ISSN: 0973-7510
E-ISSN: 2581-690X
Antimicrobial stewardship (AMS) and appropriate infection prevention practices are essential to decrease the rising trend of antimicrobial resistance (AMR). Good antimicrobial prescribing habits formed early in the medical career can make a paradigm shift in combating the menace of AMR. Scarce data is available about the knowledge and perceptions of Indian undergraduates on AMS. This study was planned to analyse the knowledge, attitude and perceptions (KAP) of Indian medical undergraduates on rational antimicrobial prescribing, so that the lacunae in the training curriculum can be identified and addressed effectively. A cross-sectional questionnaire-based survey was carried out, on the pre-final and final year medical students (6th to 9th semester) from six medical colleges across different states of India. A scoring system was used to rate the knowledge, attitude and perceptions of the respondents as poor, average, or good. A total of 1505 students (83.61%) participated in the survey. Majority of the students (81.7%) from all medical colleges favoured more education on antimicrobials and to incorporate AMS in the undergraduate curriculum through integrated teaching. The results showed that overall, 70.9% students had a “good” score for knowledge on antimicrobial use, whereas only 55% scored “good” for being confident in rational antimicrobial prescribing. Surprisingly, only 56.5% correct responses for knowledge on selection of broad-spectrum antibiotics over narrow-spectrum antibiotics were recorded in our study. Most of the students (79.9%) were conscious that irrational prescribing can result to AMR. On the other hand, 54.9% students believed that the supply of new antimicrobials would take care of AMR eventually. 78.1% of our students believed that they were confident in making the right diagnosis of infection, whereas, 63.7% of respondents believed that they were not confident in identifying the clinical scenarios where antibiotics are not required. Significant association (p<0.05) was seen for both “good” knowledge and perception scores with the higher academic semesters reflecting more clinical exposure in later in course semesters. The study has highlighted the areas of clinical weakness and dilemma regarding prescription of antimicrobials. Efforts to address these issues on basic principles of antimicrobial stewardship, is critical for laying the foundation of successful AMS program and contributing in overcoming the antimicrobial resistance. The study recommends targeted training, articulating fine details of prescribing antimicrobials with real time case scenarios through a multi-disciplinary approach. The Indian undergraduate medical curriculum needs to incorporate early well-structured training on AMS by integrating pharmacology and microbiology teaching with the clinical subjects to ensure appropriate antibiotic prescribing practices by the future prescribers.
Antimicrobial stewardship, undergraduates, curriculum, antimicrobial resistance
Antimicrobial agents are precious and different from other drugs due to their finite resources. Indiscriminate antimicrobial use has led to a global crisis of AMR. While the spread of multidrug resistant organisms (MDRO) is rampant, the pipeline for the development of new antimicrobials is dry. The only solution to combat the emergence of resistance is promotion of rational use of antimicrobials. International and national authorities have recommended implementation of multifaceted strategies promoting judicious and evidence based antimicrobial use, to control the spread of AMR.1,2 The World Health Organization states that education and training of healthcare professionals and medical students involved in antimicrobial prescribing is critical in fighting AMR.3,4
AMS is defined as “the optimal selection, dosage, and duration of antimicrobial treatment that results in the best clinical outcome for the treatment or prevention of infection, with minimal toxicity to the patient and minimal impact on subsequent resistance”.5 Traditionally, focus on AMS interventions is laid during clinical practice, after the completion of medical training, which has proved to be ineffective as the prescribing habits have already been developed.6-8 Various studies on undergraduate students have reported the requirement of further antimicrobial education during clinical training.9,10 AMS programs across the world have been developed to modify perceptions and behaviours of physicians during residency training or afterwards.11-13 However, education as well as training on AMS is likely to be more successful when started early in the medical education. This is the time when knowledge, attitude and perceptions of future practitioners are being shaped. It is critical for academia to update the undergraduate medical curriculum with special focus on good antimicrobial prescribing practices, following the basic principles of microbiology, infectious diseases and clinical pharmacology.
Several studies have been conducted on the knowledge, attitude and perception about antimicrobial prescription among medical students.14-16 However, only few studies have assessed the perceptions on AMS education and status of AMS among the Indian undergraduates. There is an urgent need to create awareness on emergence of MDRO and significance of rational antimicrobial prescribing and modifying the Indian undergraduate teaching system appropriately. This study is an attempt to generate multicentre data from various Indian medical colleges on medical student’s knowledge, attitude and perceptions regarding AMS, so that the lacunae in the training curriculum can be identified and addressed effectively. The survey aims to serve as a landmark reference, highlighting the need to revise the Indian medical curriculum, keeping at par with the evolving international standards. The study also aims to authenticate the need to integrate clinical based teaching on AMS with microbiology and pharmacology in order to inculcate rational antimicrobial prescribing practices among the future doctors.
Study Design, Population and Site
This was a cross-sectional multicentre questionnaire-based survey conducted among the Indian medical undergraduates, during May-June, 2019. The study population were the medical students of pre-final (6th, 7th semesters) and final (8th, 9th semesters) year, who have already been taught the pharmacology of antimicrobials as well as their microbiological aspect. The participants belonged to six medical colleges across six different states of India viz. Delhi, Haryana, Uttar Pradesh, Telangana, West Bengal and Assam, with three public and three private institutions, to capture diverse data involving different regions. The Hamdard Institute of Medical Sciences & Research Centre served as the coordinating centre for the study.
Questionnaire and Participation
The self-administered questionnaire was developed after literature review of comparable studies to assess the knowledge, attitude and perceptions on rational antimicrobial prescribing both quantitatively (multiple choice questions/ categorical data) and qualitatively (one word answer questions). The questionnaire was developed by a multidisciplinary team of investigators including infectious disease physician, pharmacologist, microbiologist, paediatrician and research methodologist. The questionnaire was pilot tested among 50 medical students of one of the medical colleges for readability, relevance and content validity. The reliability of the questionnaire was measured by the test-retest method (Cronbach’s co-efficient alpha 0.75)
The first section with 12 questions assessed the knowledge of the respondents about the antimicrobial use. The second section with 8 questions assessed the attitude of the students towards AMS. The third section comprising of 12 questions was an assessment of the perception of students regarding their skills acquired for rational antimicrobial prescribing.
The questionnaire was distributed and collected by the faculty members. Before the distribution the aim and significance of the study were conveyed to the students. The participants were given 35 minutes to answer. Each respondent answered the questionnaire independently without using any reference material. Participation was voluntary and responses were anonymous. No incentives were offered.
Data Analysis and Scoring
Section 1: in questions 2-11 the options “always” and “sometimes” were marked as “correct” while the options “never” and “I am not sure” were marked as “incorrect”. In the same section in question 1a and 1b the options “never” and “depending on clinical/laboratory findings” are marked “correct” while “always” and “I am not sure” are marked as “incorrect” answer. Section 2: in the Likert chart analysis the options “strongly disagree” and “disagree” were taken together as “disagree” and the options “agree” and “strongly agree” were taken together “agree”. Section 3: the answer “yes” was marked as “confident” and the answers “no” and “I am not sure” were marked as “non-confident”.
Scoring of responses on knowledge (section 1) and perceptions of rational antimicrobial prescribing (section 3) was done and categorized as poor, average or good. Section 1: a score of 1 was given to “correct” answers and 0 to “incorrect” answers. Section 3: a score of 1 was given to “confident” and 0 to “non-confident”. For both the sections a maximum score of 12 was obtained and a score of > 8 was considered as “good”. The questionnaire used and the datasets generated are available on request, however, the questions of the 3 sections are reflected in chronological order in the 3 graphical figures respectively.
Statistical Analysis
The data was analyzed in the Statistical Package for Scientific Solutions (SPSS) version 23.0. Simple descriptive statistics was used to generate frequencies, percentage and proportions. Categorical data were expressed as proportions and continuous data were expressed as mean + standard deviation. The nonparametric test (Wilcoxon-Mann-Whitney U test) were used to assess differences between groups and correlations between variables. Chi-squared test was used to explore the association between categorical data. P-value <0.05 was considered statistically significant.
A total of 1505 students from 6 medical colleges participated in the survey which corresponds to a response rate of 83.61% (1505/1800). The median age of the respondents was 22 years (interquartile range IQR 20-23 years) and 792 (52.6%) of the participants were males. Overall, 782 participants (52.0%) belonged to the pre-final year of MBBS and 723 (48%) from the final year. The percentage participation from different semesters was 25.3% for 6th semester, 15.9% for 7th semester, 21.2% for 8th semester and 11% for 9th semester. Participation from government and private institutions was 545 (36.2%) and 960 (63.8%) students respectively. Majority of the students desired to further pursue their career either in surgery (19.3%) or medicine (16.3%). The percentage participation from different states was 35.3% for Telangana, 20.1% for Uttar Pradesh, 16.3% for West Bengal, 10% for Assam, 9.9% for Haryana and 8.3% for Delhi (Table 1).
Table (1):
Demographic details of participants.
Basic Details |
Number (Percentage) |
|---|---|
Total number |
1505 |
Age |
22 years (IQR 20-23 years) |
Gender |
|
Male |
713 (47.4) |
Female |
792 (52.6) |
Semester |
|
6th |
379 (25.2) |
7th |
239 (15.9) |
8th |
319 (21.2) |
9th |
165 (11.0) |
MBBS Semester |
|
5th-6th (Pre-final) Semester |
782 (52.0) |
8th-9th (Final) Semester |
723 (48.0) |
State representation |
|
West Bengal |
246 (16.3) |
Haryana |
149 (9.9) |
Assam |
150 (10.0) |
Delhi |
125 (8.3) |
Telangana |
532 (35.3) |
Uttar Pradesh |
303 (20.1) |
Type Of College |
|
Public |
545 (36.2%) |
Private |
960 (63.8%) |
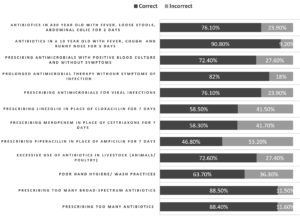
Analysis of knowledge of antimicrobial use (Fig. 1)
In section 1 of the questionnaire, 88.4% of the participants answered correctly regarding prescription of too many broad-spectrum antibiotics being the major cause of antimicrobial resistance. Knowledge on hand hygiene practices for prevention of infections was observed in 63.7% students, whereas 72.6% students acknowledged that excessive use of antibiotics in livestock also leads to antimicrobial resistance. However, in the questions assessing the knowledge of prescribing broad-spectrum antibiotics over narrow spectrum antibiotics, correct results varied between 46.8% to 58.5% among the different colleges. The fact that antibiotics have no role in viral infections was known to 76.1% of students. 82% respondents realised that prescribing prolonged empirical antimicrobial therapy without clear symptoms of infection leads to antimicrobial resistance. 90.8% students responded correctly that the most common cause of fever and upper respiratory symptoms in children were due to viral illness and did not require antibiotics. Whereas, 76.1% students knew that diarrheal infections were self-limiting with no antibiotic requirements.
Analysis of attitude towards antimicrobial stewardship (Fig. 2)
Results of section 2 revealed that 74% of the students acknowledged the fact that there is misuse of antimicrobials currently. 66% students were of the opinion that AMR was associated with increased mortality, morbidity and prolonged hospitalization. The majority of students (81.7%) agreed that further training on rational antimicrobial prescribing was required to overcome the antibiotic selection dilemmas. Once again, a high of 84.1% students supported reinforcement of antimicrobial pharmacology teaching with clinical case-based problems, whereas 73.8% students wanted integration of antimicrobial pharmacology with clinical teaching. Surprisingly, 54.9% students believed that the supply of new antimicrobials would take care of AMR eventually.
Analysis of perceptions of rational antimicrobial prescribing (Fig. 3)
Results of section 3 reflected confidence in 78.1% participants in making diagnosis of infection or sepsis, while 63.7% were confident in identifying scenarios not requiring antimicrobial therapy. In the self-assessment of the ability to select appropriate antimicrobial treatment for community acquired pneumonia, urinary tract infection, multi-drug resistant E.coli infection and drug-resistant Salmonella typhi, low confidence rates of 41.5%, 62.8%, 38.9% and 54.1% were observed respectively. Confidence in choosing the appropriate duration, route of administration and dose of antimicrobials prescribed was perceived by 69.4%, 68.2% and 61.9% students respectively. 67.8% of respondents believed that they were able to stop or deescalate antimicrobial treatment appropriately following microbiology culture reports. 68.2% students were confident for deciding the appropriate combination of antimicrobial therapy whenever required.
Scoring of knowledge and perceptions of antimicrobial stewardship
An overall “good” score for knowledge on antimicrobial use was seen in 70.9% of students whereas only 55% had an overall “good” score on perceptions of rational antimicrobial prescription. Statistical correlation of the “good” score for knowledge and perceptions with various variables including gender, MBBS semester and medical colleges was analysed (Table 2). Significant association (p<0.05) was found with higher MBBS semesters for both “good” knowledge and perception scores.
Table (2):
Factors associated with good knowledge and good perception scores.
| Factors | Good Knowledge | p-value | Good Perception | p-value |
|---|---|---|---|---|
| (n = 1067) | (n = 827) | |||
| Age (Years) | 22.01 ± 1.56 | <0.0011 | 22.10 ± 1.55 | <0.0011 |
| Gender* | 0.5322 | 0.0092 | ||
| Male | 511 (71.7%) | 417 (58.5%) | ||
| Female | 556 (70.2%) | 410 (51.8%) | ||
| Semester* | <0.0012 | <0.0012 | ||
| 4th | 175 (54.0%) | 119 (36.7%) | ||
| 5th | 56 (70.9%) | 29 (36.7%) | ||
| 6th | 281 (74.1%) | 198 (52.2%) | ||
| 7th | 221 (92.5%) | 200 (83.7%) | ||
| 8th | 210 (65.8%) | 194 (60.8%) | ||
| 9th | 124 (75.2%) | 87 (52.7%) | ||
| MBBS Semester* | <0.0012 | <0.0012 | ||
| 4th-6th (Pre-final) Semester | 512 (65.5%) | 346 (44.2%) | ||
| 7th-9th Semester (final) | 555 (76.8%) | 481 (66.5%) | ||
| State representation* | <0.0012 | <0.0012 | ||
| West Bengal | 193 (78.5%) | 90 (36.6%) | ||
| Haryana | 111 (74.5%) | 92 (61.7%) | ||
| Assam | 90 (60.0%) | 63 (42.0%) | ||
| Delhi | 93 (74.4%) | 95 (76.0%) | ||
| Telangana | 308 (57.9%) | 240 (45.1%) | ||
| Uttar Pradesh | 272 (89.8%) | 247 (81.5%) | ||
| Type Of College* | 0.3692 | <0.0012 | ||
| Government | 151 (27.7%) | 245 (45.0%) | ||
| Private | 287 (29.9%) | 582 (60.6%) |
*Significant at p<0.05, 1: Wilcoxon-Mann-Whitney U Test, 2: Chi-Squared Test.
The aim of AMS is three-fold. The first goal is to facilitate physicians to prescribe the most appropriate antimicrobials with the correct dose and duration. The second goal is to prevent antimicrobial overuse, misuse and abuse and the final goal is to minimize AMR spread. During the medical training, basics about antimicrobials and AMR are taught in pharmacology and microbiology respectively and the knowledge on the subjects is assessed. However, assuming that the knowledge of the undergraduate students on antimicrobials is adequate, it is also essential to assess their attitude as well as perception on AMS, as prescription of antimicrobials will form a major part of their practice and requires reinforcement through clinical case-based teaching and training. This is the first multicentre study conducted across various states in India; evaluating the fundamentals of AMS among the medical students. The study data revealed an overall “good” score by 70.9% participants on knowledge and 55% participants on perceptions of rational antimicrobial stewardship.
Majority of our students (82.5%) desired further education on antimicrobial prescribing. This is in accordance with the previous studies on medical students and doctors.2,10,17 Difficulty in prescribing appropriate antimicrobials in common infections and also withholding the same in certain situations is experienced by the undergraduate students when they enter into clinical practice. Thus, targeted teaching and training on antimicrobials stewardship skills will form the cornerstone for successful AMS programs18-20 81.7% of medical students in our study upheld the significance of undergraduate training on rational antimicrobial prescribing. This is similar to the study by Sharma et al; which reported a positive attitude by 98% of medical and 87% of dental students.18 Similar studies by Huang et al.14 in China, Vasundara et al.21 in India, and other studies,22,23 highlight the need for AMS education by medical students. Hence, education on the principles of AMS should start early during medical training.
The significance of clinical case-based pharmacology teaching of 2nd year medical students, simulating the complexities of ‘real-world’ decision making, has been established by many previous studies24,25 as well as by 84.1% of our participants. The major hurdle faced by contemporary medical curriculum in teaching pharmacology with simultaneous reinforcement through active clinical based problems (problem-based learning) is the ‘time constraint’.16 However, many countries such as UK and USA have revised their medical curriculum for imparting training on good antimicrobial prescribing practices at undergraduate level.7 Such initiatives in teaching rational use of antimicrobials, through clinical case-based approach in medical, dental, pharmacy as well as nursing curriculum, are much awaited in Indian education system.
The results of our study demonstrate statistically significant association between knowledge scores and higher academic course semester (p<0.05). This shows positive association with exposure to clinical postings, contrary to the report by Abbo et al.10 However, this may also indicate the significance of early exposure to the ‘infectious disease’ (ID) domain10 and further emphasize on a well-structured and standardized medical curriculum to address the areas of weakness. In India, the National Medical Council (NMC) through its revised competency based medical education (CBME) curriculum is promoting horizontal and vertical integrated teaching among various medical disciplines and provides for early clinical exposure, electives and longitudinal care,26 which again is supported by 73.8% students in our study. To standardize AMS education, teaching and learning methodology should be aided with innovative technology such as reliable open access learning sites and applications for updating information on antimicrobial use and prescribing in accordance with the current national and international guidelines.18,25
Knowledge on the role of antibiotics in viral infections was observed in 76.1% students which was further assessed by brief clinical based questions (Fig. 1) on the 2 most common scenarios of antibiotic abuse namely common cold and diarrhoea. However, only 56.5% correct responses for knowledge on selection of broad-spectrum antibiotics over narrow-spectrum antibiotics were recorded through 3 structured questions in our study (Fig. 1). Surprisingly only 63.7% students in our study had knowledge that hand hygiene is an important preventive measure against infections in the hospital, which is similar to a European study.16 These observations, similar to other studies,10,18,25 point to the need for introducing specific teaching interventions comprising of interactive clinical case-based learning. Stress should be laid on identifying irrational prescribing practices and scenarios where antimicrobials need to be withheld or combination antimicrobial therapy prescribed.
Our results on attitude of the students on antimicrobial prescribing (Fig. 2), endorse the previous observations from various studies.18,10,27 The observed differences in attitude towards antimicrobial prescribing practice can deeply affect the clinical acumen and interpretation of these future prescribers. In our study, majority of the participants (74%) agreed that a notable proportion of antimicrobial prescribing is inappropriate, similar to the US survey of doctors (62%).28 and the European study of medical students, where a greater proportion (83%) of the respondents felt the same.16 Most of the students (79.9%) in our study were conscious that irrational prescribing can result to AMR and 74% agreed on current misuse of antimicrobials, which is the ethical responsibility of the clinicians. This positive attitude could play a significant role in involving the students in stewardship interventions. Further, highlighting the successes of AMS interventions may help the young prescribers recognize that an individual change can collectively lead to significant outcomes. However, only 66% of the students believed that AMR was associated with increased mortality, morbidity and prolonged hospitalization and a low of 54.9% believe that the supply of new antimicrobials would take care of AMR eventually which can have an immense negative impact on AMS efforts.
In an effort to identify the level of perceived confidence while prescribing antimicrobials, we have observed results broadly consistent with other medical schools as well as a recent study of US students.10 Most of our students (78.1%) thought they were confident in making right diagnosis of infection; similar to a European study (92%).16 Studies have revealed ‘inaccurate diagnosis’ as the leading cause of unnecessary antibiotic use29 which may serve as one of the areas for designing educational programmes. However, the students had poor perceptions of being able to select appropriate antimicrobial treatment for common infections like community acquired pneumonia, urinary tract infection, multi-drug resistant E.coli infection and drug-resistant Salmonella typhi. Also, 63.7% of respondents believed that they were not confident in identifying the clinical scenarios where antibiotics are not required. Although, our data does not reflect an overall poor perception on AMS but the figures reflect great scope for improvement on the student confidence levels (Fig. 3). This is highly essential to upgrade the perception of self-competence translating into prompt and rational prescribing practices, once again advocating early problem-based teaching on AMS. Special attention also needs to be paid on ‘communication skills’ of the students to handle the situations of diagnostic uncertainty, which is critical to reduce the number of unnecessary prescriptions.7
The major strength of our study was its multicentre layout, capturing huge data across different states of India including both government and private sector of medical education. Other strengths include the anonymous and voluntary nature of participation, which reduces the tendency of providing “socially desirable” answers. Also, the participants were not allowed to take any help during filling the questionnaire, so the data reflects the actual KAP of the volunteers. Overall, the responses were consistent across the medical colleges for most questions, reflecting a degree of external validity. Potential limitation of our study was that no formal data on medical college curricula regarding antimicrobial use, resistance, or stewardship was collected. As with all questionnaire-based studies there was as usual the potential for recall bias. The authors would further want to assess the impact of opportunity and motivation on the prescribing practices as variables of behavioural science could also be possible limiting factors.
It can be concluded from the observations that most undergraduate students desired further education on antimicrobials during their medical education. The study recommends well-structured integration of pharmacology and microbiology teaching with the clinical trainings to strengthen AMS programs. Development of targeted educational literature and articulating fine details of prescribing antimicrobials with real time case scenarios by a multi-disciplinary team is highly recommended to overcome the clinical weaknesses and prescribing dilemmas among the medical students. Larger studies encompassing all elements of AMS with comparative analysis across different educational systems is highly recommended. This will help identify the key educational interventions and strategies at an early undergraduate level for successful implementation of AMS in Indian system.
ACKNOWLEDGMENTS
The authors would like to thank all the participated students for their contribution in this study and for providing their valuable inputs.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
AC, NN and PG have contributed to the concept and design of the article. AC, NN, PG, RB, DR, RD and NN have contributed in data collection and analysis. AC, NN and PG drafted the manuscript. All authors read and approved the final manuscript for publication.
FUNDING
None.
ETHICS STATEMENT
This study was approved by Jamia Hamdard Institutional Ethics Committee, India.
AVAILABILITY OF DATA
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
INFORMED CONSENT
Written informed consent was obtained from the participants before enrolling in the study.
- Vickers H. International antibiotic resistance crisis. Better training needed to maintain therapeutic arsenal, Student. BMJ. 2011;342:3207.
Crossref - Minen MT, Duquaine D, Marx MA, Weiss D. A survey of knowledge, attitudes, and beliefs of medical students concerning antimicrobial use and resistance. Microb Drug Resist. 2010;16(4):285-289.
Crossref - World Health Organization. The evolving threat of antimicrobial resistance: options for action. World Health Organization. 2012. https://apps.who.int/iris/handle/10665/44812
- World Health Organization. Anti-Infective Drug Resistance Surveillance and Containment Team. WHO global strategy for containment of antimicrobial resistance. World Health Organization. 2001. https://apps.who.int/iris/handle/10665/66860
- Gerding DN. The search for good antimicrobial stewardship. Jt Comm J Qual Improv. 2001;27(8):403-404.
Crossref - Akici AGM, Goren MZ, Aypak C, Terzioglu B, Oktay S. Prescription audit adjunct to rational pharmacotherapy education improves prescribing skills of medical students. Eur J Clin Pharmacol. 2005;61(9):643-650.
Crossref - Pulcini C, Gyssens IC. How to educate prescribers in antimicrobial stewardship practices. Virulence. 2013;4(2):192-202.
Crossref - Humphreys H, Dillane T, O’Connell B, Luke LC. Survey of recent medical graduates’ knowledge and understanding of the treatment and prevention of infection. Ir Med J. 2006;99(2):58-59. PMID: 16548226
- Dyar OJ, Howard P, Nathwani D, Pulcini C . Knowledge, attitudes, and beliefs of French medical students about antibiotic prescribing and resistance. Medecine Mal Infect. 2013;43(10):423-430.
Crossref - Abbo LM, Cosgrove SE, Pottinger PS, et al. Medical students’ perceptions and knowledge about antimicrobial stewardship: how are we educating our future prescribers? Clin Infect Dis. 2013;57(5):631-638.
Crossref - Roumie CL, Halasa NB, Edwards KM, Zhu Y, Dittus RS, Griffin MR. Differences in antibiotic prescribing among physicians, residents, and nonphysician clinicians. Am J Med. 2005;118(6):641-648.
Crossref - Running A, Kipp C, Mercer V. Prescriptive patterns of nurse practitioners and physicians. J Am Acad Nurse Pract. 2006;18(5):228-233.
Crossref - Edgar T, Boyd SD, Palame MJ. Sustainability for behaviour change in the fight against antibiotic resistance: a social marketing framework. J Antimicrob Chemother. 2009;63(2):230-237.
Crossref - Huang Y, Gu J, Zhang M, et al. Knowledge, attitude and practice of antibiotics: a questionnaire study among 2500 Chinese students. BMC Med Educ. 2013; 13:163.
Crossref - Thriemer K, Katuala Y, Batoko B, et al. Antibiotic prescribing in DR Congo: a knowledge, attitude and practice survey among medical doctors and students. PloS One. 2013;8(2):e55495.
Crossref - Dyar OJ, Pulcini C, Howard P, et al. European medical students: a first multicentre study of knowledge, attitudes and perceptions of antibiotic prescribing and antibiotic resistance. J Antimicrob Chemother. 2014;69(3): 842-846.
Crossref - Abbo L, Sinkowitz-Cochran R, Smith L, et al. Faculty and resident physicians’ attitudes, perceptions, and knowledge about antimicrobial use and resistance. Infect Control Hosp Epidemiol. 2011;32(7):714-718.
Crossref - Sharma K, Jain P, Sharma A. Knowledge, attitude and perception of medical and dental undergraduates about antimicrobial stewardship. Indian J Pharmacol. 2015;47(6):676-679.
Crossref - MacDougall C, Polk RE. Antimicrobial stewardship programs in health care systems. Clin Microbiol Rev. 2005;18(4):638-656.
Crossref - Sbarbaro JA. Can we influence prescribing patterns? Clin Infect Dis. 2001;33(Suppl 3):S240-244.
Crossref - Vasundara K, Kanchan P, Pundarikaksha HP, Girish K, Prassana S, Jyothi R. An imperative need to change pharmacology curriculum: A pilot survey. Indian J Pharmacol. 2010;42(6):420.
Crossref - Giblin TB, Sinkowitz-Cochran RL, Harris PL, et al. Clinicians’ perceptions of the problem of antimicrobial resistance in health care facilities. Arch Intern Med. 2004;164(15):1662-1668.
Crossref - Ross S, Loke YK. Do educational interventions improve prescribing by medical students and junior doctors? A systematic review. Br J Clin Pharmacol. 2009;67(6):662-670.
Crossref - Gupta K, Arora S, Kaushal S. Modified case-based learning: Our experience with a new module for pharmacology undergraduate teaching. Int J Appl Basic Med Res. 2014;4(2):90-94.
Crossref - Pulcini C, Wencker F, Frimodt-Moller N, et al. European survey on principles of prudent antibiotic prescribing teaching in undergraduate students. Clin Microbiol Infect. 2015;21(4):354-361.
Crossref - Medical Council of India. Competency based Undergraduate curriculum for the Indian Medical Graduate. 2018;1:136-159.
- Issue with supplement: Davey P, Garner S. Professional education on antimicrobial prescribing: A report from the Specialist Advisory Committee on Antimicrobial Resistance (SACAR) Professional Education Subgroup. J Antimicrob Chemother. 2007;60(Suppl 1):i27-32.
Crossref - Charani E, Cooke J, Holmes A. Antibiotic stewardship programmes-what’s missing? J Antimicrob Chemother. 2010;65(11):2275-2277.
Crossref - Pulcini C, Cua E, Lieutier F, Landraud L, Dellamonica P, Roger PM. Antibiotic misuse: a prospective clinical audit in a French university hospital. Eur J Clin Microbiol Infect Dis. 2007;26(4):277-280.
Crossref
© The Author(s) 2022. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.