especially among hospital strains, were documented world – wide16, and this is a major and serious therapeutic problem in the controlling and management of disease due to these bacterium. The antibacterial resistance of P. aeruginosa isolates was high in the study. The elevated and high resistance of P. aeruginosa isolates was expressed to amoxicillin (94.24%), followed by nalidixic acid (88.47%), tetracycline (71.16%), erythromycin (67.31%), and trimethoprim – sulfamethoxazol (61.54%) respectively.
This results were disagree with the previous local study that’s carried 17 their study documented that all P. aeruginosa isolates exhibited fall resistance to amoxicillin 100% and tetracycline 100%. But, resistance of P. aeruginosa isolates to amoxicillin and tetracycline is in agreement with previous foreign studies that’s carried out in Nijeria18, this study it has been revealed that 90% of P. aeruginosa clinical burns bacterial isolates showing resistance to amoxicillin and 70% were resistance to tetracycline. Others19 reported that the P. aeruginosa bacterium is naturally resistance to b – lactams, including tetracycline, mainly due to the low permeability of cell their wall. Such multi – drug resistance has serious uses and employees for the empiric therapy of infections caused by P. aeruginosa. Erythromycin which is traditionally available against burns had high resistance (70%) to P. aeruginosa clinical burns isolates. The high resistance percentage of P. aeruginosa to many antibacterial agents (antibiotics) was noticed in the present study this might be due to widespread or over usage and indiscriminate of these antibiotics over many decades in Baghdad hospitals.
The resistance profiling to Nalidixic acid was (90%)which compares with study carried out in Pakistan (92%) by 20, and in Nijeria (92.3%) by21. The elevated resistance percentage may have been due to spontaneous mutations in bacterial cells during treatment, thus making the target site inaccessible to nalidixic acid thereby resulting to elevation resistance against the selective action of antibiotics20.
Roose et al 22 reported that the resistance of antibiotics evolved by pathogens is a serious medical problem because of very fast turn over and wide spread of mutants strains, insusceptible of medical treatment by antibacterial agents. One strength feature in this study was P.aeruginosa isolates were giving resistance to impienem at a percentage (42.31%) .The marked increase of resistant strains to imipemen drug was observed which corresponds with recent findings by other researchers23. This can be explain by the variation and over usage of antibiotics in our hospitals.
The overall development of antibacterial resistance can be attributed to different factors like spread of trasposons or R- plasmids to various pathogens mainly due to the selective forces imposed by human because of the over usage of antibiotics. A review of the published research reveals over 40 known resistance gene to contain the nucleotide sequences associated with the site specific recombination site, these include gene encoding resistance to antiseptic, disinfectant and â – Lactamas 24. This result is disagree from a previous local researches that undertaken by17, they suggested that the resistance that’s by P. aeruginosa to imipenem antibiotic was 22 %. However, other study 25 documented that all P. aeruginosa isolates were expressed full susceptibly (100%) to Imipenem. Pseudomonas aeruginosa isolates exhibited low resistance level but show elevated level of susceptibility against amikacin (10%) and ciprofloxacin (6%). Proved to be the most therapeutic and effective antibacterial for routine use among the P. aeruginosa isolates tested in recent study. Also the previous study25 suggested that the bacterial isolates of P. aeruginosa were resistant to amikacin at (17.25%) while ciprofloxacin was at (27.59), this result was consistent with data that’s noticed by26. They reported that the resistance of isolates to amikacin was (18.6%) while to ciprofloxacin was (29.7%). These striking differences in the response of the organism to ciprofloxacin and amikacin may result from differences in patients individual immunity and previous usage to related types of antibiotic.
The relationship between certain plasmid and resistance to some antibacterial agents has been suggested previously by 27 . In our present study and by using agarose gel electrophoresis to detect and analyses plasmid it noticed that 7 (41.17%) of MDR P. aeruginosa isolates give clarified and detectable plasmid and remaining 10 ( 58.82%) show no plasmid bands. All isolates that had plasmids were showed resistant to amoxicillin, erythromycin, tetracycline, and nalidixic acid. The sizes of detectable plasmids among our P. aeruginosa burn isolates were ranged from ( 550-940 bp). This consistent with that documented by 28 in Iran detected plasmids in 39% of his MDR P. aeruginosa isolates. But elevated rate (47.4%) had been noticed by29 in Egypt. Plasmid evolved resistance to various antibiotics have been investigated by different workers and researchers 14,30.31
We suggested nationwide policy concerted and optimal prescribing strategies, including control of antibiotic usage, coupled with periodic Encouraging good hygienic measures could help crucial possible transmission of MDR P. aeruginosa infections within and outside the hospital environment
- Bisbe, J., J. M. Gatell, and J. Puig. Pseudomonas aeruginosabacteremia: univariate and multivariate analyses of factors influencing the prognosis in 133 episodes. Rev. Infect. Dis. 1988; 10: 629-635.[PubMed].
- Micek, S. T., A. E. Lloyd, D. J. Ritchie, R. M. Reichley, V. J. Fraser, and M. H. Kollef. Pseudomonas aeruginosabloodstream infection: importance of appropriate initial antimicrobial treatment. Antimicrob. Agents Chemother. 2005; 49: 1306-1311. [PMC free article] [PubMed]
- Carmeli YN, Troillet G, Eliopoulos GM, Samore MH. Emergence of antibiotic-resistant Pseudomonas aeruginosa: Comparison of risks associated with different antipseudomonal agents. Antimicrob. Agents Chemother. 1999; 3:1379-82. [PMC free article].
- Pool, K. Pseudomonas aeruginosa: a formidable and ever – present adversary. J. Hosp. Infect. 2011; 73:338-44.
- Caemeli, Y.N.; Eliopoulos, G.M. and Samore, M.H. ” Antecedent treatment with different antibiotic agents’. Emerg. Infect.Dis., 2002; 8: 802-807.
- National Nosocomial Infection Surveillance System. Am J Infect Control, 2004, 32: 470-485.
- Araque M, Velazco E, Int Care Med, 1998, 24(8) :839-844.
- Magiorakos AP. Multidrug Resistant (MDR), Extensively Drug Resistant (XDR) and Pandrug-1 Resistant (PDR) bacteria in healthcare settings. Expert Proposal for a Standardized International Terminology, 2011. Available online at www.escmid.org.
- Livermore, D.M. Multiple mechanisms of antimicrobial resistance in Pseudomonas vaeruginosa: Our worst nightmare? CID. Antimicrobial Resistance. 2004; 34: 634-664.
- Bukholm, G.; Tannas, T.; Kjelsberg, AB. and Smith – Erichsen, N. An outbreak of multidrug – resistant Pseudomonas aeruginosa associated with increased risk of patient death in an intensive care unit. Infect. Control. Hosp. Epidemiol. 2002; 23: 441-446.
- Bauer, A.W.; Kirby, W.M.; Sherris, J.C. and M. Truck. Antibiotic susceptibility testing by a standard single disc method. American Journal Clinical Pathology, 1966; 45:493-496.
- National Committee for Clinical Laboratory Standard ( NCCLS). (2007). Performance standards for antimicrobial susceptibility testing: twelfth informational supplement. NCCLS document M100-S12.PA, USA.
- Clinical and Laboratory Standards Institute (CLSI). (2008). Performance standards for antimicrobial disk and dilution susceptibility tests for bacteria isolated from animals; Approved Standard -Third edition, CLSI document M31-A3, Clinical and Laboratory Standards Institute, 940 West Valley Road, Wayne Pennsylvania, USA, 28:1-99.
- Yimaz, A.; Cobian, A.Y.; Yelz, Y.; Tamverdi, C.; Yidrim, T.T.; Erturan, Z.Z.; Dunipnar, B.B. and Bozdogan, B.B. Investigation of Plasmid Mediated quinolone resistance in Pseudomonas aeruginosa strains isolated from cystic fibrosis patients. Microbiol. Bull., 2011; 45: 602-608.
- Daini, O.A. and Charles – Onyeaghala, C.G. Plasmid- mediated aminoglycoside resistance of clinical isolates of Pseudomonas aeruginosa. Global Advanced Research Journal of Microbiology. 2012; 1: 052-056.
- Arora, D.; Jindal, N.; Kumar and Romit. R. Emerging antibiotic resistance in Pseudomonas aeruginosa. Int. J. Pharm .Pharm. Sci. 2011; 3(2):4-82
- Mohammed, F. Al- Marjani; Makarim, A. Khalil; Zina, H .Jzar and Zaid, N. Hassan. Detection of multidrug resistant Pseudomonas aeruginosa isolates producing IMP-1 metall-â lactamase in some Baghdad hospitals. Tikrit J. Pure. Sci. 2010; 15(1): 1662-1813.
- Akinade, O.A.; Balogun, S.A.; Ojo, D.A.; Afolabi, R.O. Motayo, B.O.; Okerentugba, P.O. and Okonko, I.O. Plasmid profile analysis of multidrug resistant Pseudomonas aeruginosa isolated from wound infections in south west, Nigeria. J. World Appl. Sci. 2012; 20(6): 775-766.
- Li, X.Z., Livermore, D.M. and Nikaido, H. Role of efflux pump(s) in intrinsic resistance of Pseudomonas aeruginosa: resistance to tetracycline, chloramphenicol and norfloxacin. Antimicrob Agents Chemother, 1994; 38(8): 1732-1741.
- Zaman, R.; Inam, M. and Ahmed, B. Sensitivity pattern of Pseudomonas. aeruginosa isolates to quinolones. J. Rawal Med. 2013; 38(3): 244-248.
- Jonthan, O. Isibor and Courage Uwabor. Antibiotic susceptibility pattern and plasmid profiles of Pseudomonas aeruginosa isolated from some hospital patients in Benin city, Nigeria. New York Sci.J. 2015; 8 (7).
- Roos, v.; Schembri, M.A.; Ulett, G.C. and Klemm, P. Asymptomatic bacteriuria Echerichia coli coli strain 83972 carriers mutations in the locus and is unable to express F1C fimbriae. Microbiology. 2006; 152:1799-1806. [PubMed].
- Akiyoshi, T.K.; Intentsu, O.; Toyoko, I. and Sachiko G. An epidemiological study of the susceptibility and frequency of multiple – drug resistant strains of Pseudomonas aeruginosa. J. Infect. Chemother. 2005; 11(2): 64.
- Lee, B.; Haagensen, J.; Ciofu, O.; Andersen, A.J.; and Molins. J.B Heterogencity of biofilms formed by non-mucoid Pseudomonas aeruginosa isolates from patients with cystic fibrosis. J. Clin. Microbiol. 2013; 43(10): 5247-5255.
- Anil, CH. And Shahid, R.M. Antimicrobial susceptibility patterns of Pseudomonas aeruginosa clinical isolates at a tertiary care hospital in Kathmandu, Nepal. Asian j. Pharm. Clin. Reas. 2013; 6(3).
- Koirala, P.; Bhatta, D.R.; Ghimire, P.; Pokhrel, B.M. and Devkota, U. Bacteriological profile of tracheal aspirates of the patients attending a neuro-hospital of Nepal. Int J Life Sci. 2010; 4: 60- 65.
- Ferguson, D.; Cahillo, J. and Quilty B. Phenotypic, molecular and antibiotic resistance profiling of nosocomial Pseudomonas aeruginosa strains isolated from two Irish hospitals 2007.
- Nikbin, V.S.; Abdi-Ali, A.; Feizabadi, M.M. and Gharavi, S. “ Pulsed field gel electrophoresis and plasmid profile of Pseudomonas aeruginosa at two hospitals in Tehran, Iran”. Indian J Med. Res., 2007; 126: 146-151.
- Mahmoud, A.B.; Zahran, W.A.; Hindawi, G.R.; Labib, A.Z.; Galal, R. Prevalence of multidrug – resistant Pseudomonas aeruginosa in patients with nosocomial infections at a university hospital in Egypt, with special reference to typing methods. J. Virol. Microbiol. 2013; 10-13.
- Shahid, M. and Malik, A. (2004). Plasmid mediated Amikacin resistance in clinical isolates of Pseudomonas aeruginosa. J. India. Med.Microb. 22: 181-184.
- Daini, O.A.; Effiong, M.J. and Ogbolu, O.D. (2008). Quinolones resistance and R – plasmids of clinical isolates of Pseudomonas aeruginosa species. J.Sudan.M.Sci. 3: 139-146.
© The Author(s) 2018. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.


