ISSN: 0973-7510
E-ISSN: 2581-690X
Like elsewhere around the globe, SARS-CoV-2 infection is spreading in rural Egypt. Due to high sensitivity and specificity, the gold standard of diagnostics is reverse transcription polymerase chain reaction PCR (RT-PCR). Rural areas without access to certified laboratories cannot take advantage of RT-PCR testing, and thus are dependent upon rapid antigen testing, a point-of-care test that requires less training and can produce results within 15 minutes. Rapid antigen testing can give an advantage to medical teams in rural settings by affording effective and early control of SARS-CoV-2 infection spread. We sought to assess the contribution of different COVID-19 testing procedures in rural Egypt. We conducted a prospective cohort study in a rural lab in Giza, Egypt. Approximately 223 individuals with potential SARS-CoV-2 infection were involved in the study during the pandemic peak in Giza, Egypt, from March 4 – May 30, 2021. Subjects were subjected to RT-PCR and rapid antigen testing, and the performance of each testing procedure was compared. Between March 4 – May 30, 2021, approximately 223 symptomatic individuals were included in this study. 190 patients (85.2%) were indicated as PCR positive for SARS-CoV-2, while 33 (14.8%) were PCR negative. In comparison, a rapid antigen test showed 178 out of 223 patients (79.8%) were indicated as positive, or 94% of the PCR-positive individuals. In Giza, a rural area of Egypt, RT-PCR had an optimal balance of sensitivity and specificity, however, the turnaround time was a limiting factor. Antigen testing, performed as a rapid point-of-care test, can play an effective role in rural outbreak control due to its ease of use and rapid results.
SARS-CoV-2, COVID-19, Antigen Testing, Rural, RT-PCR
Coronavirus disease 2019 (COVID-19) is an infectious disease induced by Coronavirus type 2 that causes Severe Acute Respiratory Syndrome (SARS-CoV-2). Effective infection control hinges, in part, on early diagnosis and isolation of infected individuals, and quarantining and testing of close contacts is of great value.1
The emergence of COVID-19 in Egypt, and its swift progression, has made rapid detection of confirmed cases, and identification of close contacts through contact tracing vital to community-based infection control.2 RT-PCR and Rapid Antigen tests are the main confirmatory tests used in the diagnosis of SARS-CoV-2 but other tests can help as non- contrast chest CT along with some blood tests as D-dimer or serum ferritin which are not confirmatory but may only suggest as they can be misdiagnosed in other diseases. Based on nucleic acid detection, the RT-PCR approach to SARS-CoV-2 testing has developed into a highly-sensitive and specific method.3 It detects positive or negative cases with no variants detection and although RT-PCR is used for consistent and effective detection of SARS-CoV-2 infection, a significant disadvantage of RT-PCR is the possibility of false results.4 Thus, a negative result does not completely rule out COVID-19. The sensitivity of RT-PCR may be inadequate since the viral load is less than the limit of detection during the initial phases of COVID-19, or due to technical difficulties such as sampling errors.5 Additionally, rural communities that lack access to facilities that can run RT-PCR tests may experience delayed reporting of results.
Antigen tests have been identified as diagnostics that are capable of rapidly distinguishing those who are infected from those who are not. Although less sensitive than molecular techniques that identify viral RNA, antigen tests are particularly useful in identifying infection in individuals with a substantial viral load in their upper respiratory tract. Because the test takes only 15 minutes to complete, it is a cost-effective, quick, and safe point-of-care diagnostic.6 Although the sensitivity of antigen tests is less than that of molecular approaches, effectiveness and short turnaround time are important considerations for controlling viral transmission.7
Another important consideration involves the process of specimen collection. RT-PCR specimen collection is invasive and runs the risk of hemorrhage for the patient. It also elevates the risk of SARS-Co-V-2 transmission to healthcare professionals. On the other hand, saliva specimen extraction is a non-invasive procedure that can be performed safely and with lower risk of SARS-CoV-2 infection to healthcare personnel,8 comparison between both methods shown in Table 1.
Table (1):
Comparison between PCR and Antigen rapid test.
RT-PCR |
Rapid antigen test |
|
|---|---|---|
Procedure |
Invasive |
Non-invasive |
Technique |
Molecular |
Antigen reaction |
Detection |
RNA genetic material |
Proteins tat are part of the virus |
Target |
Diagnose and rule out active coronavirus |
Rapid diagnose of active coronavirus |
Time |
Hours to days |
15min |
Accuracy |
Gold standard |
Positive result are confirmatory but negative result have to be repeated by RT-PCR |
Sensitivity |
High (Especially during first week) |
Low (may be high during second week) |
Specificity |
High May help in asymptomatic patients |
Needs confirmation in asymptomatic patients |
Seroconversion |
No |
Yes |
Groups |
Benefit in large group of patients |
Small group of patients |
Operator error |
High if not well trained |
Low |
The purpose of this study was to understand the accuracy of RT-PCR and rapid antigen testing as diagnostic tools used in viral detection in Giza, Egypt.
This was a prospective cohort study conducted in a lab in rural Giza, Egypt between March 4 – May 30, 2021. Approximately 223 individuals with suspected SARS-CoV-2 were subjected to RT-PCR and rapid antigen tests.
Patients
Study subjects included those with dyspnea, fever, and respiratory symptoms including cough and sore throat. A nasopharyngeal or oropharyngeal swab was collected from each individual and evaluated for the existence of SARS-CoV-2. If the initial RT-PCR result was negative, a second RT-PCR was conducted within 48-hours of visible symptoms and the absence of an alternative diagnosis. Subjects were male and female, between 23 and 75 years of age, residents of rural areas of Giza, Egypt, with clinical signs and symptoms of SARS-CoV-2 infection. We excluded asymptomatic individuals and those who refused to sign a consent or otherwise declined to be part of the study.
Molecular Technique: RT-PCR
The RT-PCR assay was used to establish the presence of SARS-CoV-2 in the laboratory. To begin, RNA was isolated from clinical specimens. The DiaPlexQTM Novel Coronavirus (2019-nCoV) Detection Kit is an in-vitro testing reagent for the qualitative detection of SARS-CoV-2 ORF1a and the N gene by Multiplex OneStep qRT-PCR. RNA was obtained from nasopharyngeal swabs utilizing the QIAamp Viral RNA Mini Kit (QIAGEN catalog # 52904 or 52906). 140 was the suggested starting volume for specimens. RNA was extracted from the samples according to the manufacturer’s guidelines for use (Roche). The Roche kit required the addition of 310L of pre-aliquoted External Lysis Buffer to a 140L sample (total input sample volume was 450L). All extracted RNA was eluted in a final volume of 60L. Parallel to each batch of patient samples, an External Positive Control was used to monitor RNA recovery, and served as a control for reverse transcription. Analysis and results were reported after analysis of the amplicon formation and calculated cut-off value.
Rapid Antigen Test
COVID19 Ag was used to identify SARS-CoV-2 antigen using the PCL COVID-19 GOLD SALIVA test pattern according to the manufacturer’s guidelines. Membrane technology dependent on colloidal gold nanoparticles and monoclonal antibodies was used in this experiment. Monoclonal antibodies were immobilized in the test region of the nitrocellulose membrane. When a sample comprised an antigen-specific for SARS-CoV-2, it was bound to the conjugate (COVID19 antibody-gold conjugate) to form a complex, moved along the nitrocellulose membrane by capillary principle, and immobilized with the COVID19 antibody in the test region. Antigen-antibody immune responses form double complexes that appear in the color band. Regardless of the presence or absence of SARS-CoV-2 antigen in the sample, the color band remained in the control zone of the product.
Nasopharyngeal Swab Specimen Procedure Rapid Ag Test
Nasopharyngeal swabs have been validated with the PCL COVID19 Ag Rapid Gold. The sampling swab was inserted through the nostril or mouth and gently pushed into the posterior nasopharynx or oropharynx. The sampling swab was rotated three times before the swab was removed. The swab was then put in the extraction buffer tube for immediate use.
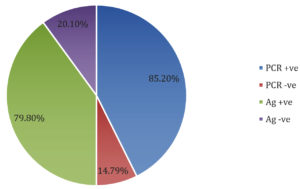
Out of 223 suspected individuals, 190 were documented as PCR-positive for SARS-CoV-2 (85.2%), and about 33 (14.8%) were PCR-negative as shown in Table (2). Comparatively, 178 of the 223 (79.8%) were SARS-CoV-2 positive with the rapid antigen test (about 94% of the PCR-positive results), while 45 (20.1%) were reported negative as shown in Table 3 and Figure.
Figure. Percentage of PCR and Rapid antigen tests showing the highest prevalence for RT-PCR +ve test
Table (2):
PCR test for suspected individuals.
PCR test |
PCR positive |
PCR negative |
Total |
|---|---|---|---|
Suspected individuals |
190 (85.2%) |
33 (148%) |
223 |
Table (3):
Rapid Antigen test for suspected individuals.
Antigen test |
Antigen positive |
Antigen negative |
Total |
|---|---|---|---|
Suspected individual |
178 (79.8 %) |
45 (20.1 %) |
223 |
Coronaviruses are non-segmented, enveloped, positive-sense RNA viruses that are widely dispersed in humans and other mammals. They are members of the family Coronaviridae and the order Nidovirales.12 Improvements in SARS-CoV-2 diagnosis with easy, rapid and cost-efficient approaches are urgently required to control the COVID-19 pandemic.
Table (4):
Characteristics of the study population revealed prevalence of male to female ratio by (60%). Most patients had one or more comorbidities. Chest and pulmonary diseases showed the highest frequency followed by cardiovascular diseases and the least for malignancy followed by hepatic diseases.
| Characteristics of the study population | |
|---|---|
| Gender | |
| Male | 60% |
| female | 40% |
| Comorbidity | |
| Chest Infection | 75% |
| Cardiovascular diseases | 65% |
| Hypertension | 40% |
| Renal Problems | 14% |
| DM | 12% |
| Malignancy | 10% |
| Hepatic diseases | 7% |
In the present study, as shown in Table 4; we reported the prevalence of male to female ratio were 60% to 40% which was similar to a study made by Abohamr et al.13 who reported majority was males confirmed by some studies,14,15 who suggested that male sex is a risk factor for the severity of COVID-19. It has been suggested that the sex-based difference between the circulating angiotensin-converting enzyme (ACE)-2 levels, the receptor of which was associated with intracellular penetration of SARS-CoV-2,16 or the smoking rate difference according to sex may have affected the sex difference on the severity of COVID-19. In addition, the potential association between androgen level and COVID-19 severity was suggested.17
Furthermore, we observed the highest prevalence for chest infection 75% followed by cardiovascular diseases 65% and the least was malignancies 10% followed by hepatic diseases 7% in the clinical study population characteristics which was in contrast by previous studies made by Huang et al.18 and Yang et al.19 who reported major clinical factor for cardiovascular and metabolic diseases and also in contrast with a study Abohamr et al.13 reported diabetes mellitus to be the most frequent comorbidity but in accordance with a study made by Wan et al.16 who reported chest and cardiovascular diseases as the highest frequency and this may be due to the expression of ACE-2 is increased in patients with hypertension, diabetes, and chronic obstructive pulmonary disease (COPD), these comorbidities can increase both the risk and severity of COVID-19 infection.20,21
In this study, we found that the RT-PCR test had a higher sensitivity than specificity. However, when results between PCR and rapid antigen test-positive cases were compared, the rapid antigen test detected 94% of the cases. Diagnostic accuracy findings should be regarded cautiously for a variety of reasons, one of which is the possibility of false negatives in both the Rapid Ag and PCR tests in the initial stages of COVID-19.22 Reasons for a false negative test result could be because of poor sampling technique. It may be less effective when carried out unsupervised. Sample degradation; samples may degrade when stored or while being transported. Sampling too early. Viral shedding from individuals peaks just before, or at the onset of symptoms. If samples are taken early in infection (1 to 4 days after infection) they have an increased false negative rate. Sampling too late; viral shedding declines after symptoms have peaked so at this stage of infection will show an increased false negative rate, CDC documented variant delta in this study period of time still no data on variants effects on the results so no suggested relationship occurred.23
To offset the possibility of false negatives, we incorporated multiple PCRs and meticulously documented each patient’s condition and this was in accordance with kruttgen et al.24 in which in their review they reported the diagnostic accuracy of rapid antigen test sensitivity to be higher in their population (Sensitivity:79.4%, Specificity:99.1%) and approaching the minimum WHO performance requirement. Also similar to a study made by Haimayo et al.,25 and Dinnes et al.,26 who reported that RA test-specific results are an important component of the tool set for policy decision-making, and demonstrate that judicious selection of an appropriate RA test can supply a viable alternative to RT-PCR in efforts to control the spread of disease that showed comparable sensitivity and specificity with the real-time RT-PCR assay. Thus, there is a potential use of this rapid and simple SARS-CoV-2 antigen detection test as a screening assay. In contrast to a study by Haung et al.,27 who reported The sensitivity of the rapid test was only 41.2%, and specificity was 98.4% versus RT-PCR results, whereas sensitivity was 100% compared with viral culture positivity and also in contrast to Lauer et al.,28 who concluded that sensitivity and specificity of the antigen assay is inferior to the PCR assay.
A significant benefit of the Rapid Ag test is the near-immediate accessibility of findings, 10-15 minutes after sample collection. The PCR test can take up to 8-10 hours, or even a full day to obtain samples and initiate a run, although the time could be reduced with training.29 In addition to the fast results, the advantage of the Rapid Ag test as a COVID-19 screening method is its straightforward technique, with its downside being poorer sensitivity. Despite its inadequacies, the nucleic acid test for SARS-CoV-2 gene identification, which would be more sensitive and specific than this side flow immunoassay, remains the gold standard for COVID-19 diagnostics.30
The WHO currently recommends Rapid Ag test that meet the minimum performance requirements of ≥80% sensitivity and ≥97% specificity compared with that of molecular testing, while the European center for Disease Prevention and Control suggests the use of tests with performance closer to RT-PCR, i.e., ≥90% sensitivity and ≥97% specificity. However, because the findings of our study showed similar overall sensitivity of Rapid Ag test than that recommended by the WHO and the ECDPC, the usefulness of Rapid Ag test as a replacement for molecular testing seemed to be of valuable alternative method.31
Therefore, the rapid SARS-CoV-2 antigen test can assist healthcare personnel in handling infected people more efficiently, and can be very useful in rural epidemics when there is limited accessibility to a lab facility equipped with PCR.
These recommendations will be delivered to the Department of Health in Giza, Egypt to encourage greater use of the rapid antigen testing process and thus improve access to SARS-CoV-2 testing in rural areas of Egypt where a certified lab is not available.
PCR remains the gold standard of SARS-CoV-2 testing. Although the sensitivity and specificity of the Rapid Ag test are lower than the PCR technique, using the Rapid Ag test to screen may play a critical role in responding to rural epidemics. Rapid Ag testing could be used in place of laboratory-based RT-PCR especially during the first week of infection, when viral loads are highest, and swift decision-making is critical, or when access to laboratory facilities are limited. Because antigen testing has varying degrees of sensitivity, individuals who test negative may nonetheless be affected. This study will help healthcare workers in Egypt with more effective utilization of the available tests when managing COVID-19.
ACKNOWLEDGMENTS
The authors would like to thank Members of Hayah Laboratory and All Staff Members, for their support to carry out this study.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
All authors listed have made a substantial, direct and intellectual contribution to the work, and approved it for publication.
FUNDING
None.
DATA AVAILABILITY
All datasets generated or analyzed during this study are included in the manuscript.
ETHICS STATEMENT
This article does not contain any studies with human participants or animals performed by any of the authors.
- Li H, Liua S-M, Yub X-H, Tang S-L, Tang C-K. Coronavirus disease (COVID-19): current status and future perspectives. Int J Antimicrob Agents. 2020;55(5):105951.
Crossref - Hameed K, Kushwah K, Saurabh S, Urkude H, Maurya MR, Sadasivuni KK. Smart technologies driven approaches to tackle COVID-19 pandemic. 3 Biotech. 2021;11(2):50.
Crossref - Yoo HM, Kim IH, Kim S. Nucleic Acid Testing of SARS-CoV-2. Int J Mol Sci. 2021;22(11):6150.
Crosssref - Shen M, Zhou Y, Ye J, et al. Recent advances and perspectives of nucleic acid detection for coronavirus. J Pharm Anal. 2020;33;10(2):97-101.
Crossref - Xie X, Zhong Z, Zhao W, Zheng C, Wang F, Liu J. Chest CT for typical 2019-nCoV Pneumonia: Relationship to negative RT-PCR testing. Radiology. 2020;296(2):E41-E45.
Crossref - Cerutti F, Burdino E, Milia MG, et al. Urgent need of rapid tests for SARS CoV-2 antigen detection: Evaluation of the SD-Biosensor antigen test for SARS-CoV-2. J Clin Virol. 2020;132:104654.
Crossref - Scohy A, Anantharajah A, Bodeus M, Kabamba-Mukadi B, Verroken A, Rodriguez-Villalobos H. Low performance of rapid antigen detection test as frontline testing for COVID-19 diagnosis. J Clin Virol. 2020;129:104455.
Crossref - Vaz SN, Santana DS, Netto EM, et al. Saliva is a reliable, non-invasive specimen for SARS-CoV-2 detection. Braz J Infect Dis. 2020;24(5):422-427.
Crossref - Wolfel R, Corman VM, Guggemos W, et al. Virological assessment of hospitalized patients with COVID-2019. Nature. 2020;581:465-469.
Crossref - Khandker SS, Nik Hashim NHH, Deris ZZ, Shueb RH, Islam MA. Diagnostic Accuracy of Rapid Antigen Test Kits for Detecting SARS-CoV-2: A Systematic Review and Meta-Analysis of 17,171 Suspected COVID-19 Patients. J Clin Med. 2021;10(16):3493.
Crossref - Wells CR, Pandey A, Moghadas SM, et al. Comparative analyses of eighteen rapid antigen tests and RT-PCR for COVID-19 quarantine and surveillance-based isolation. Commun Med. 2022;2:84.
Crossref - Treggiari D, Piubelli C, Caldrer S, et al. SARS-CoV-2 rapid antigen test in comparison to RT-PCR targeting different genes: A real-life evaluation among unselected patients in a regional hospital of Italy. J Med Virol. 2022;94(3):1190-1195.
Crossref - Abohamr SI, Abazid RM, Aldossari MA, et al. Clinical characteristics and in-hospital mortality of COVID-19 adult patients in Saudi Arabia. Saudi Med J. 2020;41(11):1217-1226.
Crossref - Shi Y, Yu X, Zhao H, Wang H, Zhao R, Sheng J. Host susceptibility to severe COVID-19 and establishment of a host risk score: Findings of 487 cases outside Wuhan. Crit Care. 2020;24:108.
Crossref - Jin J-M, Bai P, He W, et al . Gender differences in patients with COVID-19: Focus on severity and mortality. Front Public Health. 2020;8:152.
Crossref - Wan Y, Shang J, Graham R, Baric RS, Li F. Receptor recognition by the novel coronavirus from Wuhan: An analysis based on decade-long structural studies of SARS coronavirus. J Virol. 2020;94(7):e00127-20.
Crossref - Cai H. Sex difference and smoking predisposition in patients with COVID-19. Lancet Respir Med. 2020;8(4):E20.
Crossref - Huang I, Lim MA, Pranata R. Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia-A systematic review, meta-analysis, and meta-regression: Diabetes and COVID-19. Diabetes Metab Syndr Clin Res Rev. 2020;14(4):395-403.
Crossref - Yang J, Zheng Y, Gou X, et al. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis. 2020;94:91-95.
Crossref - Fang L, Karakiulakis G, Roth M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection. Lancet Respir Med. 2020;8(4):e21.
Crossref - Cho SI, Yoon S, Lee HJ. Impact of comorbidity burden on mortality in patients with COVID-19 using the Korean health insurance database. Sci Rep. 2021;11:6375.
Crossref - Pray IW, Ford L, D Cole, et al. Performance of an antigen-based test for asymptomatic and symptomatic SARS-CoV-2 testing at two university campuses.Wisconsin, September-October 2020. MMWR Morb Mortal Wkly Rep. 2021;69(51/52):1642-1647.
- Lee J, Song JU, Shim SR. Comparing the diagnostic accuracy of rapid antigen detection tests to real time polymerase chain reaction in the diagnosis of SARS-CoV-2 infection: A systematic review and meta-analysis. J Clin Virol. 2021;144:104985.
Crossref - Kruttgen A, Cornelissen CG, Dreher M, Hornef MW, Imohl M, Kleines M. Comparison of the SARS-CoV-2 Rapid antigen test to the real star Sars-CoV-2 RT PCR kit. J Virol Methods. 2021;288:114024.
Crossref - Chu VT, Schwartz NG, Donnelly MAP, et al. Comparison of Home Antigen Testing With RT-PCR and Viral Culture During the Course of SARS-CoV-2 Infection. JAMA Intern Med. 2022;182(7):701–709.
Crossref - Dinnes J, Deeks JJ, Berhane S, et al. Rapid, point-of-care antigen and molecular-based tests for diagnosis of SARS-CoV-2 infection. Cochrane Database Syst Rev. 2021;3:CD013705.
Crossref - Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497-506.
Crossref - Lauer SA, Grantz KH, Bi Q, et al. The incubation period of coronavirus disease 2019 (COVID-19) from publicly reported confirmed cases: estimation and application. Ann Intern Med. 2020.
Crossref - Malden DE, Bruxvoort KJ, Tseng HF, et al. Distribution of SARS-CoV-2 Variants in a Large Integrated Health Care System. California, March-July 2021. MMWR Morb Mortal Wkly Rep. 2021;70:1415-1419.
Crossref - European centre for disease prevention and control, options for the use of rapid antigen tests for COVID-19 in the EU/EEA and the UK. 2021
- World Health Organization (WHO). COVID-19 target product profiles for priority diagnostics to support response to the COVID-19 pandemic. 2021;v.1.0.
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.