ISSN: 0973-7510
E-ISSN: 2581-690X
Toxoplasmosis poses significant risks to pregnant women and their unborn children. The study aimed at assessing the prevalence and analyzing the risk factors associated with T. gondii infection among pregnant women in Taiz City, Yemen. 400 randomly recruited pregnant women were tested for T. gondii antibodies (IgM and IgG) by enzyme immunoassay. Bio- and socio-demographic data were gathered using a validated questionnaire, completed during face-to-face interviews. Univariate and multivariate analyses were performed to determine the independent variables associated with T. gondii seroprevalence. The study population had an average age of 26 years, with most participants in the second trimester. A significant proportion of participants reported living in rural areas and had exposure to animals, particularly cats. The seroprevalence of Toxoplasma gondii infection stands at a notable 36% with 24.5% positive for IgG antibodies only, 1.8% positive for IgM antibodies while, 9.7% positive for IgG and IgM antibodies. The study found a significant association between T. gondii seroprevalence and a history of miscarriage, households with unimproved water sources and ownership of cats in the household. Multivariate analysis confirmed that participants who lived in households with unimproved water sources and those who owned cats were significantly more likely to have T. gondii seroprevalence. This study highlights a substantial seroprevalence of T. gondii infection among pregnant women in Taiz City, Yemen, emphasizing the importance of implementing preventive measures. Promoting access to safe drinking water, advocating for hygiene practices, and raising awareness are essential to mitigate the burden of toxoplasmosis in pregnant women.
T. gondii Infection, Pregnant Women, Seroprevalence, Risk Factors, Toxoplasmosis, Maternal Health, Child Health
Toxoplasma gondii can infect humans and animals including mammals and birds,1 with cat serving as the definitive host. Human infection occurs through ingestion of food or water contaminated with sporulated oocysts excreted in cat feces, consumption of undercooked meat containing tissue cysts, or, less frequently, via contaminated needles, blood transfusion, organ transplantation, or vertical transmission.2-4
The global infection rate of T. gondii is over 30%, but varies widely by region, from 10%-90%.5 For most healthy individuals, this often presents no symptoms but can be severe in immunocompromised persons. The most serious concern is congenital toxoplasmosis resulting from primary infection during pregnancy, which can lead to congenital anomalies, neurological and ocular complications, miscarriage, or stillbirth.6,7 Higher prevalence is reported among pregnant women in specific regions especially in impoverished countries across Africa and selective regions of the Middle East,8 influenced by environmental, behavioral, socio-demographic, and obstetric risk factors, including consumption of raw or undercooked meat, unprotected water sources, direct contact with cats, and history of adverse pregnancy outcomes.9-13
Diagnostic methods for T. gondii infection include serological assays, molecular techniques, and clinical evaluations. Serological assays detecting IgM and IgG antibodies are widely used for screening and diagnosis.14 However, interpreting the results is complicated by long term persistence of IgM and lifelong IgG (at low level),15-17 prompting the introduction of IgG avidity testing to distinguish previous from current infections, and avoid false positive results of IgM testing.18-20 Despite these limits, IgM/IgG detection remains the most widely used initial screening method,21,22 with newer assays employing recombinant antigens showing promise for improved accuracy.23
Yemen, a country facing numerous healthcare challenges exacerbated by ongoing conflict and limited resources, is particularly vulnerable to infectious diseases24 such as toxoplasmosis. Previous studies in Yemen reveal varying rates of T. gondii infection among pregnant women ranging from 14.4%-64.3% across different regions of the country, but most studies were geographically restricted, based on small samples, or lacked multivariate analysis to adequately assess risk factors.12,13,25-29 Given Yemen’s diverse geographic conditions and variation in hygiene/cultural practices across regions, it is unclear whether the findings from prior localized research can be generalized nationwide.
Toxoplasmosis remains a neglected infection in Yemen, as it is not part of the regular screening tests for pregnant women. This study aimed to investigate the seroprevalence of T. gondii infection among pregnant women in Taiz city, Yemen, and explore the associated risk factors. By examining environmental exposures, demographic characteristics, and obstetric histories, we seek to identify determinants of T. gondii infection in this population. Through this research, we endeavor to contribute to the evidence base for informed decision-making and the development of targeted interventions to prevent and control T. gondii infection in pregnant women, ultimately improving maternal and child health outcomes in Yemen and beyond.
Study design and setting
A cross-sectional study was carried out in Taiz, Yemen, from October 2023 to February 2024. Data were collected using a pre-tested questionnaire first developed in English and translated into Arabic. Pregnant women attending routine antenatal visits underwent standard clinical assessments, including physical examination, history-taking, laboratory testing, and ultrasound.
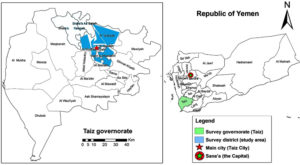
Taiz is a densely inhabited city in Yemen and rises at about 1,400 meters above the Red Sea (Figure). It has minimal seasonal temperature variation (20-30 °C) and moderate humidity (40%-60%).30 This study was conducted in a maternal and child health facility serving around 10,000 patients annually, selected for its accessibility and comprehensive antenatal services.
Study population and sampling
Participants were pregnant women seeking antenatal care. The sample size (n = 400) was determined using the WHO formula for health studies,31 based on a 46.2% previously reported toxoplasmosis prevalence.26 Every pregnant woman present on the day of recruitment was eligible for inclusion, ensuring a representative sample from the target population, and random selection was utilized to minimize selection bias and enhance the generalizability of the study findings.
Data collection procedures
Trained healthcare professionals conducted interviews and gathered pertinent data. Training included standardized instruction on questionnaire administration, specimen collection, and confidentiality procedures. A standardized questionnaire was utilized to gather data on the participants’ age, gestational age, educational level, employment status, household water sources, animal husbandry, and khat chewing habits, i.e., chewing the green leaves of the Catha edulis shrub for social and psychological purposes, a common practice in Yemen and East Africa. Water sources were classified as improved or unimproved following UNICEF/WHO Joint Monitoring Program for Water Supply and Sanitation.32
Serological analysis
Antibodies against T. gondii were analyzed using an electrochemiluminescence immunoassay (ECLIA) on the fully automated Elecsys immunoassay analyzer (Roche Diagnostics, Mannheim, Germany), employing recombinant antigens (SAG1, GRA1, GRA7). IgG and IgM positivity was defined as a signal/cutoff of >1.0. Reported sensitivities and specificities were 100%/99.8% for IgG and 96.7%/99.8% for IgM.33,34 Quality control included manufacturer-provided controls and retesting of samples suspected of prozone effect. This ECLIA method has been well validated for toxoplasmosis screening and showed excellent agreement with reference immunofluorescence and ELISA methods.35
Ethical considerations
Ethical approval was obtained from the Faculty of Medicine and Health Sciences, Taiz University (IRB-2023-05-12). Written informed consent was secured from all participants, and confidentiality was maintained throughout the study.
Characteristics of the study population
This study involved 400 pregnant women aged 15-46 years, with an average age of 26 years (interquartile range: 21-31 years). Gestational age was distributed as follows: 26.5% in the first trimester, 38.3% in the second trimester and 35.3% in the third trimester. In addition, about 26.2% of the participants had no formal education. In addition, 66% and 48.5% of the women stated that they kept animals and had cats in the household, respectively. 37.3% (149/400) of the women reported a spontaneous abortion in the past. Furthermore, the majority of pregnant women had access to unimproved water sources (61.8%, 247/400), as shown in Table 1.
Table (1):
Characteristics of study participants in Taiz, Yemen (N = 400)
| Characteristics | N (%) |
|---|---|
| Age groups (years) | |
| 15-29 | 180 (45) |
| ≥30 | 220 (55) |
| Number of children | |
| <3 | 146 (36.5) |
| ≥3 | 254 (63.5) |
| Gestational age | |
| First trimester | 106 (26.5) |
| Second trimester | 153 (38.3) |
| Third semester | 141 (35.3) |
| Residence | |
| Urban | 152 (38) |
| Rural | 248 (62) |
| Education | |
| Primary school or above | 295 (73.8) |
| No formal education | 105 (26.2) |
| History of spontaneous abortion | |
| No | 251 (62.75) |
| Yes | 149 (37.3) |
| Employment | |
| Employed | 217 (54.2) |
| Unemployed | 183 (45.8) |
| Type of household water source | |
| Improved | 153 (38.2) |
| Unimproved | 247 (61.8) |
| Rearing animals | |
| No | 136 (34) |
| Yes | 264 (66) |
| Having cats at home | |
| No | 206 (51.5) |
| Yes | 194 (48.5) |
Associated risk factors and seropositivity of T. gondii
In the study, a general seroprevalence of anti-T. gondii antibodies (IgG and/or IgM) was found in 36% (144/400) of pregnant women. Specifically, 24.5% (98/400) showed reactivity to IgG antibodies only, 9.7% (39/400) showed reactivity to IgG and IgM antibodies, and 1.8% (7/400) showed reactivity to IgM antibodies only. Chi-square test was employed in identifying the factors associated with T. gondii seropositivity.
As shown in the Chi-square analysis (Table 2), a significant association was found between T. gondii infection and a history of spontaneous abortion in pregnant women (OR = 1.61, 95% CI = 1.06-2.45, P = 0.026). Similarly, pregnant women living in households without access to improved water sources had more than double the risk of T. gondii infection than those who had access to improved water sources (OR = 2.53; 95% CI = 1.61-3.96, P = 0.001). In addition, the risk of T. gondii infection was more than 1.7 times higher in pregnant women who keep cats at home than in women who do not have cats at home (OR = 1.70; 95% CI = 1.13-2.57, P = 0.011). However, the study found no statistically significant association between T. gondii infection and the participants’ gestational age (P = 0.135), age group, employment and education status, number of children, history of blood transfusions, handling of fresh meat, and pet ownership.
Table (2):
Bivariate analysis of factors associated with seroprevalence of toxoplasmosis (N = 400)
| Variables | Toxoplasma seroprevalence | |||
|---|---|---|---|---|
| N participants | N (%) | COR (95% CI) | P-value | |
| Age groups (years) | ||||
| 15-29 | 180 | 56 (31.1) | 1 | 0.065 |
| ≥30 | 220 | 88 (40.0) | 0.68 (0.45-1.03) | |
| Number of children | ||||
| <3 | 146 | 61 (41.8) | 1 | 0.068 |
| ≥3 | 254 | 83 (32.7) | 0.68 (0.44-1.03) | |
| Education | ||||
| Primary school or above | 295 | 111 (37.6) | 1 | 0.256 |
| No formal education | 105 | 33 (31.4) | 0.76 (0.47-1.22) | |
| Employment | ||||
| Employed | 183 | 58 (31.7) | 1 | 0.099 |
| Unemployed | 217 | 86 (39.6) | 0.71 (0.47-1.06) | |
| Gestational age | ||||
| First trimester | 106 | 46 (43.4) | 1 | |
| Second trimester | 153 | 50 (32.7) | 0.63 (0.38-1.05) | 0.080 |
| Third trimester | 141 | 48 (34.0) | 0.67 (0.40-1.13) | 0.135 |
| History of spontaneous abortion | ||||
| No | 251 | 80 (31.9) | 1 | 0.026* |
| Yes | 149 | 64 (43.3) | 1.61 (1.06-2.45) | |
| Residence | ||||
| Urban | 152 | 61 (40.1) | 1 | 0.178 |
| Rural | 248 | 83 (33.5) | 0.75 (0.49-1.14) | |
| History of blood transfusion | ||||
| No | 223 | 83 (37.2) | 1 | 0.568 |
| Yes | 177 | 61 (34.5) | 0.89 (0.59-1.34) | |
| Type of household water source | ||||
| Improved | 153 | 36 (23.5) | 1 | 0.001* |
| Unimproved | 247 | 108 (43.7) | 2.53 (1.61-3.96) | |
| Handling fresh meat | ||||
| No | 131 | 41 (31.3) | 1 | 0.172 |
| Yes | 269 | 103 (38.3) | 0.73 (0.47-1.14) | |
| Rearing animals | ||||
| No | 136 | 56 (41.2) | 1 | 0.122 |
| Yes | 264 | 88 (33.3) | 0.714 (0.47-1.09) | |
| Having cats at home | ||||
| No | 206 | 62 (30.1) | 1 | 0.011* |
| Yes | 194 | 82 (42.3) | 1.70 (1.13-2.57) | |
COR: Crude Odds ratio; CI: Confidence interval; *: Significant association (P < 0.05)
A multivariate logistic regression analysis was performed to investigate the association between the seroprevalence of T. gondii infection and possible risk factors. Variables entered into the multiple logistic regression were history of spontaneous abortion, lack of access to improved water sources, and having cats at home. The results showed that lack of access to improved water sources (AOR = 2.65; 95% CI = 1.68-4.17, P = 0.001), and the presence of cats in the house (AOR = 1.65; 95% CI = 1.08-2.51, P = 0.021) were significant independent risk factors for T. gondii infection (Table 3).
Table (3):
Multivariable analysis of factors associated with seroprevalence of toxoplasmosis in pregnant women (N = 400)
| Variables | AOR | 95% CI | P–value |
|---|---|---|---|
| History of spontaneous abortion | |||
| No | 1 | ||
| Yes | 0.742 | 0.26-0.65 | 0.184 |
| Type of household water source | |||
| Improved | 1 | ||
| Unimproved | 2.65 | 1.68-4.17 | 0.001* |
| Having cats at home | |||
| No | 1 | ||
| Yes | 1.65 | 1.08-2.51 | 0.021* |
Toxoplasmosis can be fatal and lead to long-term complications, especially if it is congenital or occurs in immunocompromised individuals.36 The findings underscore the significance of understanding the epidemiology of T. gondii infection, given its potential for severe consequences, especially in congenital cases or among immunocompromised individuals.
Overall, the prevalence of T. gondii infection in this study was 36%, which is lower compared to previous studies conducted in different parts of Yemen.13,25-27 For example, in the rural community of Taiz governorate, 46.2% (166/359) of pregnant women were seropositive for T. gondii infection.26 In Aden governorate in southern Yemen, 64.3% (431/670) of those who were pregnant and sought care at private clinics and hospitals were also seropositive.29 However, a recent study of 90 pregnant women in the Hodeida governorate reported a lesser prevalence (14.4%) of T. gondii infection.
The rate of seropositivity observed in this study aligns with previous findings conducted in Sudan (34.1%) and Tobago (39.3%).37,38 In contrast, Lebanon (82.6%) and Ethiopia (85.3%) reported a higher seroprevalence rate.39,40 In addition, Saudi Arabia (8.3%), Zambia (5.9%) and Sri Lanka (12.3%) exhibited a lower rate of seropositivity for the infection than the rates revealed in the current study.41-43 Several studies indicates that the seroprevalence of T. gondii infection varies significantly by country, region and community and may be influenced by factors such as diet, socioeconomic status, culture, water quality, and sanitation.10,44
The study’s result revealed 11.5% of the pregnant women tested had IgM antibodies. Of these, 9.7% detected positive for both anti-T. gondii IgM and IgG antibodies, while 1.8% tested positive for IgM antibodies only. These results align with the outcomes of earlier studies on pregnant women in Dhamar governorate.12 However, it was reported that the seroprevalence of anti-T. gondii IgM antibodies was lower in pregnant women living in a rural community in Taiz, southern Yemen.26 When the Toxoplasma IgM antibodies are present with negative IgG antibodies, this may suggest early infection, but the concurrent detection of IgM and IgG antibodies indicates acute infection. In the present study, however, these results were not confirmed by seroconversion tests and/or IgG avidity tests. It is important to note that the detection of IgM antibodies cannot definitely confirm an acute Toxoplasma infection, as IgM antibodies can remain positive for up to two years in chronic infections.14
The results of the study suggest that, in accordance with previous global studies, history of miscarriage and feline exposure were significant independent predictors of T. gondii infection.45-47 Consistent with prior global research, the study results indicate that a history of miscarriage and exposure to felines were the key factors linked with infection by T. gondii,45-47 which has a causal link to miscarriages in the first trimester and IgM seropositivity.48 In addition, domestic cats are known to be a source of contamination with T. gondii sporocyst.49 Furthermore, based on the univariate analysis, a statistically significant association between toxoplasmosis and the use of unimproved drinking water sources among participants in Taiz. Pregnant women who used unimproved drinking water sources were about twice as likely to be infected as those who used improved sources. This observation aligns with the report from rural communities in Taiz, which demonstrated a remarkable association between the high prevalence of T. gondii infection and the consumption of unimproved drinking water.26
The age of the participants, their level of education, place of residence, employment status, number of children, handling of fresh meat, history of blood transfusion and presence of animals (except cats) in the household did not significantly affect the seroprevalence of known T. gondii infection in the present study. These findings are consistent with those from other researches.50,51 In contrast, consumption of untreated water is generally not considered a significant risk factor for T. gondii in pregnant women in Dhamar, Yemen.12 The differences in the results are possibly due to the differing climatic conditions in the Dhamar district and Taiz governorate in Yemen. Dhamar, which is situated in the mountains, has a colder and drier climate, while Taiz has a warmer and more humid climate. The warm and humid environment in Taiz could provide a more favorable atmosphere for the oocysts of T. gondii to remain infectious longer in the water, which could explain the higher incidence of infection compared to Dhamar.9
This study has some limitations that should be acknowledged. As a hospital-based cross-sectional analysis, we could not determine causality or the time of infection. This may limit the depth of understanding regarding the factors influencing T. gondii infection, hence cautious consideration is needed when interpreting the results and generalizing findings. To mitigate these limitations, future research endeavors should prioritize longitudinal cohort and community-based designs, incorporate avidity testing and direct detection methods like PCR, and broaden recruitment strategies to encompass a more diverse participant pool. These approaches would enhance the validity and generalizability of findings, thus providing a more comprehensive understanding of T. gondii infection dynamics among pregnant women in Taiz city, Yemen, and facilitating the development of targeted interventions to mitigate its impact on maternal and child.
The study suggests that 36% of pregnant women interviewed in Taiz city had evidence of previous exposure to T. gondii infection indicating a substantial number of women were exposed to the parasite. Further analysis revealed two key risk factors associated with infection: lack of access to improved water sources and presence of cats in households. Identifying these risk factors may help in the development of public health strategies to avert and control T. gondii infection in pregnant women. Promoting safe drinking water sources, encouraging good hygiene practices, and providing education about the risks linked to handling cats and contact with their feces are recommended measures to decreased the risk of T. gondii infection in pregnant women.
ACKNOWLEDGMENTS
None.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
TA, JCA, JD, RH, ARA, FDH, IA and CPC conceptualized the study. TA and IA performed data collection. TA, JCA, JD, RH, ARA, FDH, IA and CPC applied methodology. TA, JCA, JD, RH, ARA and FDH performed formal analysis. TA, JCA and IA performed visualization. TA, JCA, JD, RH, ARA, FDH, IA and CPC performed validation. TA and JCA performed project administration. TA, JCA, JD, RH, IA and CPC wrote the manuscript. All authors read and approved the final manuscript for publication.
FUNDING
None.
DATA AVAILABILITY
All datasets generated or analyzed during this study are included in the manuscript.
ETHICS STATEMENT
This study was approved by the Institutional Ethics Committee, Faculty of Medicine and Health Sciences, Taiz University, Taiz, Yemen (IRB-2023-05-12).
INFORMED CONSENT
Written informed consent was obtained from the participants before enrolling in the study.
- Centers for Disease Control and Prevention, Parasites: Toxoplasmosis. CDC, 2024. https://www.cdc.gov/parasites/toxoplasmosis/index.html Accessed 30 Nov 2024
- Munoz-Roldan M, Heimesaat MM, Liesenfeld O. 48 – Toxoplasmosis, In: Farrar J, Hotez PJ, Junghanss T, Kang G, Lalloo D, White NJ (eds), Manson’s Tropical Infectious Diseases 23th Eds., London: W.B. Saunders. 2014:652-663.e1.
- Alvarado-Esquivel C, Sanchez-Anguiano LF, Hernandez-Tinoco J, et al. Association between Toxoplasma gondii infection and history of blood transfusion: a case-control seroprevalence study. Int J Med Res. 2018;46(4):1626-1633.
Crossref - Vueba AN, Faria CP, Almendra R, Santana P, Sousa MDC. Serological prevalence of toxoplasmosis in pregnant women in Luanda (Angola): Geospatial distribution and its association with socio-demographic and clinical-obstetric determinants. PLoS One. 2020;15(11):e0241908.
Crossref - Mao F, Yang Y, Chen Y, et al. Seroprevalence and Risk Factors of Toxoplasma gondii Infection Among High-Risk Populations in Jiangsu Province, Eastern China. Front Cell Infect Microbiol. 2021;11:783654.
Crossref - Wang ZD, Liu HH, Ma ZX, et al. Toxoplasma gondii Infection in Immunocompromised Patients: A Systematic Review and Meta-Analysis. Front Microbiol. 2017;8:389.
Crossref - Villar BBDLF, Neves EDS, Louro VC, et al. Toxoplasmosis in pregnancy: a clinical, diagnostic, and epidemiological study in a referral hospital in Rio de Janeiro, Brazil. Braz J Infect Dis. 2021;24(6):517-523.
Crossref - Torgerson PR, Mastroiacovo P. The global burden of congenital toxoplasmosis: a systematic review. Bull World Health Organ. 2013;91(7):501-508.
Crossref - Yan C, Liang LJ, Zheng KY, Zhu XQ. Impact of environmental factors on the emergence, transmission and distribution of Toxoplasma gondii. Parasit Vectors. 2016;9:137.
Crossref - Pappas G, Roussos N, Falagas ME. Toxoplasmosis snapshots: global status of Toxoplasma gondii seroprevalence and implications for pregnancy and congenital toxoplasmosis. Int J Parasitol. 2009;39(12):1385-1394.
Crossref - Condoleo R, Rinaldi L, Sette S, Mezher Z. Risk Assessment of Human Toxoplasmosis Associated with the Consumption of Pork Meat in Italy. Risk Anal. 2018;38(6):1202-1222.
Crossref - Al-Adhroey AH, Mehrass AAKO, Al-Shammakh AA, Ali AD, Akabat MYM, Al-Mekhlafi HM. Prevalence and predictors of Toxoplasma gondii infection in pregnant women from Dhamar, Yemen. BMC Infect Dis. 2019;19(1):1089.
Crossref - Al-Eryani SM, Al-Mekhlafi AM, Al-Shibani LA, Mahdy MM, Azazy AA. Toxoplasma gondii infection among pregnant women in Yemen: Factors associated with high seroprevalence. J Infect Dev Ctries. 2016;10(6):667-672.
Crossref - Zhang K, Lin G, Han Y, Li J. Serological diagnosis of toxoplasmosis and standardization. Clin Chim Acta. 2016;461:83-89.
Crossref - Liu Q, Wang ZD, Huang SY, Zhu XQ. Diagnosis of toxoplasmosis and typing of Toxoplasma gondii. Parasit Vectors. 2015;8(1):292.
Crossref - Dhakal R, Gajurel K, Pomares C, Talucod J, Press CJ, Montoya JG. Significance of a Positive Toxoplasma Immunoglobulin M Test Result in the United States. J Clin Microbiol. 2015;53(11):3601-5.
Crossref - Robert-Gangneux F, Darde ML. Epidemiology of and diagnostic strategies for toxoplasmosis. Clin Microbiol Rev. 2012;25(2):264-296.
Crossref - Candolfi E, Pastor R, Huber R, Filisetti D, Villard O. IgG avidity assay firms up the diagnosis of acute toxoplasmosis on the first serum sample in immunocompetent pregnant women. Diagn Microbiol Infect Dis. 2007;58(1):83-88.
Crossref - Murat JB, L’ollivier C, Hidalgo HF, Franck J, Pelloux H, Piarroux R. Evaluation of the new Elecsys Toxo IgG avidity assay for toxoplasmosis and new insights into the interpretation of avidity results. Clin Vaccine Immunol. 2012;19(11):1838-1843.
Crossref - Villard O, Breit L, Cimon B, et al. Comparison of four commercially available avidity tests for Toxoplasma gondii-specific IgG antibodies. Clin Vaccine Immunol. 2013;20(2):197-204.
Crossref - Hajissa K, Zakaria R, Suppian R, Mohamed Z. Design and evaluation of a recombinant multi-epitope antigen for serodiagnosis of Toxoplasma gondii infection in humans. Parasit Vectors, 2015;8(1):315.
Crossref - Murat JB, Hidalgo HF, Brenier-Pinchart MP, Pelloux H. Human toxoplasmosis: which biological diagnostic tests are best suited to which clinical situations? Expert Rev Anti Infect Ther. 2013;11(9):943-956.
Crossref - Sonaimuthu P, Fong MY, Kalyanasundaram R, Mahmud R, Lau YL. Sero-diagnostic evaluation of Toxoplasma gondii recombinant Rhoptry antigen 8 expressed in E. coli. Parasit Vectors. 2014;7(1):297.
Crossref - Alzubiery TKA, Alhazari T, Alcantara JC, Majed SA, Bazaid AS, Aldarhami A. Updated Seroprevalence of Hepatitis B Surface Antigen and Anti-Hepatitis Core Antibody Among Blood Donors in Yemen. Infect Drug Resist. 2022;15;2787-2796.
Crossref - Arwa A, Hmamouch A, Amayour A, Marc I, El Kharrim K, Belghyti D. Epidemiology of toxoplasmosis among married women at birth age in Sana’a City (Yemen). Int J Innov Sci Res. 2015;19(1);40-48.
- Mahdy MAK, Alareqi LMQ, Abdul-Ghani R, et al. A community-based survey of Toxoplasma gondii infection among pregnant women in rural areas of Taiz governorate, Yemen: the risk of waterborne transmission. Infect Dis Poverty. 2017;6(1):26.
Crossref - Saif N, Al-Ameeri G, Alhweesh M, Alkadasi M, Zaid AA. Sero prevalence of toxoplasmosis in pregnant women in Taiz-Yemen. Int J Curr Microbiol Appl Sci. 2014;3(7):680-690.
- Ashraf M, Abdul-Haleem S. Seroprevalence of Anti Toxoplasma gondii IgG and IgM Among Pregnant Women in Sana’a Capital and Capital Trusteeship. Sci J King Faisal Univ. 2010;11(2):1431.
Crossref - Muqbil NA, Alqubatii MA. Seroprevalence of toxoplasmosis among women in Aden city, Yemen. Arch Biomed Sci. 2014;2(2):42-50.
- Alharazi T, Alcantara JC, Dando LL, Pangket P. Seroprevalence of toxoplasmosis at referral hospitals in the northwestern region, Saudi Arabia. J Educ Health Promot. 2023;12(1):391.
Crossref - Althubaiti A. Sample size determination: A practical guide for health researchers. J Gen Fam Med. 2022;14;24(2):72-78.
Crossref - World Health Organization. Regional Office for South-East Asia (2010). Joint monitoring programme for water supply and sanitation, : report on intercountry workshop, Jakarta, Indonesia, 27-29 April 2009. WHO Regional Office for South-East Asia. https://iris.who.int/handle/10665/205410 Accessed 30, Jan 2025
- Marques BA, Andrade GMQ, Neves SPF, Pereira FH, Talim MCT. Systematic review of serological methods used in prenatal screening for toxoplasmosis inpregnant women. Rev Med Minas Gerais. 2015;25(Suppl 6):S68–S81.
Crossref - Firouz ZE, Kaboosi H, Nasiri AF, Tabatabaie SS, Golhasani-Keshtan F, Zaboli FA. Comparative serological study of toxoplasmosis in pregnant women by CLIA and ELISA methods in Chalus City, Iran. Iran Red Crescent Med J. 2014;16(4):e15115.
Crossref - Prusa AR, Hayde M, Unterasinger L, Pollak A, Herkner KR, Kasper DC. Evaluation of the Roche Elecsys Toxo IgG and IgM electrochemiluminescence immunoassay for the detection of gestational Toxoplasma infection. Diagn Microbiol Infect Dis. 2010;68(4):352-357.
Crossref - Fouladvand M, Barazesh A, Naeimi B, Zandi K, Tajbakhsh S. Seroprevalence of toxoplasmosis in high school girls in Bushehr city South-west of Iran. Afr J Microbiol Res. 2010;4(11):1117-1121.
- Elnahas A, Gerais AS, Elbashir MI, Eldien ES, Adam I. Toxoplasmosis in pregnant Sudanese women. Saudi Med J. 2003;24(8):868-870.
- Ramsewak S, Gooding R, Ganta K, Seepersadsingh N, Adesiyun AA. Seroprevalence and risk factors of Toxoplasma gondii infection among pregnant women in Trinidad and Tobago. Rev Panam Salud Publica. 2008;23(3):164-170.
Crossref - Abamecha F, Awel H. Seroprevalence and risk factors of Toxoplasma gondii infection in pregnant women following antenatal care at Mizan Aman General Hospital, Bench Maji Zone (BMZ): Ethiopia. BMC Infect Dis. 2016;16(1):460.
Crossref - Nahouli H, El Arnaout N, Chalhoub E, Anastadiadis E, El Hajj H. Seroprevalence of Anti-Toxoplasma gondii Antibodies Among Lebanese Pregnant Women. Vector Borne Zoonotic Dis. 2017;17(12):785-790.
Crossref - Alharazi T. Prevalence and risk factors of intestinal parasitic infections among pregnant women in Taiz Governorate, Yemen: A hospital-based study. Helminthologia. 2023;26;60(3):201-207.
Crossref - Chandrasena N, Herath R, Rupasinghe N, et al. Toxoplasmosis awareness, seroprevalence and risk behavior among pregnant women in the Gampaha district, Sri Lanka. Pathog Glob Health. 2016;110(2):62-67.
Crossref - Frimpong C, Makasa M, Sitali L, Michelo C. Seroprevalence and determinants of toxoplasmosis in pregnant women attending antenatal clinic at the university teaching hospital, Lusaka, Zambia. BMC Infect Dis. 2017;17(1):10.
Crossref - Fan CK, Lee LW, Liao CW, et al. Toxoplasma gondii infection: relationship between seroprevalence and risk factors among primary schoolchildren in the capital areas of Democratic Republic of Sao Tome and Prםncipe, West Africa. Parasit Vectors. 2012;5:141.
Crossref - Awoke K, Nibret E, Munshea A. Sero-prevalence and associated risk factors of Toxoplasma gondii infection among pregnant women attending antenatal care at Felege Hiwot Referral Hospital, northwest Ethiopia. Asian Pac J Trop Med. 2015;8(7):549-554.
Crossref - Gebremedhin EZ, Tadesse G. A meta-analysis of the prevalence of Toxoplasma gondii in animals and humans in Ethiopia. Parasit Vectors. 2015;8:291.
Crossref - Halonen SK, Weiss LM. Toxoplasmosis. Handb Clin Neurol. 2013;114:125-145.
Crossref - Dubey JP. Oocyst shedding by cats fed isolated bradyzoites and comparison of infectivity of bradyzoites of the VEG strain Toxoplasma gondii to cats and mice. J Parasitol. 2001;87(1):215-219.
Crossref - Kassie E, Kebede N, Kassa T, et al. Seroprevalence and risk factors for Toxoplasma gondii infection among pregnant women at Debre Markos Referral Hospital, northwest Ethiopia. Trans R Soc Trop Med Hyg. 2024;2;118(1):61-68.
Crossref - Alvarado-Esquivel C, Pacheco-Vega SJ, Hernandez-Tinoco J, et al. Miscarriage history and Toxoplasma gondii infection: A cross-sectional study in women in Durango City, Mexico. Eur J Microbiol Immunol. 2014;4(2):117-122.
Crossref - Alvarado-Esquivel C, Pacheco-Vega SJ, Hernandez-Tinoco J, et al. Seroprevalence of Toxoplasma gondii infection and associated risk factors in Huicholes in Mexico. Parasit Vectors. 2014;7(1):301.
Crossref
© The Author(s) 2026. Open Access. This article is distributed under the terms of the Creative Commons Attribution 4.0 International License which permits unrestricted use, sharing, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.